Pituitary Anatomy & Physiology - Gland Central
- Location: Sella turcica (sphenoid bone), covered by diaphragma sellae.
- Lobes & Origin:
- Adenohypophysis (Anterior Lobe): From Rathke's pouch (oral ectoderm).
- Hormones: GH, PRL, ACTH, TSH, FSH, LH. (📌 FLAT PiG)
- Blood: Superior hypophyseal artery (hypophyseal portal system).
- Neurohypophysis (Posterior Lobe): From neuroectoderm (diencephalon downgrowth).
- Stores: ADH (vasopressin), Oxytocin (produced in hypothalamus: Supraoptic & Paraventricular nuclei).
- Blood: Inferior hypophyseal artery.
- Adenohypophysis (Anterior Lobe): From Rathke's pouch (oral ectoderm).
- Key Relations:
- Superior: Optic chiasm (compression → bitemporal hemianopia).
- Lateral: Cavernous sinuses (contains CN III, IV, V1, V2, VI; Internal Carotid Artery).
- Inferior: Sphenoid sinus (transsphenoidal surgical approach).

⭐ The cavernous sinus, lateral to the pituitary, contains CN III, IV, V1, V2, VI and the ICA. Lateral pituitary expansion can cause ophthalmoplegia and sensory loss in V1/V2 distributions.
Indications & Pre-op Eval - Surgical Summons
- Indications:
- Pituitary Adenomas:
- Functioning: Cushing's, Acromegaly, Prolactinoma (med-refractory)
- Non-Functioning: Mass effect (visual loss, hypopituitarism), apoplexy
- Other lesions: Craniopharyngioma, Rathke's Cleft Cyst (symptomatic), Sellar/Parasellar tumors.
- Pituitary Adenomas:
- Pre-op Evaluation (📌 Mnemonic: HOME):
- Hormonal: Full pituitary panel; dynamic tests prn.
- Ophthalmological: Visual acuity, fields (perimetry).
- MRI: Sellar region (gold standard); CT for bony detail.
- Endoscopy (Nasal): For transsphenoidal approach.
- General fitness (ASA) & detailed counselling.

⭐ Bitemporal hemianopia is a classic visual field defect in pituitary adenomas due to optic chiasm compression.
Surgical Approaches - The Sellar Gateway
- Transsphenoidal Approach (TSA): Primary route for >95% of pituitary tumors.
- Types:
- Endoscopic Endonasal (EEA): Gold standard. Superior visualization, wider surgical corridor.
- Microscopic: Traditional, still used.
- Corridors: Transnasal (most common), sublabial (historical), transseptal.
- Advantages: Minimally invasive, direct midline access, no external scar, ↓ hospital stay, ↓ morbidity.
- Key Complications: CSF leak (most common, ~5-15%), meningitis, diabetes insipidus (DI), sinusitis, vascular injury (ICA).
⭐ The most feared complication of TSA is injury to the internal carotid artery (ICA).
- Types:
- Transcranial Approach (TCA): Reserved for select cases.
- Indications: Large/giant adenomas with significant lateral (cavernous sinus) or anterior/posterior fossa extension, non-adenomatous sellar pathology, failed TSA.
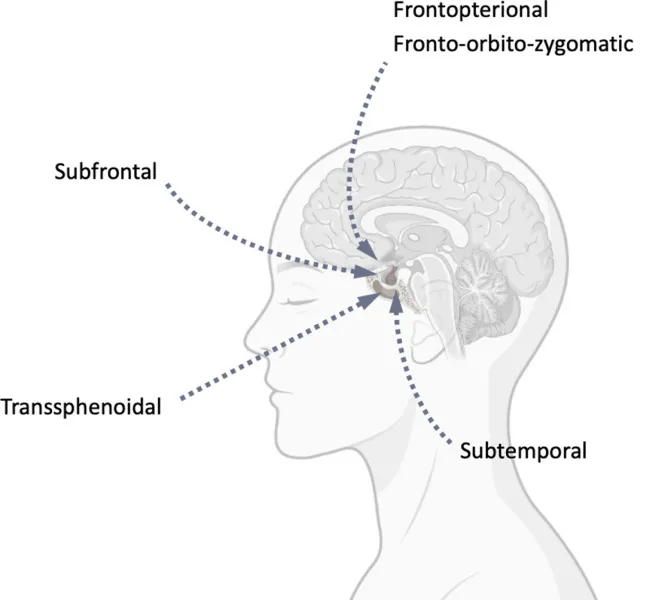
- Routes: Pterional, subfrontal, orbitozygomatic.
- Disadvantages: More invasive, brain retraction, higher risk of neurological deficits, longer recovery.
Complications & Post-op Care - Pituitary Pitfalls
- Immediate/Early:
- CSF Leak: Most common. β2-transferrin test. Manage: bed rest, drain, repair if >5-7 days.
- Hemorrhage: Sellar hematoma. Risk of vision loss.
- Visual loss: Optic nerve/chiasm injury.
- CN Palsy: III, IV, VI; often transient.
- Endocrine:
- DI: ↓ADH. Polyuria (>250ml/hr), ↑Na+ (>145 mEq/L), ↓Urine Osm (<300 mOsm/kg). Rx: DDAVP.
- SIADH: ↑ADH. Oliguria, ↓Na+ (<135 mEq/L), ↑Urine Osm. Rx: Fluid restriction.
- Hypopituitarism: ACTH/TSH deficiency common. Lifelong replacement.
- Other: Meningitis, nasal septal issues.
- Post-op Care:
- Monitor: UO, Serum Na+, vision.
- Nasal pack (2-5 days). Avoid straining/nose blowing.
- Stress-dose steroids (Hydrocortisone).
⭐ CSF rhinorrhea is the most common complication. Beta-2 transferrin is pathognomonic for CSF.
High‑Yield Points - ⚡ Biggest Takeaways
- Transsphenoidal approach: gold standard for most pituitary adenomas.
- Endoscopic endonasal approach: improved visualization, wider access, reduced morbidity.
- Key complications: CSF leak, diabetes insipidus (DI), SIADH, meningitis, visual loss, hypopituitarism.
- Prolactinomas: most common, often medically managed (dopamine agonists: cabergoline/bromocriptine).
- GH-adenomas cause acromegaly/gigantism; ACTH-adenomas cause Cushing's disease.
- Non-functioning adenomas: present with visual defects (bitemporal hemianopia) or hypopituitarism.
- Post-op MRI: assesses resection completeness, sellar integrity.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

