LSB Approaches: Overview - Entry Points Unveiled
- Definition: Surgical corridors to access lesions in the lateral skull base, involving temporal bone and adjacent areas.
- Goals:
- Maximal safe tumor removal.
- Preservation of neurological function (cranial nerves, brainstem).
- Watertight dural closure.
- Key Indications:
- Vestibular schwannomas.
- Glomus jugulare tumors.
- Petroclival meningiomas.
- Extensive cholesteatomas.
- Core Principles:
- Adequate bony unroofing for exposure.
- Early neurovascular identification & preservation.
- Meticulous hemostasis.
⭐ A key objective of LSB surgery is maximal safe resection with preservation of neurological function.
LSB Surgical Anatomy - Danger Zones & Landmarks
- Temporal Bone:
- Mastoid: Air cells, sigmoid sinus.
- Petrous Apex: ICA, CN VI.
- Critical Structures (Danger Zones):
- CN VII (Facial): Complex temporal bone course.
- CN VIII (Vestibulocochlear): With CN VII in IAM.
- ICA (Internal Carotid Artery): Petrous segment.
- Sigmoid Sinus & IJV (Internal Jugular Vein).
- Key Foramina & Contents:
| Foramen | Contents |
|---|---|
| Internal Auditory Meatus | CN VII, CN VIII, Labyrinthine a. |
| Jugular Foramen | CN IX, X, XI, IJV |
| Hypoglossal Canal | CN XII |
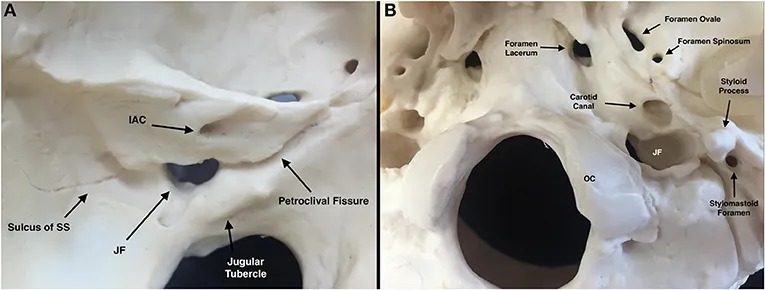
⭐ The facial nerve's intricate course through the temporal bone is a critical consideration in all lateral skull base approaches.
Key Lateral Approaches - Surgical Pathway Prowess
Lateral skull base surgery demands precise anatomical knowledge and tailored approaches. Key factors: tumor type/location, extent, hearing status.
| Approach | Indication (Hearing/Tumor) | Corridor | Pro | Con | Risk |
|---|---|---|---|---|---|
| Translabyrinthine | VS (poor hearing: PTA >50dB, SDS <50%) | Transmastoid, via labyrinth | Direct CPA, no cerebellar retract | Sacrifices hearing, CSF leak | CN VII |
| Retrosigmoid (RS) | VS (good hearing), CPA tumors | Suboccipital, post. sigmoid | Hearing pres. possible | Cerebellar retract, limited ant. reach | CN V, VII-XI |
| Middle Cranial F. | Small lat. IAC VS (good hearing, <1.5cm intra-canal) | Supratemporal, extradural | Best lat. IAC, hearing pres. | Temporal lobe retract, limited CPA | CN VII, GSPN, cochlea |
| Infratemporal F. | Glomus jugulare, extensive infralab./petroclival lesions | Below EAC (Types A,B,C) | JF, lower clivus, ICA access | Complex, CN VII/IX-XII risk, cond. HL | CN VII, IX-XII, ICA |
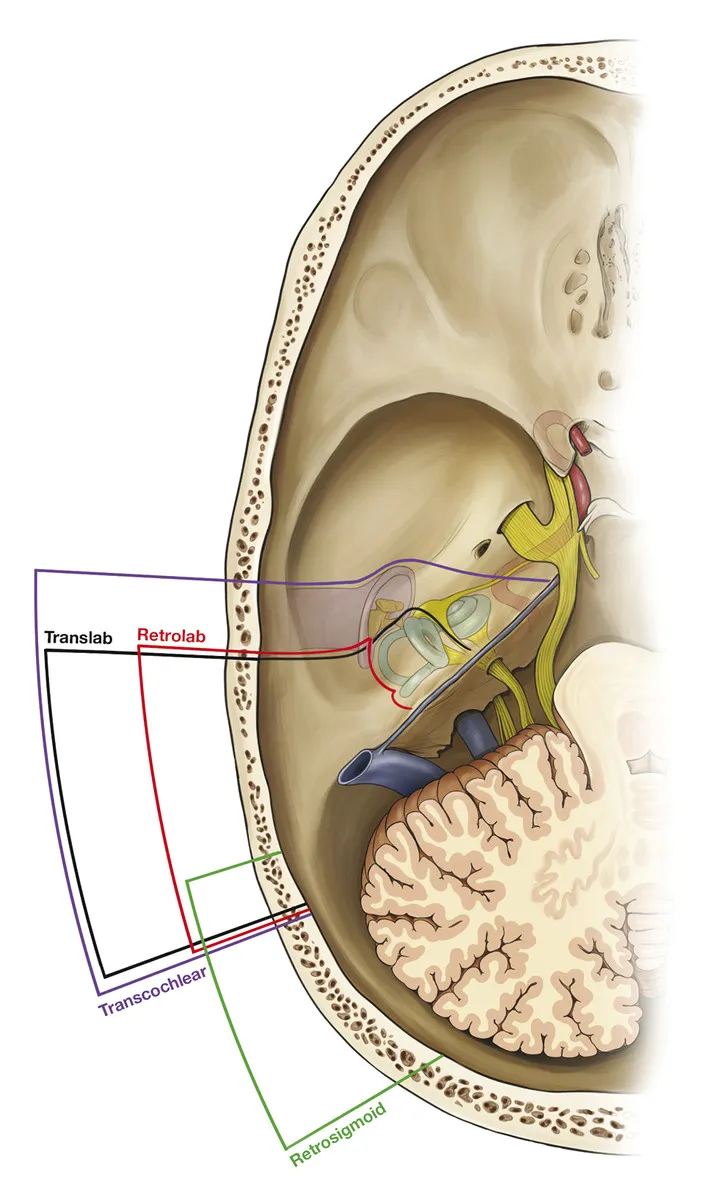
Decision-making often follows this simplified pathway:
LSB Complications - Post-Op Pitfall Patrol
- CSF Leak: Common. Management: Bed rest, lumbar drain, surgical repair.
- Facial Nerve Palsy: Assess with House-Brackmann grading (Grade I-VI). Management: Steroids, physiotherapy, surgical decompression/repair if indicated.
- Hearing Loss: Conductive or sensorineural. Management: Hearing aids, cochlear implants.
- Vertigo: Usually transient. Management: Vestibular suppressants, rehabilitation.
- Infection (Meningitis): Prophylactic antibiotics. Management: IV antibiotics.
- Vascular Injury (ICA, Sigmoid Sinus): Rare but critical. Management: Intraoperative repair, endovascular stenting.
- Lower Cranial Nerve Deficits (IX, X, XI, XII): Swallowing assessment, speech therapy.
- Wound Complications: Hematoma, infection. Management: Drainage, antibiotics.
⭐ CSF leak is a common complication; meticulous dural closure and use of prophylactic measures like lumbar drains are crucial for prevention and management.
High‑Yield Points - ⚡ Biggest Takeaways
- Transmastoid approaches are key for posterior fossa & petroclival lesions.
- Infratemporal fossa (ITF) approaches provide access to middle fossa, parasellar, & nasopharyngeal regions.
- Facial nerve (CN VII) management (mobilization, rerouting, grafting) is paramount in all lateral approaches.
- Critical structures at risk include Internal Carotid Artery (ICA), jugular bulb, and lower cranial nerves (IX-XII).
- Preventing CSF leak with meticulous dural closure and skull base reconstruction is vital.
- Hearing preservation is a significant consideration, often balanced against complete tumor removal.
- Preoperative embolization is crucial for highly vascular tumors like glomus jugulare or paragangliomas to reduce intraoperative bleeding.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

