AOM: Definition & Epidemiology - Ear's Achey Breaky Start
- Definition: Acute inflammation of the middle ear; rapid onset of signs/symptoms (e.g., otalgia, fever, irritability).
- Epidemiology:
- Peak incidence: 6 to 24 months.
- One of the most common childhood infections.
- Key risk factors: recent URI, daycare attendance, pacifier use, formula feeding, exposure to tobacco smoke.
⭐ Most cases of AOM occur in children aged 6 to 24 months.
AOM: Etiology & Pathophysiology - Bug Invasion
- Key Pathogens:
- Bacteria: S. pneumoniae (most common), H. influenzae (non-typable), M. catarrhalis. 📌 Sad Hot Mess
- Viruses: RSV, Rhinovirus, Influenza (often precede).
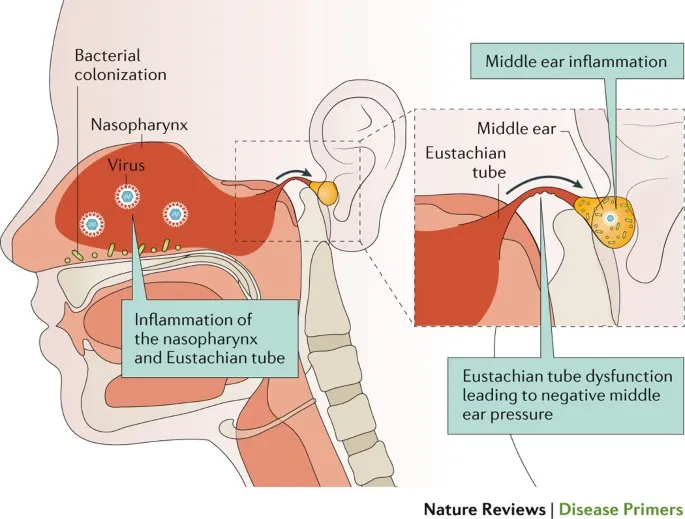
- Pathophysiology:
- Eustachian Tube Dysfunction (ETD) → impaired middle ear (ME) drainage.
- Viral URI → ME inflammation → pathogen reflux from nasopharynx.
- Bacterial proliferation → suppurative effusion.

⭐ The most common bacterial pathogen causing AOM is Streptococcus pneumoniae.
AOM: Clinical Features & Otoscopy - The Ear Weeps
- Clinical Triad: Otalgia (ear pain), fever, hearing loss. Irritability in infants.
- Otorrhea if Tympanic Membrane (TM) perforates.
- Otoscopy:
- TM: Erythematous, opaque, bulging.
- Loss of light reflex & bony landmarks.
- ↓ Mobility on pneumatic otoscopy.
- Pus/fluid behind TM; purulent discharge if perforated.

⭐ A bulging tympanic membrane on otoscopy is a hallmark sign of AOM.
AOM: Diagnosis & Criteria - Spotting the Sickness
- AOM Diagnostic Criteria:
- Acute onset (symptoms <48 hours).
- Middle Ear Effusion (MEE) evidenced by ≥1 of:
- Bulging tympanic membrane (TM).
- Limited/absent TM mobility.
- Air-fluid level behind TM.
- Otorrhea.
- Signs of acute middle ear inflammation (e.g., distinct TM erythema, otalgia).
- Key Finding:
⭐ Impaired mobility of the tympanic membrane on pneumatic otoscopy is a key diagnostic finding in AOM.
AOM: Complications - When It Gets Nasty
- Intratemporal (Within Temporal Bone):
- Mastoiditis (most common suppurative)
- Petrositis
- Facial nerve palsy
- Labyrinthitis
- Intracranial (Inside Skull):
- Meningitis
- Brain abscess (temporal lobe, cerebellum)
- Lateral sinus thrombophlebitis (LST)
- Otitic hydrocephalus
- Extracranial (Rare):
- Bezold's abscess (spread to sternocleidomastoid)
⭐ Acute mastoiditis is the most frequent suppurative complication of AOM.
- Non-suppurative:
- Hearing loss (conductive, sensorineural)
- Tympanosclerosis
AOM: Management - Kicking the Infection
-
Pain/Fever: Acetaminophen or Ibuprofen.
-
Observation (48-72h): Option for non-severe AOM if:
- Unilateral: 6 months - 2 years.
- Unilateral/Bilateral: ≥2 years.
-
Antibiotic Therapy Algorithm:
⭐ Amoxicillin (80-90 mg/kg/day) is the first-line antibiotic for AOM in most cases.
-
Key Points:
- Duration: 5-7 days (≥2y, mild-mod); 10 days (<2y or severe).
- Recurrent AOM (≥3 episodes/6mo or ≥4 episodes/12mo): Consider tympanostomy tubes.
High‑Yield Points - ⚡ Biggest Takeaways
- Most common bacteria: Streptococcus pneumoniae, then H. influenzae (non-typable), M. catarrhalis.
- Peak age group: Infants and children aged 6 to 24 months.
- Key symptoms: Sudden onset otalgia, fever, irritability, and conductive hearing loss.
- Otoscopic findings: Bulging, erythematous tympanic membrane; impaired mobility and loss of light reflex.
- First-line antibiotic: Amoxicillin is preferred; consider amoxicillin-clavulanate for recurrent/resistant cases.
- Most common intratemporal complication: Acute mastoiditis.
- Most common intracranial complication: Meningitis.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more