Filariasis Basics - Wormy Intruders
- Lymphatic Filariasis (LF): Chronic parasitic disease; affects lymphatics.
- Causative Agents: Nematodes (filarial worms).
- Wuchereria bancrofti (~90% cases).
- Brugia malayi.
- Brugia timori.
- Vectors: Mosquitoes.
- Culex quinquefasciatus (urban W. bancrofti).
- Anopheles spp. (rural W. bancrofti).
- Mansonia spp. (Brugia).
- Transmission: Infective L3 larvae from mosquito bite. Microfilariae (mf) in blood.
- Endemic in India.
⭐ Wuchereria bancrofti exhibits nocturnal periodicity (mf peak in peripheral blood at night, 10 PM - 2 AM).
Vectors & Lifecycle - Mosquito Mailmen
- Vectors (Mosquitoes):
- W. bancrofti: Culex (urban), Anopheles (rural), Aedes.
- B. malayi: Mansonia, Anopheles.
- B. timori: Anopheles barbirostris.
- Lifecycle:
- Mosquito (intermediate host) deposits L3 larvae on skin.
- L3 larvae enter skin, migrate to lymphatics.
- Mature into adult worms (human: definitive host).
- Adults release microfilariae (L1) into blood.
- Mosquito ingests L1; develop to L3 in mosquito.
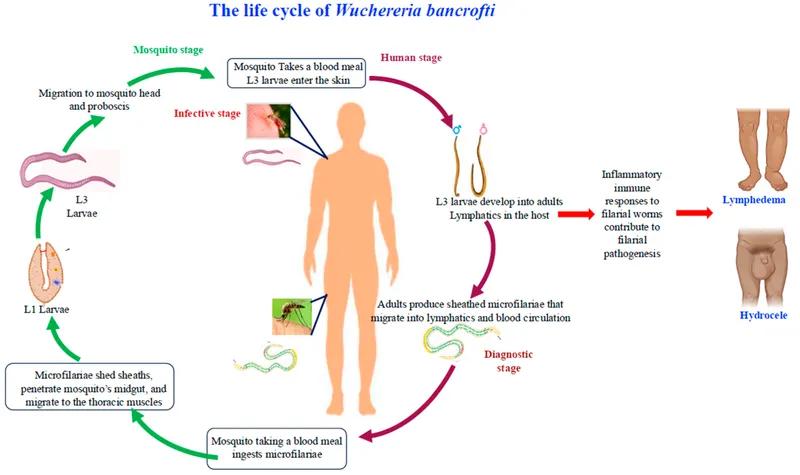
⭐ W. bancrofti microfilariae show nocturnal periodicity (peak 10 PM - 2 AM). (📌 Mnemonic: "Bankers work late")
Clinical Picture - Elephant Tales & More
- Asymptomatic Microfilaremia: Common; asymptomatic despite blood microfilariae.
- Acute Lymphatic Filariasis:
- Adenolymphangitis (ADL) / Filarial Fever: Recurrent fever, chills, painful lymphadenopathy & retrograde lymphangitis.
- Acute epididymo-orchitis, funiculitis (esp. males).
- Chronic Lymphatic Disease (Develops over years):
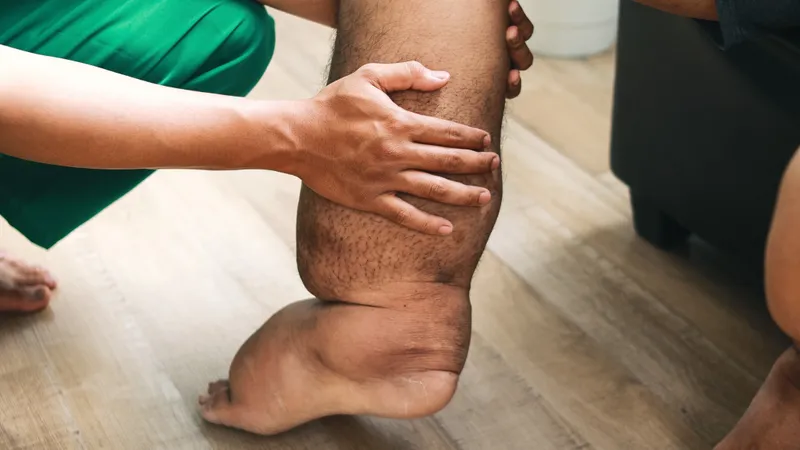
- Lymphedema: Progressive: pitting → brawny, non-pitting edema.
- Hydrocele: Most common in Bancroftian filariasis; scrotal swelling.
- Elephantiasis: Irreversible enlargement (limbs, scrotum, penis, vulva, breasts). Skin hyperkeratotic, coarse, fissured.
- Chyluria: Milky urine (lymphatic fluid, chyle).
- Occult Filariasis (e.g., Tropical Pulmonary Eosinophilia - TPE):
- Blood microfilariae absent (sequestered in lungs/tissues).
- Nocturnal cough, wheeze, dyspnea, marked eosinophilia, ↑IgE.
⭐ Hydrocele is the most common chronic manifestation of Bancroftian filariasis.
Diagnosis Decoded - Finding Filaments
- Microfilariae (MF) Detection: Key for diagnosis.
- Peripheral Blood Smear (PBS): Gold standard.
- Timing: Nocturnal sample (10 PM - 2 AM) for W. bancrofti, B. malayi.
- Stain: Giemsa. Thick/thin smears examined.
- Concentration Methods: ↑ sensitivity (e.g., Knott's, membrane filtration).
- QBC (Quantitative Buffy Coat): For MF detection using fluorescence microscopy.
- DEC Provocation Test: Induces daytime appearance of MF after 2 mg/kg DEC dose.
- Peripheral Blood Smear (PBS): Gold standard.
- Adult Worm Detection:
- Ultrasound (USG): "Filarial dance sign" (visualization of live, motile adult worms in lymphatics).
- Biopsy: Lymph node or nodule biopsy may show adult worms.
- Antigen Detection (W. bancrofti):
- Immunochromatographic Card Test (ICT): Detects Circulating Filarial Antigen (CFA).
⭐ CFA tests (e.g., ICT) can be positive even in amicrofilaremic (occult) filariasis and chronic infections.
Management & Defense - Worm Warfare
- Drug of Choice (DOC): Diethylcarbamazine (DEC).
- Regimen: 6 mg/kg/day orally for 12 days.
- Action: Potent microfilaricidal; also damages adult worms.
- ⚠️ Caution: Mazzotti reaction (systemic/local inflammation from dying mf); manage with antihistamines/corticosteroids.
- Lymphedema Care: Meticulous hygiene, limb elevation, exercises, compression; Complex Decongestive Therapy (CDT).
- Hydrocele: Surgical management (hydrocelectomy).
- Mass Drug Administration (MDA): Annual single dose of DEC (6 mg/kg) with Albendazole; or Ivermectin + Albendazole.
- Vector Control: Integrated strategies against mosquito vectors (IRS, larviciding, LLINs).
⭐ DEC is the only drug effective against adult filarial worms (macrofilaricidal), particularly W. bancrofti.
High‑Yield Points - ⚡ Biggest Takeaways
- Causative agents: Wuchereria bancrofti, Brugia spp.; Vector: Mosquitoes.
- Hallmark: Chronic lymphedema leading to elephantiasis and hydrocele.
- Acute episodes: Recurrent adenolymphangitis (ADL) with fever and painful lymphadenopathy.
- Diagnosis: Nocturnal blood smear for microfilariae; ICT card test for W. bancrofti antigen.
- Treatment: Diethylcarbamazine (DEC) is mainstay; doxycycline for Wolbachia.
- Tropical Pulmonary Eosinophilia (TPE): Occult filariasis with nocturnal cough, marked eosinophilia.
- Control: Mass Drug Administration (MDA); vector control.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

