Melanoma - Basics & Bad Seeds
- Malignant tumor of melanocytes; commonest skin cancer causing death.
- Etiology: UV radiation (UVB > UVA) is the primary modifiable risk factor, causing DNA damage.

- Risk Factors:
- Sun exposure (intense, intermittent > chronic).
- Fair skin, >50 common nevi, atypical nevi.
- Family history (e.g., FAMMM syndrome, CDKN2A gene).
- Immunosuppression.
- Indian Context: Acral lentiginous melanoma (palms, soles, subungual) is more prevalent.
⭐ Intermittent, intense sun exposure is a higher risk factor for melanoma development than chronic, cumulative exposure.
Melanoma - Rogue Cells & Faces
- Pathogenesis: Key mutations: BRAF, NRAS, c-KIT. Growth phases: Radial (intraepidermal) then Vertical (invasive, ↑metastatic potential).
- Precursor Lesions: Giant congenital nevi (>20cm), dysplastic nevi.
- Major Clinicopathological Types: 📌 Superficial Nodules Linger Around Amelanotic spots.
- Superficial Spreading (SSM): Most common overall.
- Nodular (NM): Worst prognosis, rapid vertical growth.
- Lentigo Maligna Melanoma (LMM): Elderly, sun-exposed areas.
- Acral Lentiginous Melanoma (ALM): Palms, soles, subungual; common in darker skin.
- Amelanotic Melanoma: Difficult diagnosis, lacks pigment.

⭐ Nodular melanoma has no significant radial growth phase, presenting early with vertical growth.
Melanoma - Spotting the Enemy
- Clinical Clues: New/changing mole; symptoms like itching, bleeding.
- ABCDE Rule (📌):
- Asymmetry
- Border irregularity
- Color variegation (multiple shades)
- Diameter >6mm
- Evolving/Elevation (change in size, shape, color, elevation)
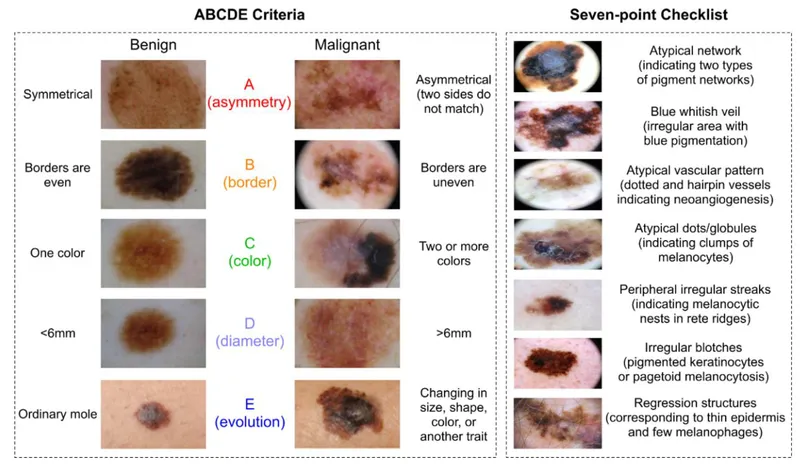
- Glasgow 7-Point Checklist:
- Major (3): Change in size, shape, color.
- Minor (4): Diameter >6mm, inflammation, oozing/bleeding, altered sensation.
- Diagnosis:
- Dermoscopy for initial evaluation.
- Excisional biopsy (gold standard) with 1-3mm margins for suspicious lesions. Avoid shave/punch biopsy.
⭐ Excisional biopsy is the diagnostic procedure of choice for a suspected melanoma.
Melanoma - Sizing Up Trouble
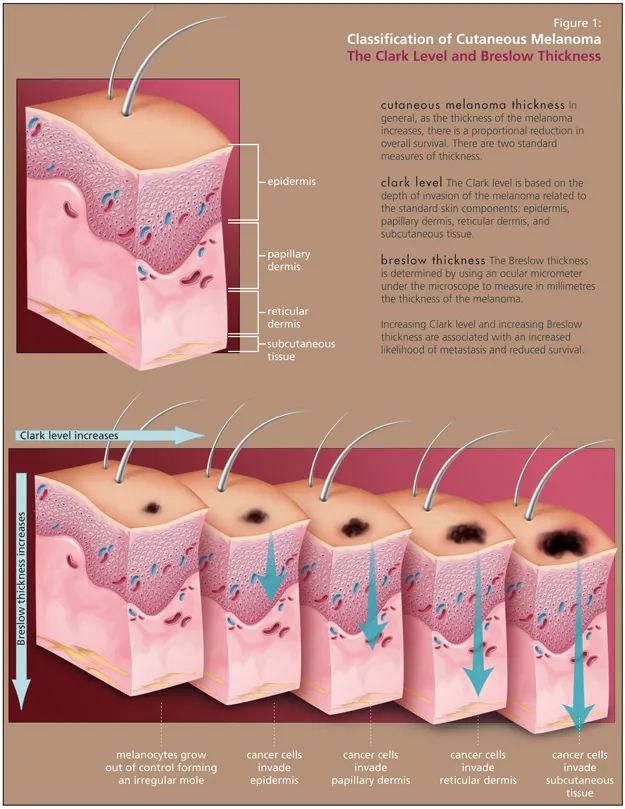
- Microstaging: Key for prognosis.
- Breslow Thickness: Depth in mm; most crucial prognostic factor.
- Clark Level: Anatomical invasion level; less used now.
- TNM Staging (AJCC 8th Ed.): Guides treatment.
- T: Tumor thickness (Breslow), ulceration.
- N: Nodal involvement (number, burden).
- M: Distant metastasis.
- Key Prognostic Factors:
- Breslow depth, ulceration, mitotic rate.
- Lymph node status, distant metastasis, LDH levels.
- Sentinel Lymph Node Biopsy (SLNB):
- Indications: Breslow >1mm, OR Breslow >0.8mm if ulceration/high mitotic rate present.
⭐ Breslow thickness is the single most important prognostic factor in localized melanoma.
Melanoma - Battle Plan Alpha
Multidisciplinary team essential.
- Surgical Management: Wide Local Excision (WLE) primary. Margins by Breslow depth:
- In situ: 0.5-1cm
- <1mm: 1cm
- 1-2mm: 1-2cm
-
2mm: 2cm
- Adjuvant Therapy (High-risk: Stage IIB/C, III):
- Immunotherapy (Nivolumab, Pembrolizumab)
- Targeted (BRAF V600): Dabrafenib/Trametinib
- Metastatic (Stage IV): Systemic therapy (Immunotherapy, Targeted). Chemo limited.
- Radiotherapy: Palliative; adjuvant in select cases.
⭐ For BRAF V600-mutated metastatic melanoma, combination BRAF/MEK inhibitors show improved outcomes over BRAF inhibitor monotherapy.
High-Yield Points - ⚡ Biggest Takeaways
- Breslow thickness: Single most important prognostic factor.
- ABCDE criteria: For clinical diagnosis (Asymmetry, Border, Color, Diameter >6mm, Evolving).
- Superficial Spreading Melanoma: Most common subtype.
- Acral Lentiginous Melanoma: Common in dark skin (palms, soles, nail beds).
- Nodular Melanoma: Worst prognosis due to rapid vertical growth.
- BRAF V600E mutation: Key therapeutic target.
- Sentinel Lymph Node Biopsy (SLNB): For tumors >1mm or ulcerated_
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

