Cutaneous Lymphomas: Overview - Skin's Stealthy Cells
- Heterogeneous group of extranodal non-Hodgkin lymphomas (NHL) primarily affecting the skin.
- Clonal proliferations of T-cells, B-cells, or rarely NK-cells.
- Incidence: ~1 per 100,000; more common in older adults (median age 50-60 years).
- Cutaneous T-cell lymphomas (CTCLs) are more common (~75%) than cutaneous B-cell lymphomas (CBCLs, ~25%).
⭐ Mycosis fungoides is the most common type of CTCL, often presenting with patches, plaques, and tumors.
Mycosis Fungoides: Patchy Problems - Fungus Mimic Rash
- Most common Cutaneous T-cell Lymphoma (CTCL); chronic, indolent. Often misdiagnosed as eczema/psoriasis ("fungus mimic").
- Clinical Progression:
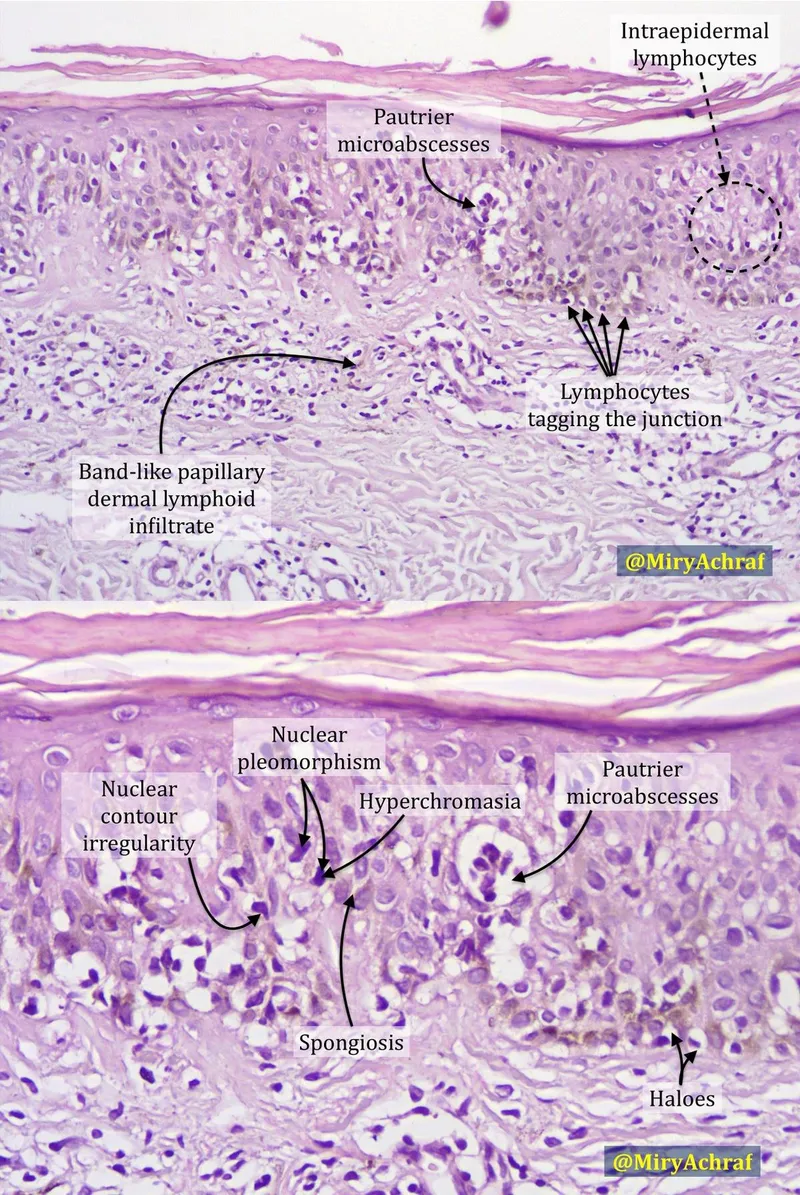
- Key Histo: Atypical T-lymphocytes (cerebriform/Lutzner cells) forming Pautrier's microabscesses in epidermis.
⭐ Pautrier's microabscesses are highly characteristic, not strictly pathognomonic, but a key diagnostic feature.
- Sézary Syndrome: Advanced, erythrodermic MF variant with >1000/µL circulating Sézary cells (Lutzner cells in blood) & lymphadenopathy.
- 📌 Mnemonic: My Fungoides = Many Faces (mimics various rashes).
Sézary Syndrome: Red Man's Woe - Itchy Crimson Tide
- Aggressive leukemic variant of Cutaneous T-cell Lymphoma (CTCL).
- Classic triad:
- Widespread erythroderma (>80% Body Surface Area).
- Generalized lymphadenopathy.
- Circulating atypical T-cells (Sézary cells >1000/μL).
- Sézary cells: Lymphocytes with characteristic cerebriform nuclei.
- Other criteria: CD4/CD8 ratio >10; clonal T-cell receptor (TCR) gene rearrangement.
- Intense pruritus, alopecia, palmoplantar keratoderma common.
⭐ Absolute Sézary cell count >1000/μL in peripheral blood is a major diagnostic criterion for Sézary Syndrome (WHO-EORTC).
Other CTCLs: Beyond MF/SS - T-Cell's Wild Cards
- Lymphomatoid Papulosis (LyP): Chronic, recurrent, self-healing CD30+ papulonodules. Low systemic lymphoma risk (10-20%).
- Primary Cutaneous Anaplastic Large Cell Lymphoma (pcALCL): Solitary/grouped CD30+ nodules/tumors. Generally good prognosis.
- Subcutaneous Panniculitis-like T-cell Lymphoma (SPTCL): Deep nodules/plaques (panniculitis). α/β T-cell phenotype. Often associated with hemophagocytic syndrome.
- Primary Cutaneous Gamma/Delta T-cell Lymphoma (PCGD-TCL): Aggressive. Ulceronecrotic plaques/tumors. Poor prognosis.

⭐ pcALCL typically presents with solitary or localized tumors and strong CD30 expression, carrying a favorable prognosis when confined to the skin (5-year survival >90%).
Cutaneous B-Cell Lymphomas: B-Cell Brigade - B-Team Defenders
- Rarer than CTCLs; generally better prognosis. Usually CD20+.
- Key Types:
- PCMZL (Primary Cutaneous Marginal Zone): Indolent. Solitary/multiple nodules (trunk, arms). BCL2+, BCL6-.
- PCFCL (Primary Cutaneous Follicle Center): Indolent. Papules/nodules (scalp, forehead, trunk). BCL6+, BCL2-.
⭐ PCFCL being BCL2-negative is a key distinction from systemic follicular lymphoma.
- PCDLBCL, Leg Type (Primary Cutaneous Diffuse Large B-Cell Lymphoma, Leg Type): Aggressive. Tumors on one/both legs; elderly women. BCL2+, BCL6+, MUM1+.
- Dx: Skin biopsy (histology, IHC). Rx: Local (radiotherapy, surgery), systemic (rituximab, chemo).

Diagnosis & Management: Unmask & Treat - Spot, Stage, Solve!
- Spot (Diagnosis): Persistent, pruritic lesions. Crucial: Skin biopsy (histopathology, IHC, TCR gene rearrangement).
- Stage (Staging): TNM classification. Blood for Sézary cells (MF/SS). Imaging (CT/PET) for advanced disease.
- Solve (Management): Multidisciplinary. Skin-directed (topicals, phototherapy, RT) for early; Systemic (retinoids, IFN, chemo, targeted) for advanced.
⭐ Pautrier's microabscesses (intraepidermal collections of atypical lymphocytes) are characteristic of Mycosis Fungoides.
High‑Yield Points - ⚡ Biggest Takeaways
- Mycosis Fungoides (MF): Most common CTCL, progresses patch → plaque → tumor. Pautrier's microabscesses are key.
- Sézary Syndrome: Leukemic CTCL; erythroderma, lymphadenopathy, circulating Sézary cells (cerebriform nuclei).
- Both MF & Sézary Syndrome are typically CD4+ T-cell lymphomas.
- Lymphomatoid Papulosis (LyP): CD30+, recurrent, self-healing papules; low malignant risk.
- Primary Cutaneous B-Cell Lymphomas (PCBCLs): Generally better prognosis than systemic counterparts.
- Treatment: Topical therapies (steroids, PUVA) for early stages; systemic for advanced disease.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

