Genetic Predisposition & Triggers - Genes & Jolts
- Genetic Factors ("Genes"):
- Polygenic; PSORS1 on chromosome 6p21 is the major susceptibility locus, accounting for up to 50% of heritability.
- HLA-Cw6: Strongest genetic marker, especially for early-onset (Type I) & guttate psoriasis.
⭐ HLA-Cw6 is the most strongly associated genetic marker for early-onset psoriasis.
- Environmental Triggers ("Jolts"):
- Trauma: Koebner phenomenon (isomorphic response; new lesions at sites of skin injury).
- Infections: Group A Streptococcal pharyngitis (classically triggers guttate psoriasis).
- Stress: Psychological or physiological; can exacerbate or initiate.
- Medications: 📌 BLAN (Beta-blockers, Lithium, Antimalarials, NSAIDs).
Innate Immune Activation - Early Warning Mayhem
Triggers (e.g., Koebner phenomenon, infections) initiate keratinocyte stress, the first step in psoriatic lesion development.
- Stressed Keratinocytes: Act as primary sensors. They release danger signals:
- Antimicrobial peptides (AMPs), notably LL-37.
- Self-DNA and self-RNA fragments.
- Plasmacytoid Dendritic Cell (pDC) Activation:
- LL-37 complexes with self-DNA/RNA, forming autoantigens.
- These complexes activate pDCs via endosomal Toll-like Receptors: TLR7 (recognizing RNA) and TLR9 (recognizing DNA).
- Activated pDCs robustly produce IFN-α (a key Type I Interferon), amplifying the early immune response.
- Myeloid Dendritic Cell (mDC) Activation:
- Stimulated by keratinocyte-derived danger signals and IFN-α from pDCs.
- mDCs unleash a cascade of pro-inflammatory cytokines:
- TNF-α, IL-1β, IL-6 (driving general inflammation).
- IL-23 (critical for the subsequent Th17 cell differentiation and psoriatic plaque maintenance).
⭐ LL-37 complexed with self-DNA/RNA acts as a key autoantigen, activating plasmacytoid dendritic cells via TLRs, initiating the psoriatic cascade.
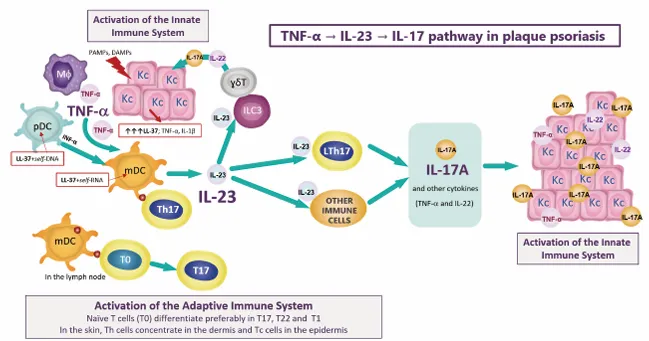
Adaptive Immune Response - T-Cell Takeover
- Antigen Presentation & T-Cell Priming:
- Activated mDCs migrate to lymph nodes, presenting antigens to naive T-cells.
- This initiates T-cell priming and differentiation into effector subsets.
- Key Differentiated T-Cell Subsets & Cytokines:
- Th1 cells: Produce IFN-γ, TNF-α (pro-inflammatory).
- Th17 cells: Major pathogenic role. Produce IL-17A, IL-17F, IL-22.
- The IL-23/Th17 axis is crucial for Th17 activity (📌 IL-23 "fuels" Th17).
- Th22 cells: Produce IL-22 (keratinocyte effects).
- Cytokine Effects on Skin:
- IL-17 (A/F): ↑ Keratinocyte proliferation, ↑ pro-inflammatory mediators (chemokines, AMPs).
- TNF-α: Amplifies inflammation.
- IL-22: ↑ Keratinocyte hyperproliferation, epidermal thickening, ↓ differentiation.
⭐ > The IL-23/Th17 axis is a central pathogenic pathway in psoriasis and a key target for biologic therapies.
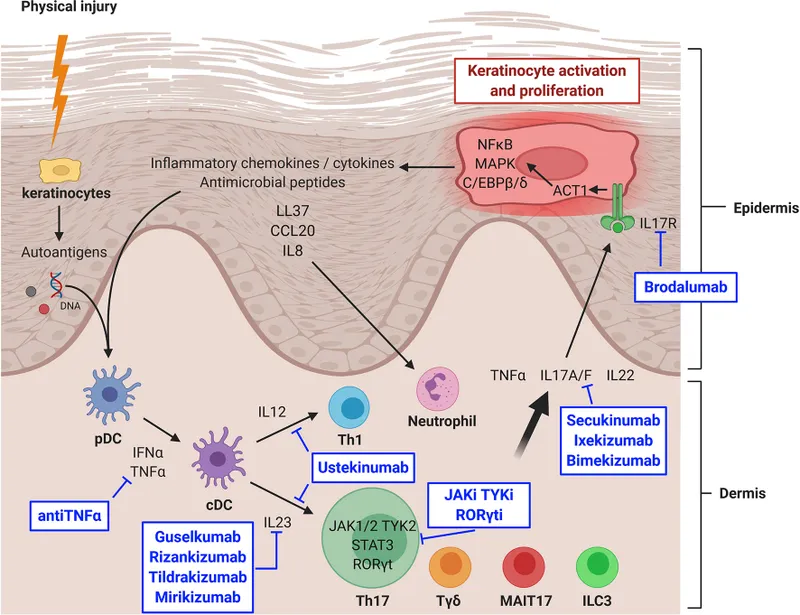
Keratinocyte & Vascular Changes - Skin's Wild Growth
- Keratinocyte Hyperproliferation:
- Accelerated epidermal turnover (cells divide ~7x faster).
- Acanthosis: Marked epidermal thickening.
- Parakeratosis: Nuclei retained in stratum corneum.
- Abnormal differentiation: Reduced or absent granular layer.
- Neutrophil Infiltration: (📌 Munro = Stratum Corneum; Kogoj = Stratum Spinosum)
- Munro's microabscesses: Neutrophils in stratum corneum.
- Kogoj's spongiform pustules: Neutrophils within stratum spinosum.
- Vascular Changes:
- Angiogenesis: ↑ new, leaky blood vessels.
- Dilated, tortuous capillaries in dermal papillae (pinpoint bleeding on scale removal - Auspitz sign).
- Driven by pro-angiogenic factors (e.g., VEGF).
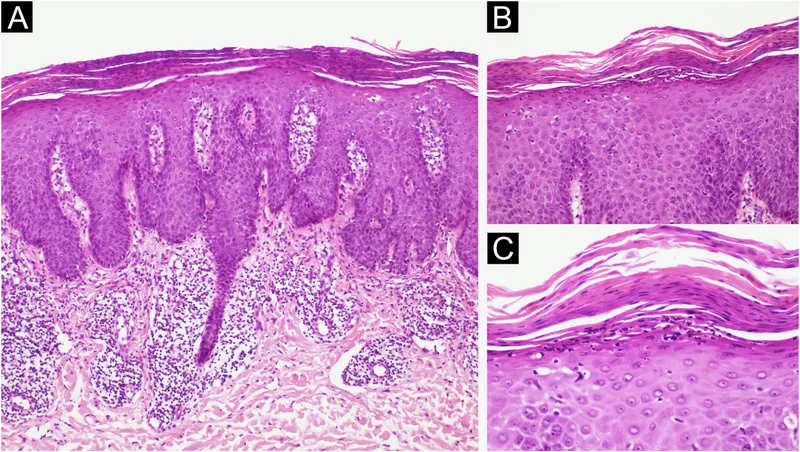
⭐ Munro's microabscesses, collections of neutrophils in the stratum corneum, are a characteristic histological feature of psoriasis.
High‑Yield Points - ⚡ Biggest Takeaways
- Psoriasis: A chronic inflammatory skin disease with strong genetic predisposition (e.g., HLA-Cw6).
- Immune-mediated pathogenesis: Primarily driven by activated T-cells (Th1, Th17, Th22) and their cytokines.
- Key pro-inflammatory cytokines include TNF-α, IL-17, IL-22, and IL-23.
- Results in keratinocyte hyperproliferation and abnormal differentiation, forming characteristic plaques.
- Histological hallmarks: Acanthosis, parakeratosis, and Munro's microabscesses (neutrophils in stratum corneum).
- Clinically important: Auspitz sign (pinpoint bleeding) and Koebner phenomenon (trauma-induced lesions).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

