Neonatal Skin Physiology & Approach - Tiny Skin Big Changes
- Thinner epidermis & dermis; fewer cell layers.
- ↑ Surface area to volume ratio: ↑ drug absorption, ↑ heat/water loss.
- Immature barrier function: improves over first few weeks.
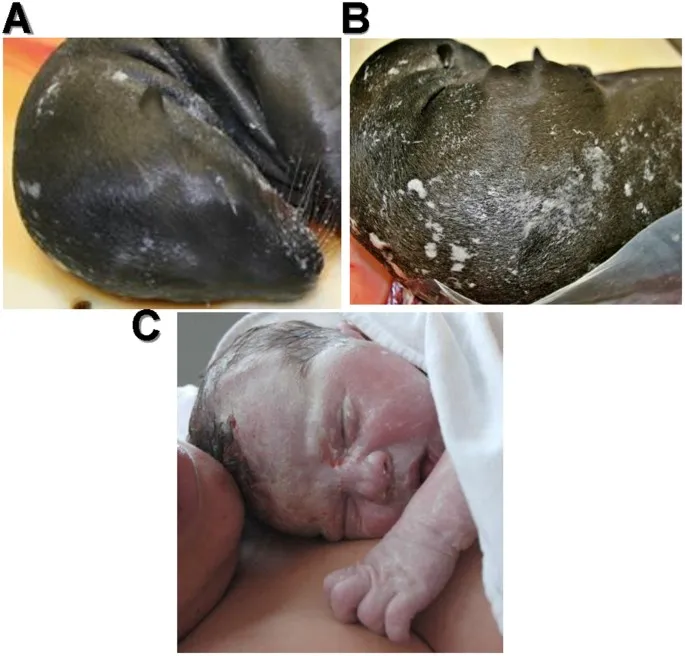
- Vernix caseosa: cheesy, white biofilm. Composed of sebum, lanugo, epidermal cells.
⭐ Vernix caseosa protects against amniotic fluid maceration and provides innate immunity.
- Skin pH: ~6.0 at birth, acidifies to 4.5-5.5 (acid mantle).
- Eccrine glands functional; apocrine glands develop at puberty.
- Melanocytes present, less active initially.
Transient Benign Lesions - Passing Skin Shows
- 📌 Miliaria: Crystalline Clear, Rubra Red & Rough.
| Lesion | Key Features | Onset | Resolution | Histology (Key) |
|---|---|---|---|---|
| Erythema Toxicum Neonatorum (ETN) | Flea-bitten rash; spares palms/soles | 24-48 hrs | 7-14 days | Eosinophils |
| Transient Neonatal Pustular Melanosis (TNPM) | Pustules → scale → pigmented macules; all areas | Birth | Pustules: days; Macules: wks-mths | Neutrophils (no eos) |
| Milia | 1-2 mm white keratin cysts; face | Birth | Weeks | Keratin cysts |
| Miliaria Crystallina | Tiny clear vesicles; non-inflammatory | First few wks | Days | Block: Stratum corneum |
| Miliaria Rubra (Prickly Heat) | Red papules/pustules; pruritic; intertriginous | First few wks | Days-wks | Block: Deeper epidermis |
| Sebaceous Gland Hyperplasia | Tiny yellow papules; nose, cheeks (maternal androgens) | Birth | Wks-mths | Hyperplastic seb. glands |
| Mongolian Spots | Blue-grey macules; lumbosacral (Asian/African) | Birth | 3-5 yrs | Dermal melanocytes |
Vesiculopustular Eruptions - Bumps & Bubbles Alert
- Common Benign Conditions (Usually well baby):
- Erythema Toxicum Neonatorum (ETN): Appears day 2-5. Erythematous macules, papules, pustules ("flea-bitten"). Wright stain: Eosinophils. Resolves spontaneously.
- Transient Neonatal Pustular Melanosis (TNPM): Present at birth. Fragile pustules rupture → collarette of scale & hyperpigmented macules. Wright stain: Neutrophils. Benign.
- Miliaria (Crystallina, Rubra, Pustulosa): Due to sweat duct obstruction (heat/humidity). Superficial vesicles or erythematous papules/pustules.
- Infectious (Potentially Serious - Prompt Diagnosis & Rx Crucial):
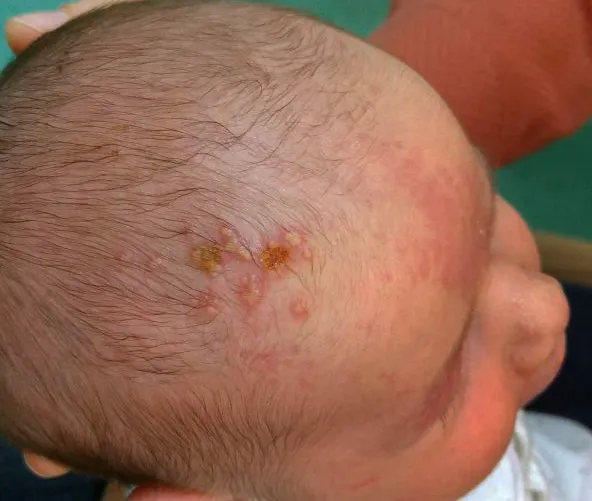
- Neonatal Herpes Simplex (HSV): Grouped vesicles on erythematous base. May be localized or disseminated. Tzanck smear: Multinucleated giant cells. Rx: Acyclovir 20 mg/kg IV q8h.
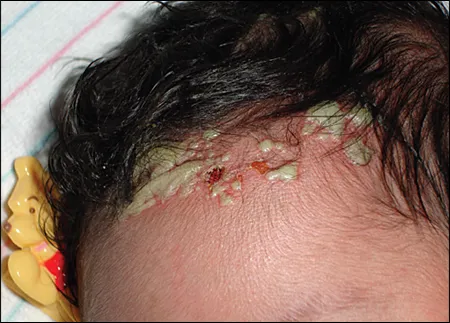
- Staphylococcal Pustulosis/Impetigo: Pustules, bullae (Bullous Impetigo if S. aureus produces exfoliative toxin), honey-colored crusts. Gram stain: Gram+ cocci in clusters. Culture. Rx: Antibiotics.
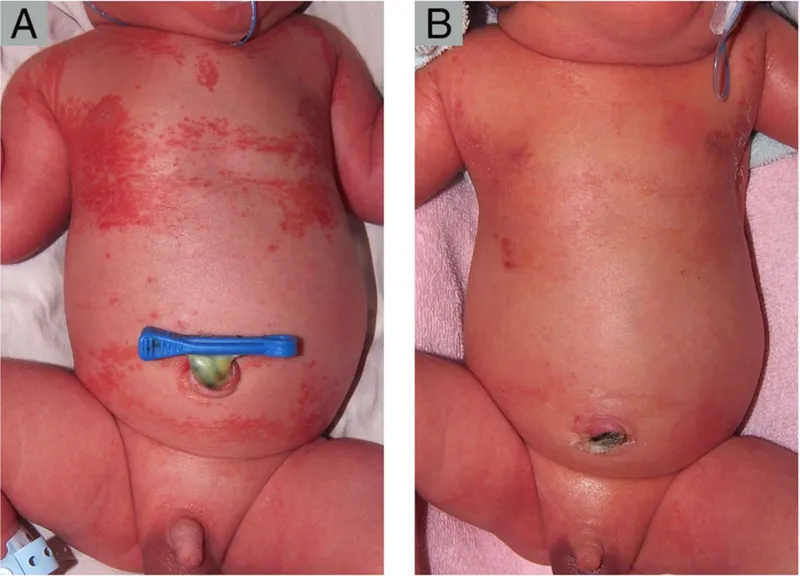
- Neonatal Candidiasis: Erythematous plaques with satellite papules/pustules. Common in intertriginous areas, diaper area. KOH prep: Pseudohyphae, spores. Rx: Topical/Systemic antifungals.
- Neonatal Herpes Simplex (HSV): Grouped vesicles on erythematous base. May be localized or disseminated. Tzanck smear: Multinucleated giant cells. Rx: Acyclovir 20 mg/kg IV q8h.
- Other: Infantile Acropustulosis (recurrent, intensely pruritic vesicopustules on acral sites).
⭐ Multinucleated giant cells on Tzanck smear are characteristic of Herpes simplex infection.
Birthmarks & Nevi - Marks of Distinction
Common congenital markings; early recognition is key.
| Birthmark | Key Features | Associations | Management Flags |
|---|---|---|---|
| Nevus Simplex (Salmon Patch) | Pink macules (eyelids, glabella, nape); fade ~1-2yr | - | Reassurance |
| Port-Wine Stain (PWS) | Dark red/purple patches; persist, may thicken | Sturge-Weber (V1/V2), Klippel-Trenaunay | Ophtho/Neuro consult if V1/V2; Laser |
| Infantile Hemangioma | Bright red (superficial), bluish (deep); grow then involute | PHACES (📌) (large facial) | Propranolol (2-3 mg/kg/day); Ulceration, obstruction |
| Congenital Melanocytic Nevus (CMN) | Brown/black; present at birth; melanoma risk ↑ with size | Neurocutaneous melanosis (large/multiple) | Monitor; Excision for giant CMN (>20cm) |
| Nevus Sebaceus | Yellowish, waxy plaque (scalp/face); ↑ BCC risk later | Schimmelpenning syndrome | Monitor; Excision controversial |
 |
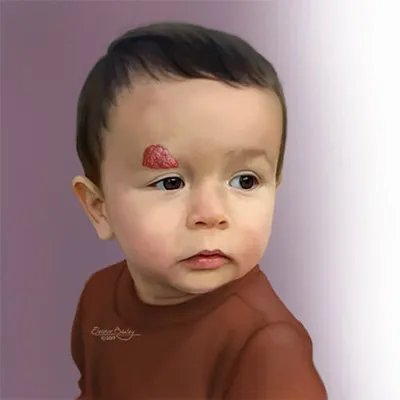
⭐
Facial port-wine stain in V1 dermatomal distribution is highly associated with Sturge-Weber syndrome, warranting ophthalmology and neurology evaluation.
📌 PHACES syndrome components:
- Posterior fossa malformations
- Hemangiomas (large facial)
- Arterial anomalies
- Cardiac defects
- Eye abnormalities
- Sternal cleft/Supraumbilical raphe
High‑Yield Points - ⚡ Biggest Takeaways
- Erythema toxicum neonatorum: Benign rash, eosinophils on smear; spares palms/soles.
- Transient Neonatal Pustular Melanosis (TNPM): Pustules to collarettes of scale, hyperpigmentation; neutrophils on smear.
- Milia: Common, tiny white keratin-filled cysts; resolve spontaneously.
- Miliaria rubra: "Prickly heat" due to blocked sweat ducts; erythematous papules.
- Seborrheic dermatitis: "Cradle cap"; greasy, yellow scales on scalp/face.
- Neonatal acne: Maternal/endogenous androgen-driven; comedones, papules, pustules.
- Harlequin color change: Transient, benign unilateral erythema with midline demarcation.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

