Occupational Pigmentary Disorders - Hue Done It?
- Skin dyschromia (color changes) from workplace exposures.
- Types:
- Hyperpigmentation: ↑ melanin (e.g., tar, pitch, psoralens, arsenic).
- Hypopigmentation: ↓ melanin (e.g., phenols, hydroquinone, mercaptans).
- Depigmentation/Leukoderma: Complete melanin loss (e.g., MBEH).
- Causative Agents:
- Chemicals: Phenols, catechols, quinones, heavy metals (As, Ag, Au, Hg), tars.
- Physical: Heat, UV radiation, chronic friction/trauma.
- Biological: Rare, post-inflammatory changes.
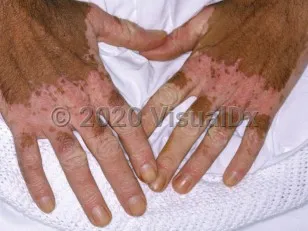
⭐ Monobenzyl ether of hydroquinone (MBEH) in rubber products classically causes irreversible occupational contact leukoderma, often mimicking vitiligo.
Occupational Hyperpigmentation - Shady Business
- Etiology: Prolonged/repeated exposure to specific agents in the workplace.
- Key Causative Agents & Presentations:
- Tar & Pitch (Coal Tar Derivatives): Melanosis, often reticulate pattern on sun-exposed areas (face, neck, forearms, V of chest). Photosensitization common. Riehl's melanosis-like picture.
- Specific compounds: Phenols, cresols, anthracene.
- Petroleum Oils & Greases: Follicular hyperpigmentation (oil acne), comedones, perifollicular melanosis on forearms, thighs.
- Drugs: Certain medications handled occupationally (e.g., phenothiazines) can cause slate-grey pigmentation.
- Phytophotodermatitis (Berloque Dermatitis): Contact with psoralen-containing plants (e.g., celery, parsnips, figs, limes) + UVA exposure → patterned hyperpigmentation (streaks, bizarre shapes).
- Mechanism: Furocoumarins (psoralens) are photosensitizers.
- Metals: Arsenic (diffuse or raindrop pigmentation), silver (argyria - slate-grey/blue-grey).
- Friction/Pressure: Lichenification and post-inflammatory hyperpigmentation (PIH) at sites of chronic rubbing.
- Tar & Pitch (Coal Tar Derivatives): Melanosis, often reticulate pattern on sun-exposed areas (face, neck, forearms, V of chest). Photosensitization common. Riehl's melanosis-like picture.
⭐ Exam Favourite: Phytophotodermatitis often presents with streaky or bizarre hyperpigmented macules corresponding to areas of contact with plant-derived photosensitizers followed by sun exposure.
- Diagnosis: Detailed occupational history, distribution of lesions, patch testing (sometimes), biopsy (rarely needed).
- Management: Avoidance of causative agent, sun protection, topical depigmenting agents (hydroquinone, retinoids, azelaic acid).
Occupational Hypo/Depigmentation - Vanishing Hues
Loss of skin pigment from workplace chemical or physical agents, primarily chemical leukoderma.
- Key Causative Agents (Chemical Leukoderma):
- Phenolic & Catecholic Compounds:
- Hydroquinone, monobenzyl ether of hydroquinone (MBEH), p-tertiary butylphenol (PTBP), p-tertiary amylphenol (PTAP), alkylphenols.
- Found in: Germicides, disinfectants, antioxidants (rubber, plastics), photographic developers, adhesives.
- Other Agents: Mercaptans (e.g., mercaptoethylamine), sulfhydryls, arsenic, cinnamic aldehyde.
- Phenolic & Catecholic Compounds:
- Mechanisms of Depigmentation:
- Inhibition of tyrosinase (melanin synthesis enzyme).
- Direct melanocytotoxicity (e.g., via reactive oxygen species).
- Interference with melanosome formation or transfer.
- Occupational Vitiligo:
- Clinically mimics idiopathic vitiligo; may be preceded by contact dermatitis.
- Often starts at sites of direct contact, can spread (Koebnerization).
- Lesions: Well-demarcated, "confetti-like" macules or larger patches.
⭐ MBEH (Monobenzyl Ether of Hydroquinone) can cause permanent, widespread depigmentation resembling vitiligo universalis, even distant from application sites.
OPD Dx & Prevention - Spotting & Stopping
- Dx (Spotting):
- History: detailed occupational exposure, onset, progression.
- Exam: lesion morphology, distribution (exposed sites common).
- Wood's Lamp: assess pigment depth/changes (e.g., vitiligo).
- Patch Test: if allergic contact dermatitis suspected (post-inflammatory changes).
- Biopsy: for diagnostic uncertainty or to exclude other causes.
- Prevention (Stopping):
- Substitution: replace hazardous agents with safer alternatives.
- Engineering Controls: ventilation, closed systems, process modification.
- PPE: appropriate gloves, protective clothing, respirators.
- Education: worker training on hazards, hygiene, early symptom reporting.
- Surveillance: pre-placement & periodic health checks.
⭐ Many occupational pigmentary disorders are secondary to inflammation (post-inflammatory hyper/hypopigmentation).
High‑Yield Points - ⚡ Biggest Takeaways
- Occupational pigmentary disorders include hyperpigmentation (e.g., tar melanosis) or hypopigmentation/leukoderma.
- Hydroquinone causes contact leukoderma and exogenous ochronosis (paradoxical hyperpigmentation) with long-term use.
- Phenols and catechols (e.g., rubber, adhesives) cause occupational leukoderma.
- Chronic arsenicism causes characteristic "raindrop" pigmentation (mixed hypo/hyperpigmentation).
- Tar, pitch, and creosote cause phototoxic reactions and reticulate hyperpigmentation (tar melanosis).
- Phytophotodermatitis (psoralens + UV light) causes post-inflammatory hyperpigmentation.
- Management: Identify and avoid causative agent, plus strict photoprotection.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

