Introduction & Etiology - Fungal Foes
- Dermatophytoses: Superficial fungal infections of keratinized tissues (skin, hair, nails).
- Etiologic agents: Dermatophytes (keratinophilic fungi).
- Key Genera (📌 TME):
- Trichophyton: Affects skin, hair, nails.
- Microsporum: Affects skin, hair.
- Epidermophyton: Affects skin, nails.
- Ecological Classification:
- Anthropophilic: Human-to-human (e.g., T. rubrum).
- Zoophilic: Animal-to-human (e.g., M. canis).
- Geophilic: Soil-to-human (e.g., M. gypseum).
- Pathogenesis: Keratinase enzymes digest keratin, facilitating invasion.

⭐ Trichophyton rubrum is the most common dermatophyte globally, frequently causing chronic infections like tinea pedis and tinea cruris.
Clinical Manifestations - Ringworm Roundup
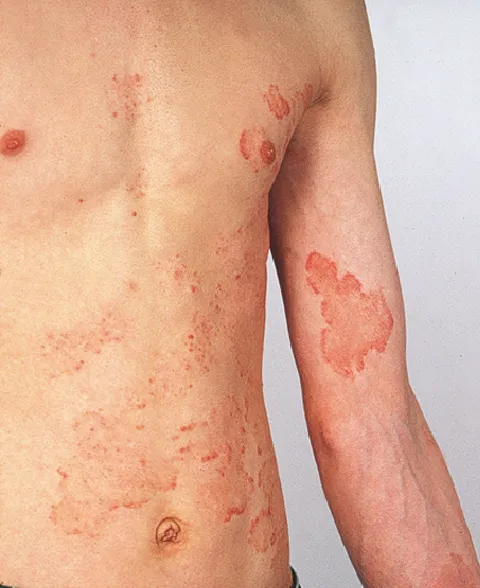
- General: Annular, erythematous, scaling plaques; active, raised border; central clearing. Pruritus common.
- Tinea Corporis (Body): Classic ringworm on trunk, limbs.
- Tinea Cruris (Groin): "Jock itch". Erythematous patches on inner thighs, inguinal folds; scrotum spared.
- Tinea Pedis (Feet): "Athlete's foot".
- Types: Interdigital (most common, maceration), Moccasin (diffuse scaling), Vesiculobullous (vesicles/bullae).
- Tinea Manuum (Hands): Often unilateral scaling; "Two feet, one hand" syndrome.
- Tinea Capitis (Scalp): Alopecia, scaling, broken hairs.
- Patterns: Ectothrix, Endothrix.
- Inflammatory: Kerion (boggy mass).
- Chronic: Favus (scutula; yellowish, cup-shaped crusts).
⭐ Wood's lamp: Microsporum spp. fluoresce blue-green; Trichophyton spp. usually do not.
- Tinea Barbae (Beard): Pustular folliculitis in beard area.
- Tinea Unguium (Onychomycosis): Nail discoloration, thickening, subungual debris. Distal Lateral Subungual Onychomycosis (DLSO) common.
- Tinea Faciei (Face): Annular lesions on non-bearded face; often photosensitive distribution if topical steroids misused (tinea incognito).
Diagnostic Methods - Spotting Spores
- KOH Mount (10-20%): Primary test. Skin/nail/hair scrapings. Dissolves keratin, reveals septate hyphae & arthrospores.
⭐ Calcofluor white stain under fluorescent microscope provides rapid and brilliant visualization of fungal elements.
- Fungal Culture: Gold standard for species ID. Sabouraud Dextrose Agar (SDA) ± antibiotics. Dermatophyte Test Medium (DTM) shows color change (yellow → red).
- Wood's Lamp (UV 365nm): Greenish fluorescence with some Microsporum spp. (e.g., M. canis). Not all fluoresce.
- Biopsy: PAS/GMS stains for atypical/deep infections.

Management Strategies - Kicking Keratin-lovers
- Goal: Eradicate infection, prevent recurrence.
- General: Hygiene, dry skin, loose cotton clothing.
- Tinea Capitis: Systemic therapy essential (Griseofulvin/Terbinafine). Add antifungal shampoo (Ketoconazole/Selenium sulfide).
- Onychomycosis: Systemic preferred (Terbinafine/Itraconazole).
- ⚠️ Avoid irrational steroid combinations; risk of Tinea Incognito.
⭐ Terbinafine is fungicidal via squalene epoxidase inhibition; Azoles are generally fungistatic via 14-α-demethylase inhibition, targeting lanosterol demethylation to ergosterol.
Special Aspects - Tricky Tineas
- Tinea Incognito: Steroid-modified, ↓inflammation, atypical presentation.
- Majocchi's Granuloma: Deep follicular invasion (T. rubrum), often legs, immunocompromised.
- Tinea Imbricata: Concentric scaly rings ("Tokelau"), T. concentricum.
- Favus (Tinea Capitis): T. schoenleinii, scutula (yellow crusts), scarring alopecia.
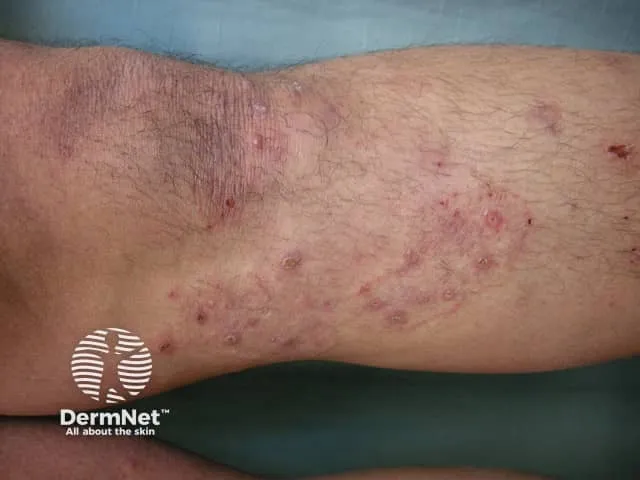
⭐ Majocchi's granuloma is a deep fungal folliculitis, commonly on legs of women (shaving) or in immunocompromised patients.
High‑Yield Points - ⚡ Biggest Takeaways
- Dermatophytes (Trichophyton, Microsporum, Epidermophyton) are keratinophilic fungi infecting skin, hair, and nails.
- Tinea corporis (ringworm) typically presents as annular lesions with central clearing and an active, erythematous border.
- Diagnosis is confirmed by KOH mount of skin scrapings showing septate hyphae; Wood's lamp helps identify some Microsporum species (e.g., M. canis fluoresces green).
- Tinea capitis often requires systemic antifungal therapy (e.g., griseofulvin, terbinafine), especially for endothrix infections.
- Onychomycosis (tinea unguium) is challenging to treat, usually necessitating prolonged oral antifungals like terbinafine or itraconazole.
- Treatment involves topical antifungals (azoles, allylamines) for localized infections, and oral agents for extensive disease, hair/nail involvement, or failed topical therapy.
- An Id reaction (dermatophytid) is a sterile, allergic hypersensitivity rash at a distant site from the primary fungal infection, not representing spread of infection.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more