ACD Basics - Skin's Delayed Fury
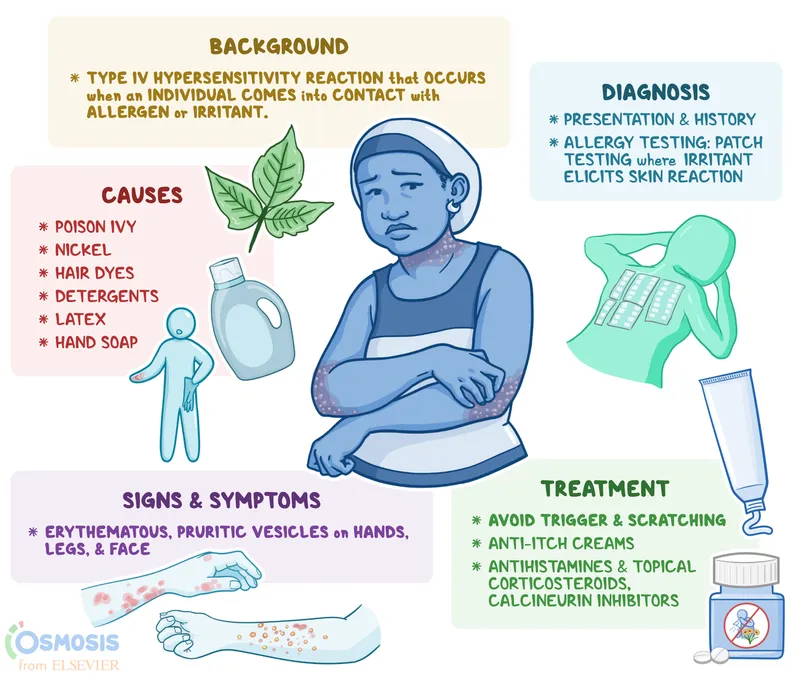
- Definition: Allergic Contact Dermatitis (ACD) is an immune-mediated, delayed (Type IV) hypersensitivity reaction to an external allergen. Unlike Irritant Contact Dermatitis (ICD), which is direct non-immune tissue damage. 📌 ACD = Allergen Causes Delayed reaction.
- Pathophysiology (Type IV Hypersensitivity):
⭐ ACD is a classic example of a Type IV hypersensitivity reaction mediated by T-lymphocytes.
Allergen Parade - The Usual Suspects
📌 For common metals: No Chrome Contact (Nickel, Cobalt, Chromium).
| Allergen | Common Sources (India Focus) | Key Notes / Cross-reactions |
|---|---|---|
| Nickel | Artificial jewelry, coins, buckles, jean studs | Cross-reacts: Cobalt, Palladium |
| Potassium dichromate | Cement (construction), leather, paints, matches | Cross-reacts: Cobalt |
| Paraphenylenediamine (PPD) | Hair dyes, "black henna" tattoos, some textiles | Cross-reacts: Azo dyes, sulfonamides, PABA |
| Fragrance Mix | Cosmetics, perfumes, soaps, toiletries | Cross-reacts: Balsam of Peru, colophony |
| Preservatives | Cosmetics, creams (parabens, formaldehyde-releasers) | Patch testing often needed |
| Parthenium hysterophorus | "Congress grass" (common airborne weed) | Significant plant dermatitis cause in India |
| Urushiol | Mango sap, marking nut (bhilawan), cashew shell | Family: Anacardiaceae; potent sensitizer |
| Topical Medications | Neomycin creams, some topical corticosteroids | Neomycin cross-reacts: other aminoglycosides |
⭐ Parthenium dermatitis is a significant cause of airborne contact dermatitis in India.
Rash Report - Itch & Tell
- Onset: 24-72 hours post-exposure in sensitized individuals.
- Morphology:
- Acute: Erythema, edema, vesicles/bullae (may be tense), oozing, intense pruritus.
- Subacute: Scaling, crusting, less vesicular, resolving erythema.
- Chronic: Lichenification (thickened skin), fissuring, hyper/hypopigmentation, dryness.
- Distribution:
- Often sharply demarcated, localized to site of direct contact.
- Linear streaks: Plant contact (e.g., Poison Ivy, Parthenium - 📌 think "streaky rash from a leafy dash").
- Specific Patterns: Consider: Earlobes (nickel), eyelids (cosmetics, nail polish transfer), feet (footwear components like chromates, rubber).
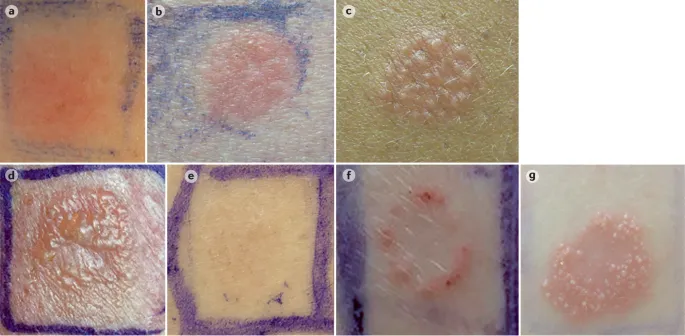
⭐ The presence of well-demarcated, eczematous lesions in an area of allergen exposure is highly suggestive of ACD.
Patch Test Puzzles - Finding Culprits
- History is Key: Occupation, hobbies, cosmetics, topicals, clothing, jewelry.
- Patch Testing: Gold Standard
- Identifies specific allergen.
- Technique: Allergens applied, readings at 48 & 72/96 hrs.
- Interpretation: + (weak), ++ (strong), +++ (extreme), IR (irritant).
- Series: Indian Standard Series.

- Differential Diagnosis:
- Irritant Contact Dermatitis (ICD)
- Atopic Dermatitis
- Seborrheic Dermatitis
- Psoriasis
- Fungal infections
⭐ A positive patch test must be clinically relevant to the patient's dermatitis to confirm ACD.
Soothe & Shield - Calming Chaos
- Cornerstone: Allergen identification & strict avoidance.
- Patient Education: Allergen sources, cross-reactants, alternative products.
- Topical Therapy:
- Corticosteroids: Potency based on site/severity.
- Topical Calcineurin Inhibitors (TCIs): e.g., Tacrolimus, Pimecrolimus for sensitive areas, long-term use.
- Systemic Therapy (Severe/Widespread ACD):
- Oral Corticosteroids: e.g., Prednisolone $0.5-1 \text{ mg/kg/day}$ tapered over 2-3 weeks.
- Antihistamines: For pruritus.
- Supportive Care: Emollients, wet compresses.
⭐ Short courses of potent topical steroids are preferred over long courses of weaker steroids to minimize side effects.
High‑Yield Points - ⚡ Biggest Takeaways
- Type IV hypersensitivity reaction, delayed onset (24-72 hours post-exposure).
- Common allergens: nickel (jewelry), poison ivy (urushiol), fragrances, preservatives, PPD (hair dye).
- Clinical: intensely pruritic, erythematous papules/vesicles, well-demarcated at contact site.
- Patch testing is gold standard for diagnosis, identifies specific allergen.
- Management: strict allergen avoidance, topical corticosteroids (mainstay), emollients; systemic steroids for severe/widespread.
- Chronic ACD: lichenification, scaling, fissuring; may become generalized or id reaction (autosensitization).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

