Plasma Proteins Overview - The Blood's Workhorses
Total plasma protein: 6.0-8.3 g/dL. Primarily synthesized in the liver (except γ-globulins from plasma cells).
-
Core Functions:
- Oncotic pressure (key: albumin)
- Transport (e.g., hormones, drugs, lipids)
- Buffering (acid-base balance)
- Immunity (γ-globulins/antibodies)
- Coagulation (e.g., fibrinogen)
-
Major Classes & Primary Roles:
- Albumin: Highest concentration; maintains oncotic pressure, transport.
- Globulins:
- α1, α2: Transport, protease inhibitors.
- β: Transport (e.g., iron via transferrin, lipids via LDL).
- γ (Immunoglobulins): Antibodies for immunity.
- Fibrinogen: Essential for blood clotting.
-
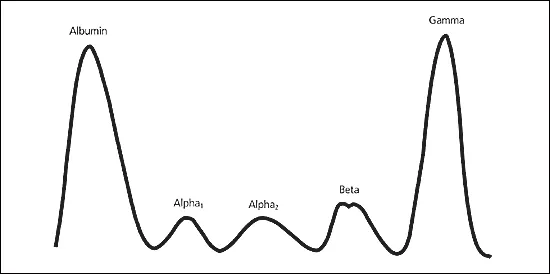
Analysis - SPEP: Serum Protein Electrophoresis separates into 5 bands: Albumin, α1, α2, β, and γ globulins.
⭐ Most plasma proteins are glycoproteins, except for albumin.
Albumin Focus - Osmotic & Transport Titan
- Most abundant plasma protein (~60% of total; 3.5-5.0 g/dL).
- Structure: Single polypeptide chain; no carbohydrate (CHO).
- Functions:
- Major contributor to plasma oncotic pressure (~80%).
- Versatile transport: Bilirubin, fatty acids, Ca²⁺, hormones, drugs (e.g., warfarin, salicylates).
- Buffering (minor physiological role).
- Synthesis: Exclusively in the liver.
- Acute Phase Reactant: Negative (levels ↓ during inflammation).
- Hypoalbuminemia (<3.5 g/dL):
- Causes: 📌 NALS (Nephrotic syndrome, Anorexia/Malnutrition, Liver cirrhosis, Severe burns/Skin loss).
- Consequences: Generalized edema (peripheral, pulmonary, ascites).
⭐ Edema typically occurs when serum albumin levels fall below 2.0-2.5 g/dL.
- Hyperalbuminemia (>5.0 g/dL):
- Causes: Primarily severe dehydration.
- Analbuminemia: Rare congenital disorder (virtual absence of albumin).

Globulins Deep Dive - Defense & Delivery Crew
- Heterogeneous group; separated by electrophoresis (e.g., SPEP).
| Type | Key Proteins & Core Function | Clinical Correlations |
|---|---|---|
| α1-Globulins | - α1-Antitrypsin (AAT): Protease inhibitor - α-Fetoprotein (AFP): Fetal marker | - AAT def: Emphysema, liver dz - AFP: ↑ HCC, neural tube defects (NTDs) |
| α2-Globulins | - Ceruloplasmin: Cu transport, ferroxidase - Haptoglobin: Binds free Hb - α2-Macroglobulin: Protease inhib. | - Ceruloplasmin: ↓ Wilson's dz - Haptoglobin: ↓ Hemolysis - α2-Macro: ↑ Nephrotic synd. |
| β-Globulins | - Transferrin: Fe transport - β2-Microglobulin: MHC I component - CRP: Major APR | - Transferrin: ↑ Fe deficiency anemia - β2-Micro: ↑ Renal failure, malignancies - CRP: ↑ Inflammation |
| γ-Globulins | - Immunoglobulins (Igs e.g., IgG, IgM): Antibodies from plasma cells | - Altered in immune disorders, infections, paraproteinemias (e.g., Myeloma) |
⭐ A decreased or absent α1-globulin band on SPEP is highly suggestive of α1-antitrypsin deficiency.
Fibrinogen & Others - Clotting & Crisis Responders
-
Fibrinogen (Factor I): Synthesized in the liver. Crucial for blood coagulation; converted to fibrin by thrombin.
- Normal range: 200-400 mg/dL.
- Conditions: Afibrinogenemia (absence), dysfibrinogenemia (abnormal function).
-
Acute Phase Reactants (APRs): Proteins whose plasma levels change significantly with inflammation/tissue injury (stimuli: IL-1, IL-6, TNF-α).
- Positive APRs (↑): C-Reactive Protein (CRP), Fibrinogen, Haptoglobin, Ceruloplasmin, Alpha-1 Antitrypsin (A1AT), Ferritin, Serum Amyloid A (SAA).
- Negative APRs (↓): Albumin, Transferrin, Prealbumin (Transthyretin).
-
Plasma Protein Electrophoresis (SPEP) Patterns:
- Nephrotic Syndrome: ↓ Albumin, ↑ α2-macroglobulin, ↓ γ-globulins.
- Liver Cirrhosis: Polyclonal gammopathy (broad ↑ γ-globulins), β-γ bridging.
- Multiple Myeloma: Monoclonal gammopathy (M-spike).
⭐ In multiple myeloma, the M-spike is most commonly due to monoclonal IgG, followed by IgA.
High‑Yield Points - ⚡ Biggest Takeaways
- Albumin: Most abundant plasma protein, synthesized in the liver; maintains oncotic pressure and acts as a transporter.
- Hypoalbuminemia: Key cause of generalized edema.
- α1-Antitrypsin deficiency: Associated with early-onset emphysema and liver cirrhosis.
- Ceruloplasmin: Primary copper-carrying protein; decreased in Wilson's disease.
- Haptoglobin: Binds free hemoglobin; levels decrease significantly in intravascular hemolysis.
- Transferrin: Major iron transport protein; levels increase in iron-deficiency anemia.
- Acute phase reactants (e.g., CRP, fibrinogen) are altered during inflammation; albumin is a negative acute phase reactant (levels ↓).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

