Metabolic Syndrome - Defining the Danger
Prothrombotic, proinflammatory state. Diagnosis: ≥3 of 5 criteria (📌).
| Criterion | NCEP ATP III (Any ≥3) | IDF (Central Obesity + ≥2) |
|---|---|---|
| Waist | >102/88 cm (Ind: >90/80) | Required (Ethnic-spec.) |
| ↑ TG | ≥150 mg/dL (Rx) | ≥150 mg/dL (Rx) |
| ↓ HDL-C | <40/50 mg/dL (M/F, Rx) | <40/50 mg/dL (M/F, Rx) |
| ↑ BP | ≥130/85 mmHg (Rx) | ≥130/85 mmHg (Rx) |
| ↑ Fasting Glc | ≥100 mg/dL (Rx) | ≥100 mg/dL (or T2DM) |
⭐ NCEP ATP III criteria are widely used for diagnosing Metabolic Syndrome, requiring at least three out of five specific risk factors.
Pathophysiology - Insulin's Resistance Riot
- Core Defect: Insulin Resistance (IR) - liver, muscle, adipose cells resist insulin action.
- Primary Drivers of IR:
- Visceral Adiposity: Central fat.
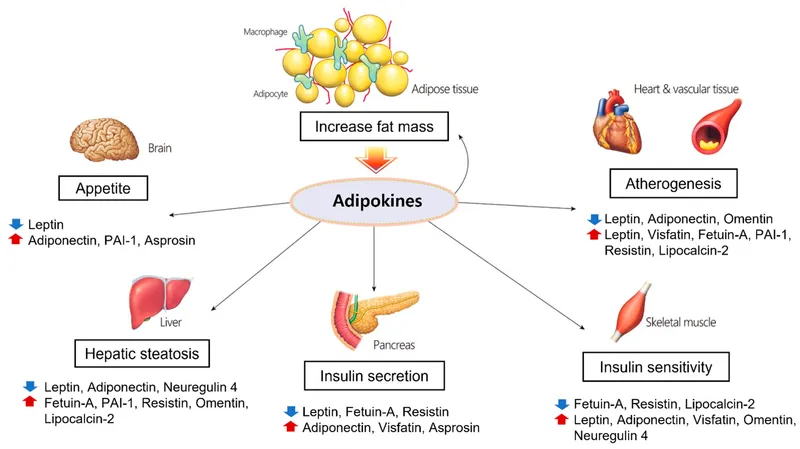
- Alters adipokine secretion:
- ↓ Adiponectin (sensitizing).
- ↑ TNF-α, ↑ Resistin (pro-IR).
- Alters adipokine secretion:
- Chronic Inflammation & Oxidative Stress.
- Genetics & Lifestyle (diet, inactivity).
- Visceral Adiposity: Central fat.
⭐ Insulin resistance, often driven by visceral adiposity and altered adipokine secretion (e.g., ↓adiponectin, ↑TNF-α, ↑resistin), is the central pathophysiological mechanism in Metabolic Syndrome.
- Consequences (The "Riot"):
- Hyperinsulinemia: Compensatory; β-cell failure risk.
- Hyperglycemia: ↓Muscle uptake, ↑hepatic output.
- Atherogenic Dyslipidemia: ↑TGs, ↓HDL-C, ↑small dense LDL (sdLDL).
- Hypertension: Endothelial dysfunction, ↑SNS, ↑RAAS.
- Pro-inflammatory/thrombotic state.
Clinical Impact - The Body's Alarms
⭐ Metabolic Syndrome significantly elevates the risk of developing Type 2 Diabetes Mellitus (up to 5-fold) and atherosclerotic Cardiovascular Disease (up to 2-fold).
- Systemic Consequences & Associated Conditions:
- Endocrine:
- Type 2 Diabetes Mellitus (T2DM): Due to insulin resistance.
- Polycystic Ovary Syndrome (PCOS) in women.
- Cardiovascular:
- Atherosclerotic CVD (ASCVD): Myocardial Infarction (MI), Stroke, Peripheral Artery Disease.
- Hypertension: Often a core component.
- Hepatic:
- Non-alcoholic Fatty Liver Disease (NAFLD), progressing to Non-alcoholic steatohepatitis (NASH), fibrosis, cirrhosis.
- Renal:
- Chronic Kidney Disease (CKD), microalbuminuria.
- Respiratory:
- Obstructive Sleep Apnea (OSA).
- Musculoskeletal:
- Gout (Hyperuricemia).
- Oncologic:
- ↑ Risk of certain cancers (e.g., colorectal, breast, endometrial).
- Endocrine:
- Overall Impact: ↑ All-cause mortality, ↓ Quality of life.
Management - Reversing the Risks
⭐ Lifestyle modification, including dietary changes (e.g., DASH or Mediterranean diet), increased physical activity (≥150 min/week moderate intensity), and weight reduction, is the cornerstone of Metabolic Syndrome management.
Management is comprehensive, targeting risk factor reduction. 📌 Mnemonic: ABCDE (Assess risk/Aspirin, Blood pressure, Cholesterol/Cigarettes, Diet/Diabetes, Exercise).
- Core Strategy: Aggressive lifestyle changes are paramount.
- Pharmacological Aid: Medications address individual components if lifestyle targets are not met.
- Prioritize agents with benefits beyond single risk factors (e.g., ACEi/ARBs in diabetes).
- Surgical Option: Bariatric surgery for refractory severe obesity.
- Monitoring: Regular follow-up to assess efficacy and adjust therapy.
High‑Yield Points - ⚡ Biggest Takeaways
- Metabolic Syndrome: Cluster of ≥3 risk factors: central obesity, ↑ triglycerides (≥150 mg/dL), ↓ HDL-C (<40M/<50F mg/dL), ↑ BP (≥130/85 mmHg), ↑ fasting glucose (≥100 mg/dL).
- Insulin resistance is the core mechanism.
- Diagnosis by NCEP ATP III criteria (3 of 5).
- Significantly ↑ risk for CVD, Type 2 DM, and NAFLD.
- Altered adipokines (e.g., ↓ adiponectin, ↑ TNF-α) contribute.
- Lifestyle modification (diet, exercise) is primary treatment.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

