Porphyrias: Heme Synthesis & Intro - Pathway Puzzles
- Porphyrias: Inherited disorders from enzyme defects in heme biosynthesis pathway. Each defect is a "puzzle piece".
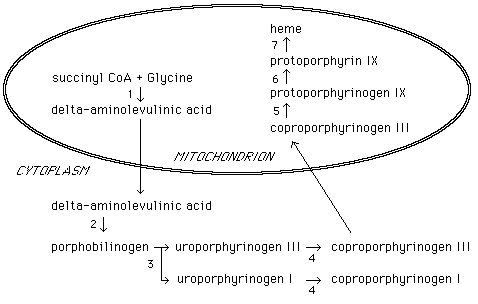
- Heme: Essential iron-porphyrin for hemoglobin, myoglobin, cytochromes. Synthesis in mitochondria & cytosol.
- Key Steps: Glycine + Succinyl CoA $\xrightarrow{\text{ALAS}}$ $\delta$-ALA $\rightarrow$ Porphobilinogen (PBG) $\rightarrow \dots \rightarrow$ Protoporphyrin IX + $Fe^{2+}$ $\xrightarrow{\text{Ferrochelatase}}$ Heme.
⭐ ALA synthase (ALAS) is the rate-limiting enzyme in heme synthesis and is feedback inhibited by heme.
- Defect $\rightarrow$ ↑ specific precursor $\rightarrow$ unique porphyria type & symptoms.
Porphyrias: Classification - Symptom Sorting
- Primary Site of Defect:
- Hepatic: Defect in liver (e.g., AIP, PCT, VP, HCP).
- Erythropoietic: Defect in bone marrow (e.g., CEP, EPP).
- Clinical Presentation (Symptom-Based):
- Acute (Neurovisceral): Severe abdominal pain, neuropathy, psychiatric symptoms. Urine may darken.
- Examples: AIP, ADP, VP, HCP.
- Cutaneous (Photosensitive): Skin fragility, blisters, scarring on sun-exposed areas.
- Examples: PCT, EPP, CEP.
- Mixed: VP & HCP exhibit both neurovisceral and cutaneous features.
- Acute (Neurovisceral): Severe abdominal pain, neuropathy, psychiatric symptoms. Urine may darken.
⭐ Acute porphyrias (e.g., AIP) are characterized by neurovisceral symptoms, while non-acute/cutaneous porphyrias (e.g., PCT) primarily manifest with photosensitivity.
Porphyrias: Acute (AIP) - Neurovisceral Vexations
- Acute Intermittent Porphyria (AIP): Most common acute type. Autosomal dominant.
- Defect: ↓ Hydroxymethylbilane synthase (HMBS) / Porphobilinogen deaminase (PBGD).
- Accumulation: Porphobilinogen (PBG) & Aminolevulinic acid (ALA).
- Clinical (Neurovisceral Attacks):
- 📌 AIP's 5 P's: Pain (severe abdominal), Peripheral neuropathy, Psychological disturbances, Pee (port-wine colored), Precipitated by drugs (barbiturates, sulfonamides), stress, fasting.
- Diagnosis (Acute Attack):
- ↑↑ Urinary PBG (key) & ALA.
- DNA testing confirms.
⭐ Elevated urinary porphobilinogen (PBG) is pathognomonic for acute attacks of AIP, HCP, and VP.
- Management:
- Acute: IV Hemin (3-4 mg/kg IV daily for 4 days), glucose.
- Avoid precipitants.
- Flowchart: AIP Pathogenesis
Porphyrias: Cutaneous (PCT) - Dermal Dramas
- Most common porphyria; adult onset.
- Defect: Uroporphyrinogen decarboxylase (UROD). Accumulation of uroporphyrinogen.
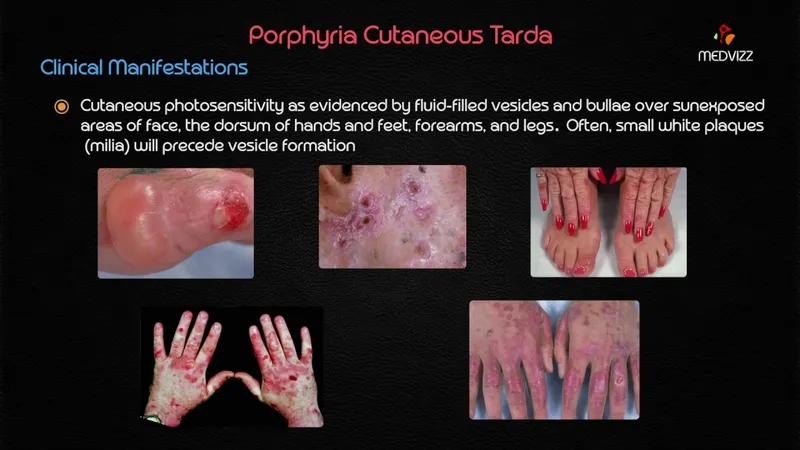
- Clinical: Photosensitivity (blisters, erosions, fragility on sun-exposed areas), hyperpigmentation, hypertrichosis. No acute attacks.
- Triggers: 📌 IAESH (Iron, Alcohol, Estrogen, Hepatitis C, Smoking), HIV.
- Diagnosis:
- ↑ Urine uroporphyrins (Type I > III); pink/red urine, coral-pink fluorescence (Wood's lamp).
- ↑ Plasma porphyrins (peak ~620 nm).
- ↑ Fecal isocoproporphyrin.
- Normal ALA/PBG.
- Management: Phlebotomy (ferritin <50 ng/mL), low-dose hydroxychloroquine/chloroquine. Avoid triggers, sun protection.
⭐ Porphyria Cutanea Tarda (PCT) is the most common porphyria, characterized by photosensitive skin lesions and elevated uroporphyrins in urine.
High‑Yield Points - ⚡ Biggest Takeaways
- Porphyrias: Inherited enzyme defects in heme synthesis pathway.
- Acute Intermittent Porphyria (AIP): PBG deaminase defect; neurovisceral symptoms (pain, neuropathy), port-wine urine, no photosensitivity. Triggered by drugs.
- Porphyria Cutanea Tarda (PCT): Uroporphyrinogen decarboxylase defect; most common; photosensitivity, blisters, tea-colored urine.
- Erythropoietic Protoporphyria (EPP): Ferrochelatase defect; photosensitivity (non-blistering), risk of gallstones, liver disease.
- Lead poisoning inhibits ALA dehydratase & ferrochelatase, mimicking porphyria.
- AIP treatment: glucose, hemin. Avoid precipitants for all.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

