Assay Principles - Hormones Under Scope
- Immunoassays: Core of hormone measurement.
- Competitive: Labeled & unlabeled hormone compete for limited antibody sites. Signal $\propto$ 1/[Analyte].
- Non-competitive (Sandwich): Analyte captured between two antibodies. Signal $\propto$ [Analyte].
- Key Techniques:
- ELISA: Enzyme-linked, colorimetric/fluorometric signal.
- RIA: Radiolabeled antigen ($^{125}$I), highly sensitive.
- CLIA: Chemiluminescent signal, high sensitivity & wide range.
- LC-MS/MS: Gold standard for steroids; high specificity & multiplexing.
- Hormones Covered: Thyroid (TSH, T3, T4), PTH, Cortisol, Aldosterone, GH, ACTH, Prolactin, Insulin, Estrogen, Testosterone, hCG.

⭐ Free hormone fractions (e.g., fT4, fTestosterone) often better reflect biological activity than total hormone levels, as they are unbound to proteins.
Pituitary & Thyroid - Master Regulators
- Pituitary Gland:
- Anterior Lobe: Secretes TSH, ACTH, GH, PRL, FSH, LH. 📌 Mnemonic: FLAT PiG.
- TSH (Thyrotropin): Stimulates thyroid hormone (T3, T4) synthesis/release. Regulated by hypothalamic TRH (+) and thyroid hormone (-).
- Posterior Lobe: Stores & releases ADH, Oxytocin (synthesized in hypothalamus).
- Anterior Lobe: Secretes TSH, ACTH, GH, PRL, FSH, LH. 📌 Mnemonic: FLAT PiG.
- Thyroid Gland:
- Hormones: Thyroxine (T4), Triiodothyronine (T3), Calcitonin.
- T4 is prohormone; converted to T3 (more potent) in periphery by deiodinases.
- Binding proteins: TBG (Thyroxine-binding globulin) carries most T4/T3.
- Hypothalamic-Pituitary-Thyroid (HPT) Axis:
- Thyroid Function Tests (TFTs) Interpretation:
- TSH: Best initial screening. Normal: 0.4-4.0 mIU/L.
- Primary Hypothyroidism: ↑ TSH, ↓ Free T4.
- Primary Hyperthyroidism: ↓ TSH, ↑ Free T4.
- Subclinical Hypothyroidism: ↑ TSH, Normal Free T4.
- Anti-TPO Abs: Hashimoto's. TSH-Receptor Abs (TSI): Graves' disease.
- TSH: Best initial screening. Normal: 0.4-4.0 mIU/L.
⭐ TSH is the most sensitive indicator of primary thyroid dysfunction; changes in TSH often precede changes in T4/T3 levels.
Adrenal & Gonadal - Stress & Sex Hormones
- Adrenal Cortex:
- Cortisol (Glucocorticoid): Stress response, ↑glucose. Reg: CRH-ACTH-Cortisol.
- Tests: Dexamethasone suppression, ACTH stimulation, 24hr Urinary Free Cortisol (UFC).
- Disorders: Cushing's syndrome (↑cortisol), Addison's disease (↓cortisol).
- Aldosterone (Mineralocorticoid): Na⁺/H₂O reabsorption, K⁺ excretion, BP control. Reg: RAAS, K⁺.
- Tests: Aldosterone:Renin Ratio (ARR). Conn's syndrome (↑aldosterone).
- Adrenal Androgens (DHEA, DHEAS): Precursors to sex hormones.
- Test: 17-hydroxyprogesterone (17-OHP) for Congenital Adrenal Hyperplasia (CAH).
- Cortisol (Glucocorticoid): Stress response, ↑glucose. Reg: CRH-ACTH-Cortisol.
- Adrenal Medulla:
- Catecholamines (Epinephrine, Norepinephrine): Fight-or-flight.
- Test: Plasma/Urinary Metanephrines, Vanillylmandelic Acid (VMA) for Pheochromocytoma.
- Catecholamines (Epinephrine, Norepinephrine): Fight-or-flight.
- Gonadal Hormones:
- Testosterone (Androgen): Male 2° sexual characteristics, spermatogenesis.
- Tests: Total/Free Testosterone, LH, FSH.
- Estrogen (Estradiol) & Progesterone: Female 2° sexual characteristics, menstrual cycle, pregnancy.
- Tests: Estradiol, Progesterone, LH, FSH. Polycystic Ovary Syndrome (PCOS) common.
- Testosterone (Androgen): Male 2° sexual characteristics, spermatogenesis.
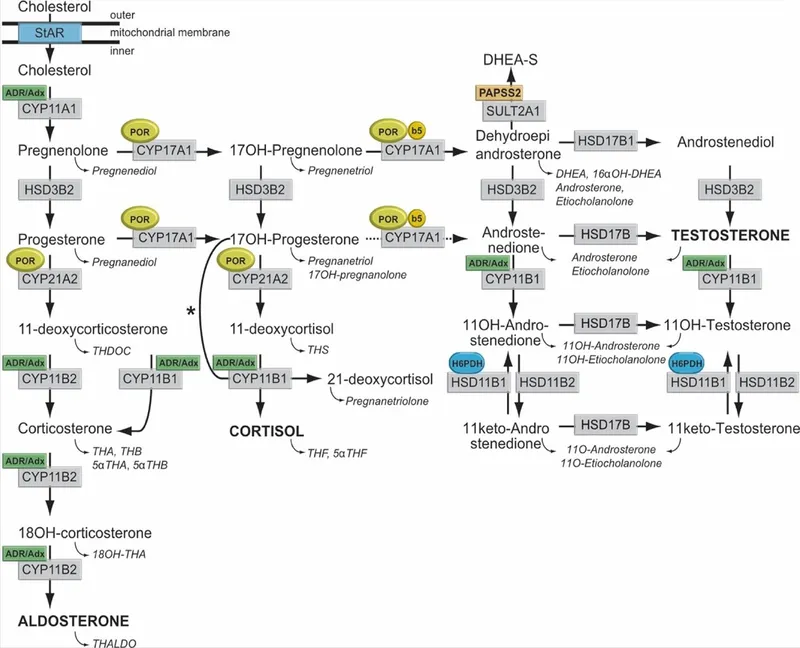
⭐ 21-Hydroxylase deficiency is the most common CAH cause: ↓cortisol, ↓aldosterone, ↑androgens. Presents with salt wasting & virilization (females).
Pancreas & Calcium - Metabolic Managers
- Pancreatic Hormones:
- Insulin (β-cells): Anabolic. ↓ Blood glucose. C-peptide reflects endogenous insulin.
- Glucagon (α-cells): Catabolic. ↑ Blood glucose, glycogenolysis, gluconeogenesis.
- Somatostatin (δ-cells): Universal inhibitor (insulin, glucagon, GH).
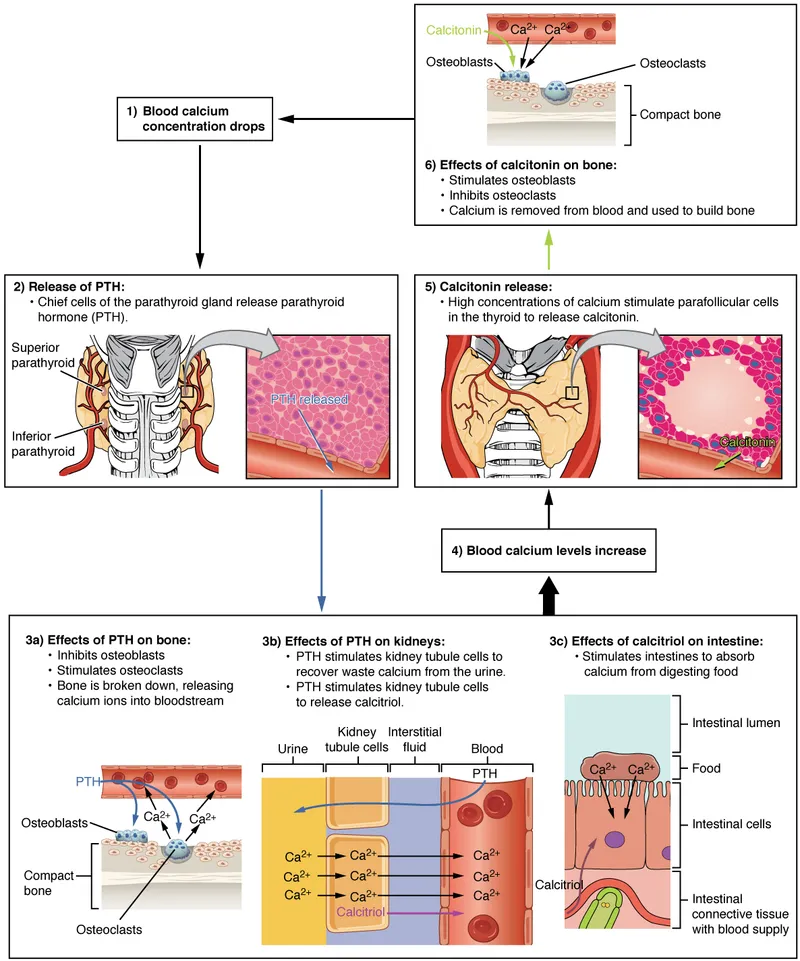
- Calcium Homeostasis:
- PTH: ↑ Serum $Ca^{2+}$, ↓ Serum $PO_4^{3-}$ (📌 Phosphate Trashing Hormone). Stimulates osteoclasts, renal $Ca^{2+}$ reabsorption, Vit D activation.
- Vitamin D ($1,25(OH)_2D_3$): ↑ Intestinal $Ca^{2+}$ & $PO_4^{3-}$ absorption.
- Calcitonin (Thyroid C-cells): Weakly ↓ Serum $Ca^{2+}$ by inhibiting osteoclasts.
⭐ Primary hyperparathyroidism classically presents with high PTH, high serum calcium, low serum phosphate, and increased urinary cAMP.
High‑Yield Points - ⚡ Biggest Takeaways
- Immunoassays (ELISA, RIA, CLIA) are mainstay for hormone quantification.
- Dynamic function tests (e.g., Dexamethasone suppression) assess endocrine reserve/autonomy.
- Free hormone levels (e.g., FT4) better reflect bioactivity than total hormone levels.
- Pulsatile secretion (LH) & diurnal variation (cortisol) demand timed/pooled sampling.
- Assay interferences (e.g., HAMA) can cause falsely high or low results.
- Interpret results with clinical context, considering age, sex, pregnancy, and medications.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more