Maternal Physiology in High-Risk Pregnancy - Body Under Duress
- Normal pregnancy adaptations are stressed, often decompensating.
- Cardiovascular:
- ↑Cardiac Output (CO) (30-50%) faces limits (e.g., cardiac disease).
- Preeclampsia: ↑Systemic Vascular Resistance (SVR), vasospasm, endothelial dysfunction.
- Peripartum cardiomyopathy: Left ventricular dysfunction.
- Respiratory:
- ↓Functional Residual Capacity (FRC) (~20%) worsens (obesity, multiple gestations); rapid desaturation risk.
- ↑O2 consumption.
- Hematological:
- Exaggerated hypercoagulability (e.g., Antiphospholipid Syndrome - APLAS).
- Thrombocytopenia (e.g., HELLP, ITP); anemia often severe.
- Renal & Hepatic:
- Preeclampsia: Proteinuria, ↓Glomerular Filtration Rate (GFR). HELLP: ↑Liver Function Tests (LFTs), liver dysfunction.
- Gastrointestinal (GI): ↑Aspiration risk (obesity, diabetes, GERD).
⭐ In severe preeclampsia, intravascular volume is often decreased despite generalized edema, due to capillary leak and endothelial dysfunction, complicating fluid management.
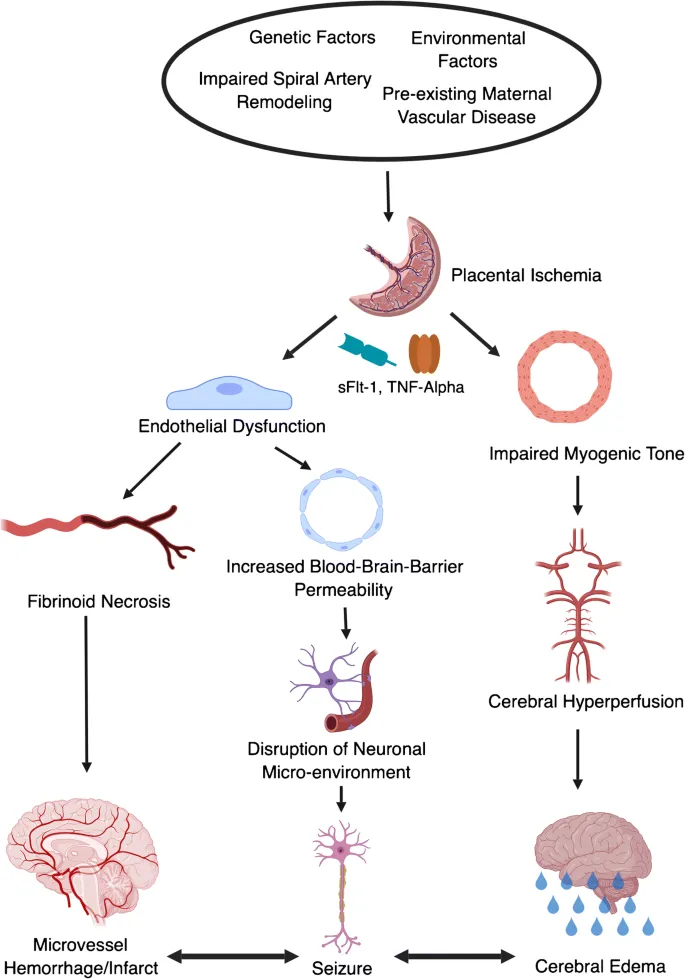
Hypertensive Disorders - Pressure Point Perils
-
Spectrum:
- Chronic HTN: BP ≥ 140/90 mmHg <20 wks gestation.
- Gestational HTN: BP ≥ 140/90 mmHg >20 wks, no proteinuria.
- Preeclampsia: HTN >20 wks + Proteinuria (≥300mg/24h) OR end-organ damage (e.g., BP ≥ 160/110 mmHg, Plt <100,000/µL, ↑LFTs, Cr >1.1 mg/dL, pulmonary edema, cerebral/visual symptoms).
- Eclampsia: Preeclampsia + Seizures.
- HELLP Syndrome: Hemolysis, Elevated Liver enzymes, Low Platelets.
-
Anesthetic Goals:
- Seizure control ($MgSO_4$).
- BP control (Labetalol, Hydralazine); Target SBP 140-155 mmHg, DBP 90-105 mmHg.
- Judicious fluid management.
- Safe delivery (neuraxial preferred if no contraindications).
-
Key Anesthetic Points:
- ↑Airway edema risk; careful airway assessment.
- $MgSO_4$: Potentiates neuromuscular blockers (NMBs). Monitor for toxicity (↓DTRs, respiratory depression). Antidote: Calcium gluconate.
- Neuraxial (epidural/spinal): Preferred if Platelets >70,000-80,000/µL & no coagulopathy.
- General Anesthesia (GA): Rapid Sequence Intubation (RSI). Attenuate pressor response to laryngoscopy.
- HELLP: High risk of bleeding/hematoma. Neuraxial often contraindicated.
⭐ Magnesium sulfate is the drug of choice for eclampsia seizure prophylaxis and treatment; therapeutic range 4.8-8.4 mg/dL (2-3.5 mmol/L).
Obstetric Hemorrhage - Code Red Crisis
- Life-threatening bleeding: Antepartum (APH) or Postpartum (PPH).
- PPH: Blood loss >500mL (vaginal), >1000mL (CS) in 24h.
- 📌 PPH Causes (4 T's):
- Tone: Atony (70-80%). Uterotonics.
- Trauma: Lacerations, rupture. Repair.
- Tissue: Retained products. Evacuate.
- Thrombin: Coagulopathy. Correct.
- CODE RED Protocol:
- Team alert (OB, Anesthesia, Blood Bank).
- 2 large IVs, O₂, warming. Monitor Shock Index ($SI = HR/SBP$).
- MTP: PRBC:FFP:Platelets 1:1:1. Consider Calcium.
- Anesthesia: Regional (stable) vs. GA (unstable/urgent).
⭐ Tranexamic acid (TXA) 1g IV within 3h of PPH onset reduces bleeding deaths. Repeat dose if bleeding continues after 30 min or restarts within 24h.

Coexisting Medical Conditions - Complex Challenges
- Cardiac Disease:
- NYHA class guides risk; aim for ↓cardiac stress, maintain perfusion.
- Epidural ideal (slow onset, stable hemodynamics).
- Avoid: Ketamine (↑HR/BP), Ergometrine (↑BP).
- Mitral Stenosis: Maintain HR & preload; avoid tachycardia, fluid overload.
- Aortic Stenosis: Maintain SVR crucial; avoid spinal hypotension.
- Eisenmenger's: Very high maternal mortality; strictly avoid ↓SVR, hypoxia.
- Diabetes Mellitus:
- Risks: Macrosomia, neonatal hypoglycemia.
- Goal: Euglycemia; epidural preferred.
- GA: Monitor glucose; DKA risk.
- Obesity (BMI >30 kg/m²):
- Challenges: Airway, IV access, regional anesthesia.
- ↑Risks: GDM, OSA, VTE; drug dose adjustments.
- Asthma:
- Optimize pre-op; regional preferred.
- GA: Ketamine, sevoflurane. ⚠️ PGF2α (Carboprost) contraindicated (bronchospasm).
⭐ Parturients with severe mitral stenosis are highly sensitive to changes in heart rate; maintaining sinus rhythm and avoiding tachycardia is crucial.
High-Yield Points - ⚡ Biggest Takeaways
- Preeclampsia/Eclampsia: Magnesium sulfate for seizures; neuraxial if platelets >70k & no coagulopathy.
- HELLP Syndrome: Severe preeclampsia variant; high risk of epidural hematoma with neuraxial.
- Placenta Previa/Accreta: Anticipate massive hemorrhage; GA often for accreta, ensure blood.
- Amniotic Fluid Embolism: Sudden CV collapse, hypoxia, DIC; aggressive supportive care.
- Cardiac Disease (e.g., Eisenmenger): Maintain hemodynamic stability; GA often for severe cases.
- Morbid Obesity: Increased difficult airway risk; neuraxial preferred, careful positioning.
- Antepartum Hemorrhage: Rapid resuscitation and urgent delivery are critical.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

