Venous Thromboembolism - Clot Chaos Intro
- VTE: Pathological clot formation in veins. Spectrum: Deep Vein Thrombosis (DVT) - common in legs; Pulmonary Embolism (PE) - clot travels to lungs.
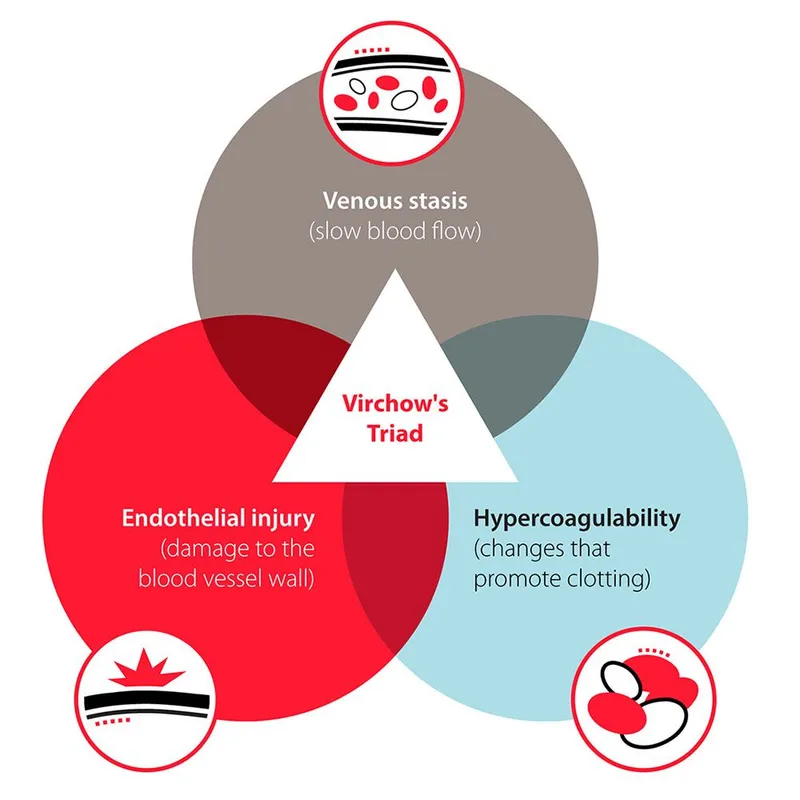
- Pathophysiology: Virchow's Triad 📌 (SHE):
- Stasis (e.g., immobility, post-op)
- Hypercoagulability (e.g., Factor V Leiden, malignancy, OCPs)
- Endothelial injury (e.g., trauma, central lines)
- Classification:
- Provoked: Due to transient risk factor (surgery, trauma).
- Unprovoked: Idiopathic; higher recurrence risk.
⭐ Factor V Leiden is the most common inherited thrombophilia predisposing to VTE.
Venous Thromboembolism - Leg Clot Alert
- Deep Vein Thrombosis (DVT): Common, serious VTE manifestation.
- Clinical Signs: Unilateral leg swelling, pain, warmth, erythema. (Homan's sign: low sensitivity/specificity).
- Wells Score: Stratifies DVT risk (Low/Mod/High). Key factors include: cancer, paralysis, recent surgery/immobilization, tenderness, leg swelling, edema.
- Score ≥2: DVT likely.
- Score <2: DVT unlikely.
- Diagnosis:
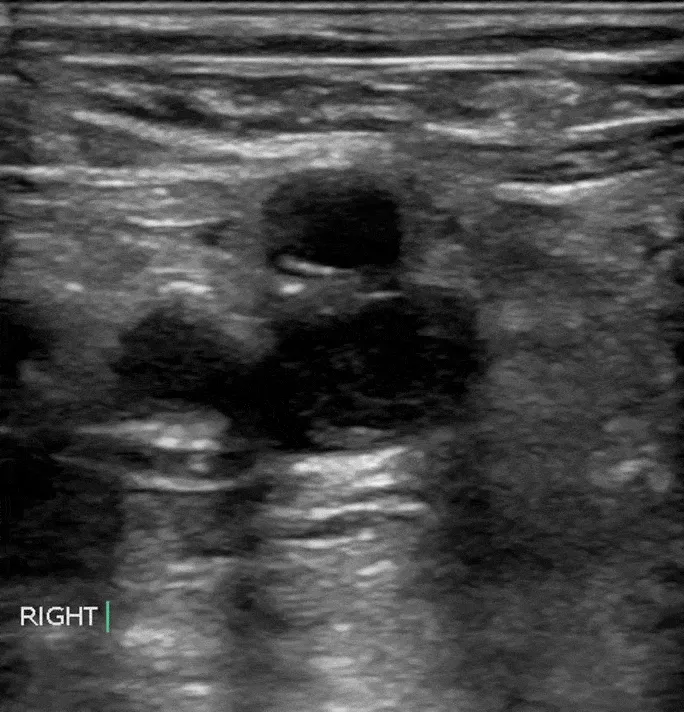
- Compression Ultrasonography (CUS): Gold standard. Non-compressible vein = DVT.
- D-dimer: High NPV; useful to exclude DVT in low probability cases.
⭐ Paradoxical Embolism: DVT can cause stroke via patent foramen ovale (PFO).
Venous Thromboembolism - Lung Clot Crisis
Pulmonary Embolism (PE): Lung artery obstruction, often from DVT. Symptoms: Sudden dyspnea, pleuritic pain, tachypnea, tachycardia. Massive PE: hypotension (SBP < 90 mmHg), syncope. Diagnosis: - Wells/Geneva Score: Pre-test probability. - D-dimer: Rules out PE if low probability. - CTPA: Gold standard imaging. - V/Q Scan: If CTPA C/I. - ECG: S1Q3T3 (classic), sinus tachycardia. Management: - Anticoagulation: LMWH, UFH, DOACs. - Thrombolysis/Embolectomy: For massive PE (hemodynamic instability). - IVC Filter: Recurrent PE or anticoagulation C/I.
⭐ Westermark sign (oligemia) & Hampton's hump (pleural-based infarct) are classic but rare CXR findings in PE.

Venous Thromboembolism - Clot Busters & Blockers
-
Primary Goals: Prevent clot propagation, embolization (PE), recurrence; restore flow.
-
Therapeutic Pillars: Anticoagulation (blockers), Thrombolysis (busters).
-
Anticoagulants (Clot Blockers):
- Initial: LMWH (Enoxaparin 1 mg/kg BID), UFH, Fondaparinux.
- Long-term: DOACs (Apixaban, Rivaroxaban) strongly preferred.
- Warfarin: Target INR 2.0-3.0; requires bridging & monitoring. 📌 Mnemonic: WEPT (Warfarin Extrinsic PT).
-
Thrombolytics (Clot Busters):
- Indications: Massive PE (SBP <90 mmHg, persistent instability), extensive limb-threatening DVT (phlegmasia).
- Agents: Alteplase (tPA). Catheter-directed thrombolysis (CDT) for selected cases.
-
IVC Filters:
- Reserved for: Absolute contraindication to anticoagulation; recurrent PE despite adequate anticoagulation.
⭐ DOACs are first-line long-term for most VTE over Warfarin: superior safety/efficacy, no INR checks. Exceptions: Antiphospholipid syndrome, severe renal failure.
Venous Thromboembolism - Guarding the Gates
- Prophylaxis: Mechanical (GCS, IPC); Pharmacological (LMWH, UFH).
- Pregnancy:
- LMWH preferred throughout & 6 weeks postpartum.
- Warfarin contraindicated (teratogenic).
- Cancer-Associated Thrombosis (CAT):
- LMWH or DOACs for long-term treatment.
- Long-term: Duration individualized; DOACs often used.
⭐ LMWH is the anticoagulant of choice for VTE in pregnant patients.
High‑Yield Points - ⚡ Biggest Takeaways
- Virchow's triad (stasis, hypercoagulability, endothelial injury) is key to VTE pathogenesis.
- Wells score and D-dimer are crucial for DVT/PE diagnosis and risk stratification.
- Pulmonary Embolism (PE) is a life-threatening complication of DVT.
- Anticoagulation (LMWH, UFH, DOACs) is the mainstay of VTE treatment.
- IVC filters are indicated for recurrent VTE despite anticoagulation or when anticoagulation is contraindicated.
- Post-thrombotic syndrome (PTS) is a common long-term complication of DVT.
- Massive PE may require thrombolysis or embolectomy; Saddle embolus is a classic example of massive PE affecting the pulmonary artery bifurcation.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more