PAD Basics - Plaque Attack Primer
- Definition: Peripheral Arterial Disease (PAD) signifies atherosclerotic obstruction of arteries supplying the extremities, predominantly lower limbs. Leads to ↓ tissue perfusion.
- Pathophysiology: Progressive atherosclerotic plaque accumulation within arterial walls → luminal stenosis/occlusion → impaired blood flow → distal ischemia.
- Major Risk Factors:
- Cigarette Smoking (paramount; dose-response relationship)
- Diabetes Mellitus (accelerated atherogenesis, neuropathy)
- Hypertension (endothelial injury)
- Hyperlipidemia (↑LDL, ↓HDL cholesterol)
- Advancing Age (>40 years, prevalence ↑ significantly >65)
- Male Sex
- Family History (premature CAD/PAD)
- Chronic Kidney Disease

⭐ The superficial femoral artery (SFA) passing through the adductor (Hunter's) canal is the most common segment affected by significant stenosis in PAD.
Symptoms & Signs - Leg's Distress Signals
- Intermittent Claudication (IC):
- Most common: exertional muscle pain (calf, thigh, buttock).
- Relieved by rest (minutes); reproducible distance.
- Rest Pain:
- Severe PAD: burning pain in forefoot/toes at rest, worse at night.
- Relieved by dependency. Ominous sign.
- Critical Limb Ischemia (CLI):
- Rest pain OR tissue loss (ulcers, gangrene).
- Ankle Pressure < 50 mmHg; Toe Pressure < 30 mmHg.
- Physical Signs:
- Skin: Pale, shiny, hairless, cool. Dependent rubor, pallor on elevation.
- Pulses: ↓/absent distal pulses.
- Capillary Refill: > 2 sec.
- Ulcers: Painful, "punched-out" (toes, malleoli).
- Gangrene.
- Buerger's angle < 20°: severe ischemia.
⭐ Leriche Syndrome (Aortoiliac occlusive disease): Triad of buttock/thigh claudication, absent/diminished femoral pulses, and impotence in males.
Diagnosis & Staging - Sizing Up Ischemia
- Initial Non-Invasive Tests:
- Ankle-Brachial Index (ABI): Key.
- Normal: 1.0-1.4
- Mild PAD: 0.71-0.90
- Moderate PAD: 0.41-0.70
- Severe PAD/CLI: ≤0.40
- Non-compressible: >1.4 (use TBI)
- Toe-Brachial Index (TBI): Use if ABI >1.4; TBI <0.7 diagnostic.
- Duplex Ultrasound (DUS): Localizes stenosis; PSVR >2.0 for >50% stenosis.
- Exercise ABI: Unmasks PAD if resting ABI normal; >20% drop positive.
- Ankle-Brachial Index (ABI): Key.
- Advanced Imaging (Pre-intervention):
- CTA, MRA, DSA (gold standard).
- Clinical Staging Systems:
- Fontaine:
- I: Asymptomatic
- IIa: Mild claudication
- IIb: Mod/Sev claudication
- III: Rest pain
- IV: Ulcer/gangrene
- Rutherford: (Cat. 0-6) Detailed, objective.
- Fontaine:
⭐ ABI ≤0.90 diagnoses PAD. If ABI >1.4 (calcification), TBI <0.7 is more reliable (e.g., diabetes, ESRD).

Management Spectrum - Revascularization Roadmap
- Indications for Revascularization:
- Lifestyle-limiting claudication (Rutherford 2-3)
- Critical Limb Ischemia (CLI):
- Rest pain (Rutherford 4)
- Tissue loss (ulcer/gangrene) (Rutherford 5-6)
- Primary Goals: Symptom relief, limb salvage, improved Quality of Life (QoL).
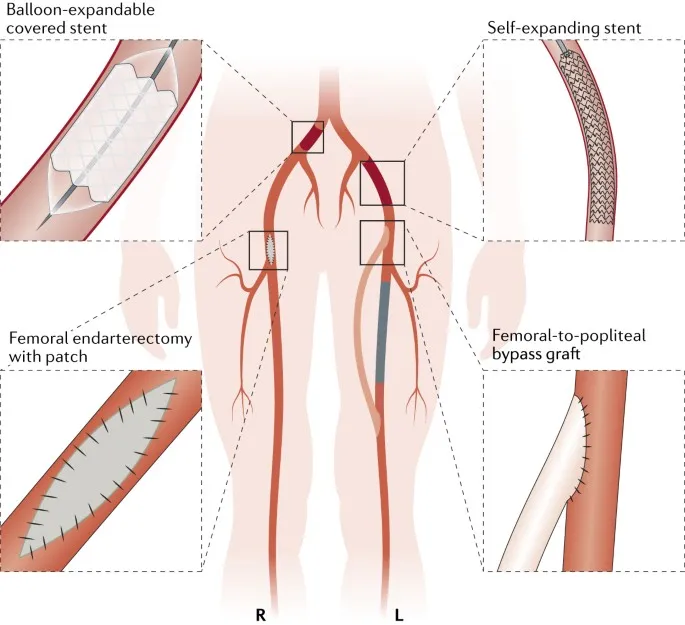
- Modalities & Strategy (TASC II Guided):
- Endovascular Therapy (EVT): Preferred for TASC A & B.
- Percutaneous Transluminal Angioplasty (PTA) ± Stenting (BMS/DES)
- Atherectomy (adjunctive)
- Surgical Bypass: For TASC C & D, long occlusions, failed EVT.
- Vein grafts (Great Saphenous Vein - GSV) > prosthetic.
- Common: Aortobifemoral, Femoropopliteal, Femorodistal.
- Hybrid Procedures: Combined EVT + open surgery.
- Endovascular Therapy (EVT): Preferred for TASC A & B.
- Post-Revascularization: Dual antiplatelet therapy (DAPT), statins, strict risk factor control.
⭐ CLI revascularization goal: Restore direct inline flow to ≥1 foot artery (angiosome concept) for optimal wound healing & limb salvage.
High‑Yield Points - ⚡ Biggest Takeaways
- Atherosclerosis is the most common cause of Peripheral Arterial Disease (PAD).
- Intermittent claudication (leg pain on exertion, relieved by rest) is the hallmark symptom.
- An Ankle-Brachial Index (ABI) < 0.9 is diagnostic for PAD.
- Critical Limb Ischemia (CLI) presents with rest pain, ischemic ulcers, or gangrene.
- Cilostazol is a key pharmacotherapy for symptomatic claudication.
- Smoking cessation is the single most important modifiable risk factor and intervention.
- Buerger's disease (thromboangiitis obliterans) is a non-atherosclerotic inflammatory disease strongly associated with young male smokers and a key differential diagnosis for PAD-like symptoms in this demographic.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

