Endovascular Basics & Access - Gateway to Vessels
Endovascular: Minimally invasive procedures within vessels.
-
Advantages: ↓morbidity, ↓hospital stay, ↓pain; local anesthesia.
-
Disadvantages: Radiation, contrast, restenosis, cost, technical skill.
-
Patient Selection: Comorbidities, vascular anatomy.
-
Access Sites:
- Common Femoral Artery (CFA): Preferred; antegrade/retrograde.
- 📌 Seldinger Technique: 1. Needle → 2. Wire → 3. Needle out → 4. Sheath/catheter.
- Alternatives: Brachial, radial, popliteal.
- Common Femoral Artery (CFA): Preferred; antegrade/retrograde.
-
Basic Tools:
- Needles (Seldinger); Guidewires (0.035", 0.018", 0.014"; J-tip, angled, hydrophilic, stiff); Catheters (diagnostic e.g. pigtail, guiding); Sheaths (introducer, French).
-
Imaging:
- Fluoroscopy (C-arm), DSA, roadmapping. IVUS/OCT for detail.
⭐ Seldinger technique: cornerstone for percutaneous arterial access.
PTA & Stenting - Pipe Perfectors
- Percutaneous Transluminal Angioplasty (PTA):
- Mechanism: Plaque fracture, vessel stretching, controlled dissection.
- Indications: Focal stenosis/occlusion (PVD, renal artery stenosis).
- Balloons: Compliant (sizing), Non-compliant (high-pressure for resistant lesions).
- Stents:
- Indications: Post-PTA (flow-limiting dissection, elastic recoil), restenosis prevention.
- Types:
Stent Type Key Feature / Drug (DES) Primary Uses Balloon-Expandable High radial force, precise Renal, iliac a. Self-Expanding Flexible, conformable SFA, carotid a. BMS Mechanical scaffold General use DES Drugs (Sirolimus/Paclitaxel); ↓neointimal hyperplasia Coronary, PVD (high restenosis risk) Covered (Stent-Graft) PTFE-lined; seals Aneurysms, perforations, AVFs
- Antiplatelet Therapy:
- DAPT: Aspirin + Clopidogrel (or Ticagrelor/Prasugrel). Duration varies by stent/location.
⭐ Drug-eluting stents significantly reduce in-stent restenosis rates compared to bare-metal stents, particularly in smaller vessels or diabetic patients.
Specialized Tools & Aneurysm Repair - Advanced Arsenal
-
Atherectomy Devices: Plaque debulking/removal.
- Types: Directional, rotational, orbital, laser.
- Indications: Calcified/ostial lesions, PTA/stenting alternative.
-
Thrombectomy/Embolectomy Devices: For thrombus/embolus removal.
- Types: Aspiration, mechanical fragmentation, rheolytic.
- Indications: Acute limb ischemia, DVT, PE.
-
Endovascular Aneurysm Repair (EVAR): For Abdominal Aortic Aneurysm (AAA).
- Device: Stent-graft.
- Indications: Diameter >5.5cm, symptomatic, rapid expansion.
- Key Anatomy: Adequate neck length/angulation, access vessel diameter.
-
Thoracic Endovascular Aortic Repair (TEVAR): For thoracic aortic aneurysms/dissections. Device: Stent-graft.
-
Endoleaks: Persistent aneurysm sac perfusion outside graft.
- Types I-V (📌 "SEB-PT"):
- I: Seal zone (graft ends)
- II: Branch (retrograde flow, e.g., lumbar, IMA)
- III: Fabric tear / Junctional separation
- IV: Porosity (graft wall)
- V: Endotension (sac expansion, no visible leak)
- Types I-V (📌 "SEB-PT"):
⭐ Type II endoleak, from branch vessels (e.g., lumbar artery, IMA), is the most common type following EVAR and often managed conservatively initially.
Complications & Post-Procedure - Navigating Pitfalls
- Access Site:
- Hematoma, pseudoaneurysm (Doppler: to-and-fro flow; Rx: compression, thrombin inj.), AV fistula, dissection, thrombosis, infection.
- Systemic:
- Contrast-Induced Nephropathy (CIN): Risks: CKD, DM, dehydration, high contrast volume. Prevent: Hydration, low/iso-osmolar contrast, ↓contrast volume, N-acetylcysteine.
- Allergic reaction.
- Procedure-Related:
- Distal embolization ("trash foot"), vessel perforation/rupture, dissection, radiation injury.
- Stent-Related (Long-term):
- In-stent restenosis (neointimal hyperplasia), stent thrombosis (DAPT adherence crucial!), stent fracture, migration.
- Post-Procedure:
- Monitoring; surveillance imaging (Duplex USG, CT Angio for EVAR/TEVAR).
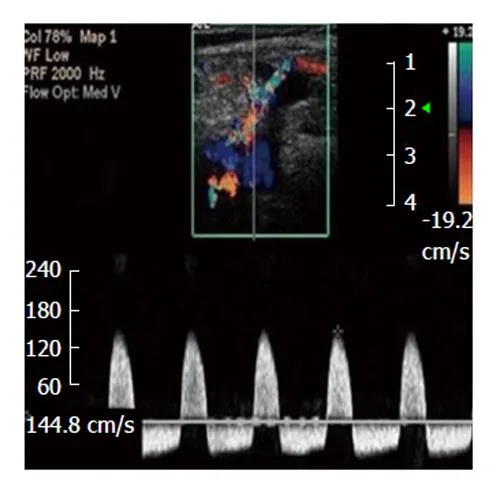
- Monitoring; surveillance imaging (Duplex USG, CT Angio for EVAR/TEVAR).
⭐ Acute stent thrombosis is a dreaded complication often linked to premature discontinuation of dual antiplatelet therapy (DAPT).
High‑Yield Points - ⚡ Biggest Takeaways
- Seldinger technique is fundamental for vascular access.
- Guidewires (hydrophilic, stiff) and catheters are core endovascular tools.
- Angioplasty (PTA) dilates stenoses; stents (BMS, DES) maintain vessel patency.
- EVAR/TEVAR is preferred for suitable aortic aneurysms over open repair.
- Complications: access site issues (hematoma, pseudoaneurysm), embolization, contrast nephropathy.
- Covered stents (stent-grafts) treat aneurysms, dissections, and perforations.
- Mechanical thrombectomy is vital for acute limb ischemia and stroke management.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

