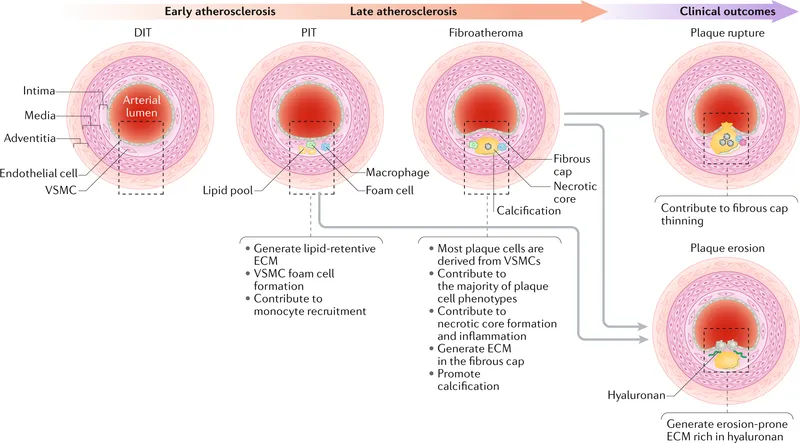
Pathophysiology & Risks - Genesis of Plaque
- Endothelial Injury/Dysfunction: Initial step. ↑Permeability, leukocyte adhesion. Triggers: HTN, smoking, hyperglycemia.
- Lipid Infiltration & Modification: LDL enters intima, undergoes oxidation (oxLDL).
⭐ Oxidized LDL is a key chemoattractant for macrophages in plaque formation.
- Inflammation & Foam Cell Formation:
- Monocytes → macrophages; engulf oxLDL → foam cells (fatty streaks).
- Plaque Maturation:
- Smooth muscle cell (SMC) migration, proliferation.
- SMCs synthesize ECM (collagen) → fibrous cap.
- Central necrotic core (lipids, debris) forms.
- Key Risk Factors:
- Non-Modifiable: Age, male, genetics.
- Modifiable: Dyslipidemia (↑LDL, ↓HDL), HTN (>130/80 mmHg), smoking, Diabetes (HbA1c >6.5%), obesity (BMI >30), ↑hs-CRP.
Clinical Manifestations - Arterial Distress Signals

| Arterial Bed | Clinical Manifestations |
|---|---|
| Coronary Artery Disease | Angina (stable/unstable), Myocardial Infarction (MI), Sudden Cardiac Death. |
| Carotid Artery Disease | Transient Ischemic Attack (TIA) - amaurosis fugax, focal weakness/sensory loss; Stroke (CVA). |
| Peripheral Arterial Disease (PAD) | Intermittent Claudication (calf, thigh, buttock), Rest Pain, Ulceration, Gangrene. 📌 6 P's of Acute Limb Ischemia: Pain, Pallor, Pulselessness, Paresthesia, Paralysis, Poikilothermia. Fontaine/Rutherford stages. |
| Renal Artery Stenosis | Refractory Hypertension, Flash Pulmonary Edema, Renal Failure. |
| Mesenteric Ischemia | Acute: Severe abdominal pain "out of proportion to exam", bloody diarrhea. Chronic: Postprandial pain ("intestinal angina"), weight loss, food fear. |
Diagnosis - Unmasking the Culprit
Key diagnostic steps include:
- Ankle-Brachial Index (ABI): Key non-invasive test. $ABI = \frac{Highest,Ankle,Systolic,Pressure}{Highest,Brachial,Systolic,Pressure}$
- Normal: 0.9-1.3
- PAD: <0.9 (Mild-Mod: 0.41-0.89, Severe: ≤0.4)
- Calcified vessels (e.g., in DM): >1.3
| Modality | Use | Pro(s) | Con(s) |
|---|---|---|---|
| ABI | Screen, severity | Non-invasive, cheap | Calcified vessels (DM) |
| DUS | Localize stenosis, f/u | No radiation/contrast, dynamic | Operator-dependent, view limits |
| CTA | Pre-op plan | Fast, good resolution | Radiation, contrast risks |
| MRA | CTA C/I (allergy, renal) | No radiation | Costly, implants, NSF risk |
| DSA | Gold standard, intervention | Max accuracy, therapeutic | Invasive, risks (contrast/rad) |
| %%{init: {'flowchart': {'htmlLabels': true}}}%% | |||
| flowchart TD |
Start["🩺 Suspected PAD
• Arterial disease• Leg pain symptoms"]
Assess["📋 Clinical Eval
• History and Exam• Pulse palpation"]
ABI["🔬 Initial ABI
• Brachial index• Doppler pressure"]
DUS["🔬 Duplex US
• Localize lesion• Assess severity"]
Exer["🔬 Exercise/TBI
• Post-stress ABI• Toe Brachial Index"]
CTAMRA["💊 CTA or MRA
• Pre-intervention• Vascular mapping"]
Start --> Assess Assess --> ABI ABI -->|ABI < 0.9| DUS ABI -->|Normal+Symptom| Exer DUS --> CTAMRA
style Start fill:#F7F5FD, stroke:#F0EDFA, stroke-width:1.5px, rx:12, ry:12, color:#6B21A8 style Assess fill:#FEF8EC, stroke:#FBECCA, stroke-width:1.5px, rx:12, ry:12, color:#854D0E style ABI fill:#FFF7ED, stroke:#FFEED5, stroke-width:1.5px, rx:12, ry:12, color:#C2410C style DUS fill:#FFF7ED, stroke:#FFEED5, stroke-width:1.5px, rx:12, ry:12, color:#C2410C style Exer fill:#FFF7ED, stroke:#FFEED5, stroke-width:1.5px, rx:12, ry:12, color:#C2410C style CTAMRA fill:#F1FCF5, stroke:#BEF4D8, stroke-width:1.5px, rx:12, ry:12, color:#166534
> ⭐ Digital Subtraction Angiography (DSA) remains the gold standard for arterial imaging but is invasive.
## Management Approaches - Revascularization Roadmap
* **Baseline**: Optimal Medical Therapy (OMT) - Aspirin **75-325mg** / Clopidogrel **75mg**, Statins (LDL <**70mg/dL**), BP/DM control.
* **Peripheral Arterial Disease (PAD)**:
- Intermittent Claudication:
+ Conservative: Exercise, Cilostazol **100mg** BID (📌 CI: Heart Failure).
+ Revascularization (Endovascular/Surgical) if lifestyle-limiting.
- Critical Limb Ischemia (CLI): Urgent Revascularization!
```mermaid
%%{init: {'flowchart': {'htmlLabels': true}}}%%
flowchart TD
Start["<b>⚠️ Critical Ischemia</b><br><span style='display:block; text-align:left; color:#555'>• Rest pain/ulcers</span><span style='display:block; text-align:left; color:#555'>• Gangrene symptoms</span>"]
Assess["<b>📋 Patient Assessment</b><br><span style='display:block; text-align:left; color:#555'>• Lesion evaluation</span><span style='display:block; text-align:left; color:#555'>• Risk stratification</span>"]
Optimize["<b>💊 Optimize Therapy</b><br><span style='display:block; text-align:left; color:#555'>• Medical management</span><span style='display:block; text-align:left; color:#555'>• Risk reduction</span>"]
Revasc["<b>📋 Revascularization</b><br><span style='display:block; text-align:left; color:#555'>• Endo vs Surgical</span><span style='display:block; text-align:left; color:#555'>• Plan strategy</span>"]
Angio["<b>💊 Angioplasty +/- Stent</b><br><span style='display:block; text-align:left; color:#555'>• Minimal invasive</span><span style='display:block; text-align:left; color:#555'>• Endo preference</span>"]
Success1["<b>📋 Success?</b><br><span style='display:block; text-align:left; color:#555'>• Evaluate flow</span><span style='display:block; text-align:left; color:#555'>• Clinical response</span>"]
Bypass["<b>💊 Surgical Bypass</b><br><span style='display:block; text-align:left; color:#555'>• e.g. Fem-Pop</span><span style='display:block; text-align:left; color:#555'>• Open procedure</span>"]
Success2["<b>📋 Success?</b><br><span style='display:block; text-align:left; color:#555'>• Graft patency</span><span style='display:block; text-align:left; color:#555'>• Wound healing</span>"]
Follow["<b>👁️ Follow-up + OMT</b><br><span style='display:block; text-align:left; color:#555'>• Regular monitoring</span><span style='display:block; text-align:left; color:#555'>• Continue therapy</span>"]
Amputate["<b>⚠️ Palliative Care</b><br><span style='display:block; text-align:left; color:#555'>• Consider amputation</span><span style='display:block; text-align:left; color:#555'>• Comfort measures</span>"]
Start --> Assess
Assess --> Optimize
Optimize --> Revasc
Revasc -->|Endo First| Angio
Revasc -->|Complex/Failed| Bypass
Angio --> Success1
Success1 -->|Yes| Follow
Success1 -->|No| Bypass
Bypass --> Success2
Success2 -->|Yes| Follow
Success2 -->|No| Amputate
style Start fill:#FDF4F3, stroke:#FCE6E4, stroke-width:1.5px, rx:12, ry:12, color:#B91C1C
style Assess fill:#FEF8EC, stroke:#FBECCA, stroke-width:1.5px, rx:12, ry:12, color:#854D0E
style Optimize fill:#F1FCF5, stroke:#BEF4D8, stroke-width:1.5px, rx:12, ry:12, color:#166534
style Revasc fill:#FEF8EC, stroke:#FBECCA, stroke-width:1.5px, rx:12, ry:12, color:#854D0E
style Angio fill:#F1FCF5, stroke:#BEF4D8, stroke-width:1.5px, rx:12, ry:12, color:#166534
style Success1 fill:#FEF8EC, stroke:#FBECCA, stroke-width:1.5px, rx:12, ry:12, color:#854D0E
style Bypass fill:#F1FCF5, stroke:#BEF4D8, stroke-width:1.5px, rx:12, ry:12, color:#166534
style Success2 fill:#FEF8EC, stroke:#FBECCA, stroke-width:1.5px, rx:12, ry:12, color:#854D0E
style Follow fill:#EEFAFF, stroke:#DAF3FF, stroke-width:1.5px, rx:12, ry:12, color:#0369A1
style Amputate fill:#FDF4F3, stroke:#FCE6E4, stroke-width:1.5px, rx:12, ry:12, color:#B91C1C
- Carotid Artery Stenosis:
- Symptomatic (TIA/Stroke): Carotid Endarterectomy (CEA) for stenosis >70% (NASCET) or >50% (ECST). Carotid Artery Stenting (CAS) for high surgical risk.
- Asymptomatic: OMT. Consider CEA/CAS if stenosis >60-70% & low peri-operative risk (<3%).

⭐ Cilostazol, a phosphodiesterase III inhibitor, is used for intermittent claudication; it has antiplatelet and vasodilatory effects. Avoid in heart failure.
High‑Yield Points - ⚡ Biggest Takeaways
- Atherosclerosis is a systemic disease; affects multiple arterial beds.
- Key risk factors: smoking, diabetes, hypertension, hyperlipidemia.
- Common sites: abdominal aorta, coronaries, carotids, femoro-popliteal segment.
- Ankle-Brachial Index (ABI) <0.9 diagnoses Peripheral Arterial Disease (PAD); <0.4 indicates Critical Limb Ischemia (CLI).
- CLI (rest pain, ulcer, gangrene) needs urgent revascularization.
- Management: risk factor control, antiplatelets (aspirin, clopidogrel), statins, revascularization.
- Symptomatic carotid stenosis >50-70% often requires carotid endarterectomy (CEA) to prevent stroke.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

