Intro & Classification - Aorta's Big Bulge
- Aortic Aneurysm: Permanent localized dilatation of aorta; diameter > 1.5x normal expected diameter.
- Normal aorta: Thoracic ≈ 3 cm, Abdominal ≈ 2 cm.
- Classification by Location:
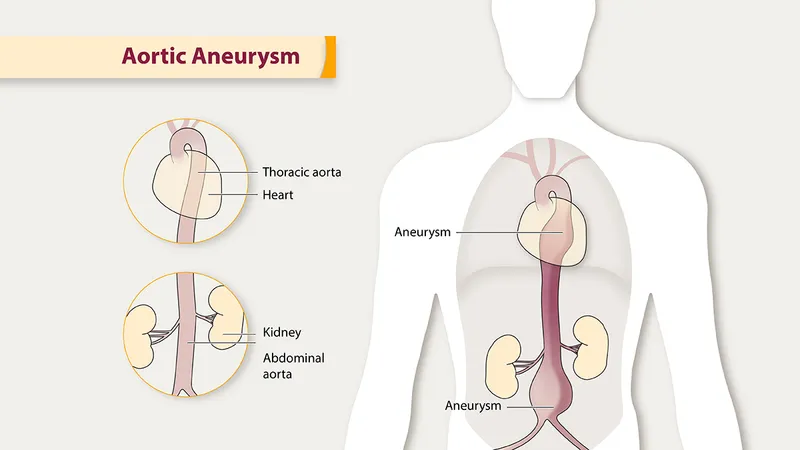
- Abdominal Aortic Aneurysm (AAA): Most common, typically infrarenal.
- Thoracic Aortic Aneurysm (TAA).
- Classification by Morphology:
- Fusiform: Symmetrical, spindle-shaped (common).
- Saccular: Asymmetrical, berry-like outpouching.
- Wall Involvement:
- True Aneurysm: Involves all three layers (intima, media, adventitia).
- Pseudoaneurysm (False): Contained rupture; wall not all 3 layers.
⭐ Majority (≈90%) of AAAs are infrarenal.

Etiology & Risks - Weak Wall Woes
- Primary: Atherosclerotic degeneration (most common).
- Wall weakening: Elastin/collagen breakdown in media.
- Enzymatic degradation: ↑ Matrix Metalloproteinases (MMPs).
- Inflammation & oxidative stress contribute.
- Key Risk Factors:
- Advanced age (>60-65 years).
- Male sex (M:F ≈ 4:1).
- 📌 Smoking: Strongest modifiable risk; dose-dependent.
- Hypertension.
- Family history of AAA.
- Hyperlipidemia.
- Genetic Links:
- Marfan (FBN1), Ehlers-Danlos Type IV (COL3A1), Loeys-Dietz (TGFBR1/2).
- Less Common:
- Infections (mycotic aneurysms).
- Vasculitis (e.g., Takayasu).
- Trauma.
⭐ Smokers have up to 5x increased risk of developing AAA and faster expansion.
Clinical Features - Silent Threats Scream
- Often asymptomatic, discovered incidentally.
- Thoracic Aortic Aneurysm (TAA):
- Chest/back pain (most common).
- Dyspnea, cough, hoarseness (recurrent laryngeal nerve).
- Dysphagia (esophageal compression).
- Superior Vena Cava (SVC) syndrome.
- Abdominal Aortic Aneurysm (AAA):
- Most are asymptomatic until rupture.
- Pulsatile abdominal mass (often found on routine exam).
- Abdominal or back pain (constant, gnawing; suggests expansion/impending rupture).
- Limb ischemia (embolic phenomena).
- Rupture Triad (AAA):
- Sudden severe pain (abdominal/back/flank).
- Hypotension.
- Pulsatile abdominal mass.
⭐ Most AAAs are infrarenal. Rupture into the retroperitoneum is more common than free intraperitoneal rupture, leading to a contained hematoma initially before potential free rupture and rapid exsanguination. 📌 RUPTURE = Renal colic-like pain, Unstable vitals, Pulsatile mass, Tender abdomen, Urge to defecate, Radiating pain to back/groin, Ecchymosis (Grey Turner's/Cullen's sign - late).
Diagnosis & Screening - Spotting the Swell
- Clinical: Often asymptomatic. Pulsatile abdominal mass.
- Imaging:
- Ultrasound (USG): Primary for diagnosis & screening; measures diameter accurately.
- CT Angiography (CTA): Gold standard for pre-operative planning; details anatomy, extent, vessel involvement.
- MRA: CTA alternative (e.g., renal issues, contrast allergy).
- AXR: Incidental finding (calcified aortic outline).
- Screening (USPSTF):
⭐ AAA Definition: Focal aortic dilation ≥ 3.0 cm OR > 1.5 times normal diameter (normal aorta ≈ 2.0 cm).

Management - Repair & Rescue
- Indications for Repair (AAA):
- Symptomatic (pain, embolism)
- Diameter >5.5 cm (men), >5.0 cm (women)
- Rapid expansion: >0.5 cm in 6 months or >1 cm/year
- Complications: dissection, pseudoaneurysm
- Repair Options:
- Endovascular Aneurysm Repair (EVAR): Preferred for suitable anatomy; lower perioperative mortality.
- Open Surgical Repair: For complex anatomy, younger patients, connective tissue disorders.
- Ruptured AAA (Rescue):
- Emergency surgery (EVAR or open)
- Permissive hypotension (SBP 70-90 mmHg) until aortic control.
- ABCDE, IV access, cross-match blood.
⭐ Post-EVAR, endoleaks are a common complication requiring surveillance and potential re-intervention. Type II endoleak (branch vessel backflow) is the most frequent.
High‑Yield Points - ⚡ Biggest Takeaways
- Abdominal Aortic Aneurysms (AAA) are most common, typically infrarenal.
- Atherosclerosis is the primary cause; smoking is a major risk factor.
- Often asymptomatic; rupture triad: pain, hypotension, pulsatile mass.
- Ultrasound for screening (men 65-75 with smoking history) & surveillance.
- CT angiography for pre-operative planning.
- Repair (open or EVAR) if diameter > 5.5 cm, rapidly expanding, or symptomatic.
- Law of Laplace links size to ↑rupture risk.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

