Kidneys - Bean Brilliance
- General: Retroperitoneal. Wt: ~150g. Size: ~11x6x3 cm. Loc: T12-L3 (R lower).
- Coverings (Inner→Outer): Fibrous capsule, perirenal fat, renal fascia (Gerota's), pararenal fat.
- Hilum (Ant→Post): 📌 VAU - Vein, Artery, Ureter/Pelvis.
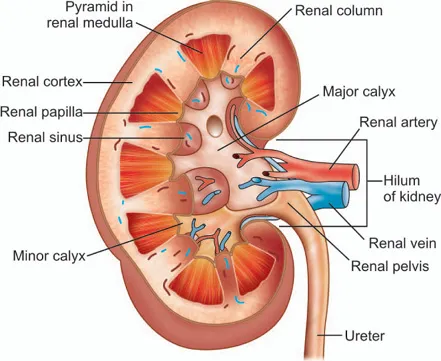 , relations)
, relations) - Relations:
Aspect Right Kidney Left Kidney Anterior Liver, duodenum, hepatic flexure, jejunum Stomach, spleen, pancreas tail, splenic flexure, jejunum Posterior Diaphragm, 12th rib, psoas, QL, trans. abdominis Diaphragm, 11th & 12th ribs, psoas, QL, trans. abdominis - Arterial Supply: Renal art. (aorta) → segmental → lobar → interlobar → arcuate → interlobular → afferent arteriole.
- Venous Drainage: Parallels arteries → renal vein → IVC.
⭐ Left renal vein longer; receives L. suprarenal & L. gonadal veins.
- Lymphatics: Para-aortic nodes.
- Innervation: Renal plexus (symp. T10-L1; parasymp. vagus).
Ureters - Pathway Pipes
- Retroperitoneal tubes, ~25-30 cm long.
- Course:
- Abdominal: Descends on psoas major.
- Pelvic: Crosses pelvic brim/iliac vessels.
- Three Constrictions (Sites of calculus impaction):
-
- Pelvi-ureteric junction (PUJ)
-
- Crossing pelvic brim/iliac vessels
-
- Vesico-ureteric junction (VUJ)
-
- Blood Supply (Segmental): From renal, gonadal, aorta, common iliac, & internal iliac arteries.
- Histology: Transitional epithelium (urothelium).
- Relations: 📌 'Water under the bridge':
- Females: Ureter passes under uterine artery.
- Males: Ureter passes under vas deferens.
⭐ The narrowest point of the ureter is the vesico-ureteric junction (VUJ), a common site for calculus impaction.
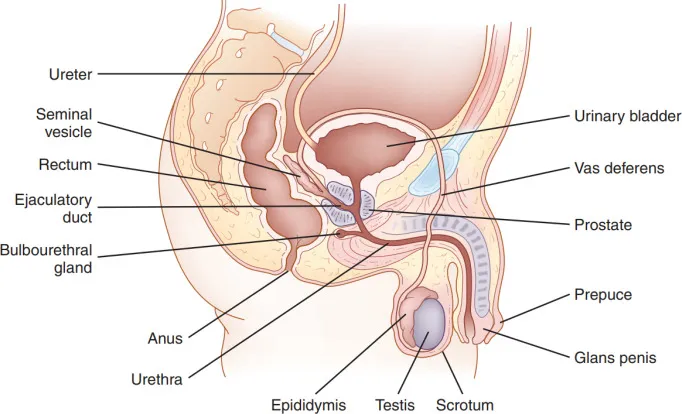
Bladder & Urethra - Reservoir & Release
- Bladder:
- Location: Pelvic cavity; retroperitoneal. Apex ant., Base post., Neck inf.
- Relations: ♂ Ant. to rectum, sup. to prostate. ♀ Ant. to uterus & vagina.
- Trigone: At base; ureteric orifices & int. urethral meatus.
- Detrusor muscle: Smooth muscle wall. Normal capacity: 300-500ml.
- Innervation & Micturition:
- Urethra:
- Female Urethra: ~4cm; ext. meatus in vestibule.
- Male Urethra: ~20cm. 📌 Mnemonic (Parts): 'Prostitutes Make Me Beg Pardon' (Prostatic, Membranous, Bulbar, Penile/Spongy).
- Prostatic (~3cm): Widest.
- Membranous (~1-2cm): Narrowest, passes UG diaphragm.
- Bulbar (~1-2cm): In bulb of penis.
- Penile/Spongy (~15cm): Longest, in corpus spongiosum.
- Sphincters: Int. (smooth, involuntary), Ext. (skeletal, voluntary, pudendal n.).
⭐ The membranous urethra is the shortest, least dilatable part, and most prone to injury in pelvic fractures.
Prostate & Testes - Glandular Guards
Prostate:
- Location: Inferior to bladder, surrounds prostatic urethra; ~20g.
- Zones & Significance:
- Peripheral (PZ): 70%; most CaP.
- Central (CZ): 25%.
- Transitional (TZ): 5%; BPH.
- Anterior fibromuscular stroma.
- Ejaculatory ducts: Pass posterior, open into prostatic urethra.

Testes:
- Location: Scrotum.
- Coverings: 📌 'Some Damn Englishman Called It The Testis'; Skin, Dartos, External spermatic fascia, Cremasteric fascia, Internal spermatic fascia, Tunica vaginalis, Tunica albuginea.
- Blood Supply:
- Testicular artery: from aorta (L2).
- Pampiniform plexus: thermoregulation, forms testicular vein.
- Lymphatics: Para-aortic nodes.
- Vas deferens: epididymis to ejaculatory duct.
⭐ Most CaP (~70-80%) in peripheral zone, DRE detectable.
High‑Yield Points - ⚡ Biggest Takeaways
- Kidneys: Retroperitoneal, T12-L3. Segmental arteries are end arteries, infarction risk.
- Ureteric constrictions: PUJ, pelvic brim, VUJ - common sites for stone impaction.
- Bladder trigone: Smooth, bounded by ureteric orifices and internal urethral meatus.
- Testicular drainage: Left vein to left renal vein, right to IVC. Lymphatics to paraaortic nodes.
- Male urethra: Prostatic (widest), membranous (narrowest, injury prone), spongy.
- Gerota's fascia encloses kidney/adrenal; Waldeyer's sheath at VUJ helps prevent reflux.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

