CAKUT & Antenatal Hydronephrosis - Kidney Quirks & Womb Woes
- CAKUT (Congenital Anomalies of Kidney & Urinary Tract): Spectrum of structural malformations.
- Common types: Ureteropelvic Junction Obstruction (UPJO), Vesicoureteral Reflux (VUR), Posterior Urethral Valves (PUV), Multicystic Dysplastic Kidney (MCDK).
- Antenatal Hydronephrosis (ANH): Dilation of fetal renal collecting system (pelvis AP diameter >4mm <28wks, >7mm ≥28wks).
- SFU Grading: Grades 1-4 assess severity.
- Causes: Transient (most common), UPJO, VUR, PUV, MCDK.
- Postnatal Evaluation: Ultrasound (USG) initial. Further: Voiding Cystourethrogram (VCUG), renal scan (DTPA/MAG3).
- Management: Observation, prophylactic antibiotics (VUR), or surgical correction for obstruction.
⭐ Most common cause of neonatal hydronephrosis is transient hydronephrosis, followed by UPJ obstruction.
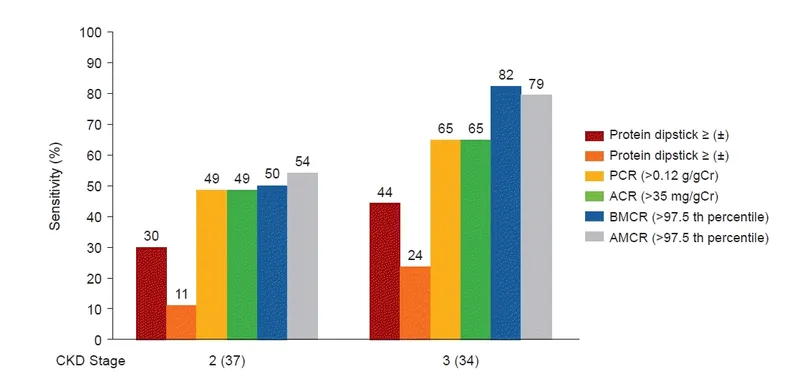
Postnatal ANH Management Flow:
Obstructive Uropathies - Plumbing Problems Pronto
-
Posterior Urethral Valves (PUV):
- Embryology: Wolffian duct remnant.
- Diagnosis: Antenatal USG ('keyhole' sign); postnatal VCUG (gold standard).
- Management: Endoscopic valve ablation.
⭐ Posterior Urethral Valves (PUV) are the most common cause of bladder outlet obstruction in male neonates.
-
Ureteropelvic Junction Obstruction (UPJO):
- Causes: Intrinsic (aperistaltic segment) or extrinsic (crossing vessels).
- Symptoms: Antenatal hydronephrosis, flank pain, UTI.
- Diagnosis: USG, diuretic renography (MAG3/DTPA). Surgery if symptomatic / DRF < 40%.
- Management: Anderson-Hynes pyeloplasty.
- Ureterovesical Junction Obstruction (UVJO):
- Types: Primary (congenital) or secondary.
- Leads to megaureter (ureter > 7mm).
- Management: Ureteral reimplantation if symptomatic or ↓ renal function.
VUR & Pediatric UTIs - Reflux Ruckus & Bug Battles
- VUR (Vesicoureteral Reflux): Retrograde urine flow (bladder → kidney).
- Primary: Congenital UVJ incompetence. Secondary: ↑ Bladder pressure (e.g., PUV).
- Grading: International Reflux Study I-V.
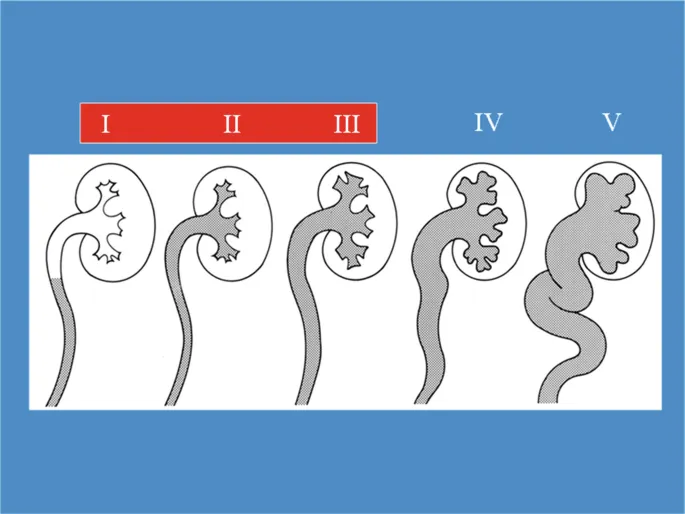
- Dx: Voiding Cystourethrogram (VCUG).
⭐ Voiding Cystourethrogram (VCUG) is the gold standard for diagnosing Vesicoureteral Reflux (VUR).
- Complications: Recurrent UTIs, renal scarring, HTN.
- VUR Management:
- Conservative: Continuous Antibiotic Prophylaxis (CAP) for Grades I-III / symptomatic.
- Surgical: Breakthrough UTIs on CAP, new/worsening scars, persistent high-grade (IV/V) >1-2 yrs. Options: Deflux, ureteric reimplantation.
- Flowchart:
- Pediatric UTIs:
- Risks: VUR, obstruction, female, uncircumcised males <1yr.
- Bugs: E. coli (most common), Klebsiella, Proteus.
- Dx: Urine culture. Tx: Antibiotics.
- Scarring: DMSA scan (4-6 months post-UTI). 📌 DMSA: Detects My Scarring Always.
Genital & Testicular Anomalies - Bits & Bobs Basics
- Hypospadias: Urethral meatus opens on ventral aspect of penis.
- Classification: Glandular, coronal, penile, scrotal.
- Associated: Chordee (ventral curvature), hooded prepuce (dorsal redundancy).
- Repair: Surgical correction at 6-18 months; aims for normal voiding & cosmesis.

- Epispadias: Urethral meatus on dorsal aspect of penis; often associated with bladder exstrophy.
- Undescended Testis (UDT)/Cryptorchidism: Failure of testis to descend into scrotum.
- Types: Palpable (approx. 80%), non-palpable (approx. 20%).
- Complications: ↓Fertility, ↑Malignancy risk (seminoma 4-10x higher).
- Management: Orchiopexy, ideally between 6-12 months of age.
> ⭐ The optimal timing for orchiopexy in Undescended Testis (UDT) is between **6 and 12 months** of age to maximize fertility potential and allow for early detection of malignancy.
- Testicular Torsion: Twisting of spermatic cord leading to vascular compromise; a urological emergency.
- Neonatal: Extravaginal; often presents as a firm, painless scrotal mass.
- Pubertal: Intravaginal; associated with 'bell clapper' deformity; acute onset of severe testicular pain.
- Management: Urgent surgical exploration, detorsion, and bilateral orchiopexy.
High‑Yield Points - ⚡ Biggest Takeaways
- PUV: Commonest male neonatal bladder outlet obstruction; "keyhole" sign USG.
- VUR: VCUG for diagnosis & grading; risk of renal scarring.
- Hypospadias: Ventral meatus, chordee; no circumcision pre-repair.
- Cryptorchidism: ↑ risk malignancy/infertility; orchiopexy by 6-18 months.
- Wilms' Tumor: Commonest pediatric renal cancer; painless abdominal mass.
- UPJ Obstruction: Commonest cause antenatal hydronephrosis; pyeloplasty.
- Testicular Torsion: Surgical emergency; absent cremasteric reflex; immediate detorsion.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

