Vascular Trauma - Bleeding Battleground
Damage to arteries or veins, often life/limb-threatening.
- Mechanisms:
- Penetrating: Gunshot wounds (GSW), stab wounds.
- Blunt: Fractures, dislocations, crush.
- Iatrogenic: Post-procedural.
- Hard Signs (➡️ OR):
- Pulsatile bleeding, expanding hematoma.
- Absent distal pulses, palpable thrill, audible bruit.
- Signs of acute limb ischemia (📌 6 P's: Pain, Pallor, Pulselessness, Paresthesia, Paralysis, Poikilothermia).
- Soft Signs (➡️ Investigate):
- Hx of arterial bleed, diminished pulses, injury near artery (fracture/dislocation), nerve deficit.
- Diagnosis: ABI <0.9, CT Angiography (CTA), Duplex USG.
- Management: ABCDEs, direct pressure, tourniquet. Definitive: Surgical (repair/bypass), Endovascular.
⭐ Most common mechanism of major vascular injury is penetrating trauma (e.g., GSW, stab wounds).
Diagnosis - Spot the Leak
- Clinical Evaluation: Assess for hard and soft signs of vascular injury.
Hard Signs (Immediate OR) 📌 "PULSE B H" Soft Signs (Further Investigation) Pulsatile bleeding Small, stable hematoma Unexplained shock/hypotension Associated nerve injury Large/expanding hematoma History of moderate hemorrhage (scene) Signs of ischemia (6 Ps) Proximity to major vessel / Penetrating injury path Audible Bruit Significant bony injury / Dislocation Palpable Thrill Diminished (but palpable) pulses History of hemorrhage (active/pulsatile) - Key Diagnostic Tools:
- Ankle-Brachial Index (ABI): $ABI = P_{ankle} / P_{brachial}$. ABI < 0.9 suggests arterial injury.
- Duplex Ultrasonography (DUS): Non-invasive, real-time, bedside assessment.
- CT Angiography (CTA): Preferred modality for hemodynamically stable patients.
- Conventional Angiography: Gold standard, especially if endovascular intervention is planned.
⭐ CT Angiography (CTA) is the diagnostic modality of choice for hemodynamically stable patients with suspected extremity vascular trauma.

Management - Stop the Flood
-
Pre-Hospital & ED Resuscitation:
- Direct pressure; tourniquet for severe limb bleed (note time). 📌 Convert <2h if possible.
- ABCDEs, O2, 2 large-bore IVs.
- Fluids: Crystalloids, then 1:1:1 blood products (PRBC:FFP:Platelets).
- Permissive Hypotension: SBP 80-90 mmHg (penetrating), <110 mmHg (blunt) until control (not for TBI).
- Reverse anticoagulants; give antibiotics, tetanus toxoid.
-
Hemorrhage Control & Repair Strategy:
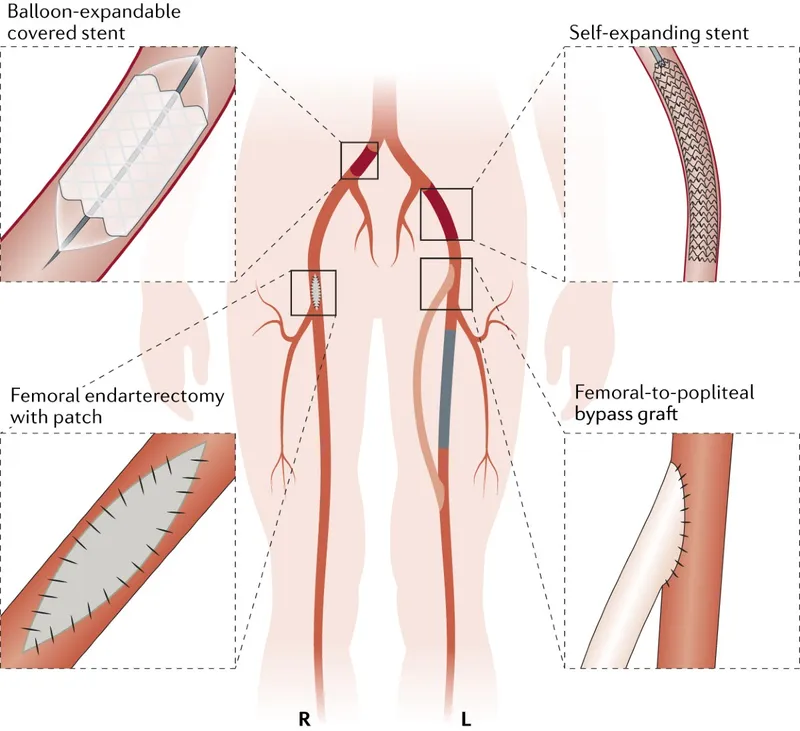
- Key Repair Principles & Adjuncts:
- Obtain proximal/distal control.
- Techniques: Primary suture, end-to-end anastomosis, vein graft (GSV preferred), ligation (damage control), endovascular (stents/embolization).
- Fasciotomy: For compartment syndrome risk (ischemia >4-6h, combined A+V injury, swelling).
⭐ Popliteal artery injury with knee dislocation: high amputation risk (30-50% if repair >8h delayed), needs urgent surgery.
Complications - Aftermath & Alerts
Error: Failed to generate content for this concept group.
High‑Yield Points - ⚡ Biggest Takeaways
- Hard signs of vascular injury (e.g., pulsatile bleed, expanding hematoma, absent pulse, thrill/bruit) mandate immediate surgical exploration.
- Soft signs (e.g., history of bleed, diminished pulse, proximity, nerve deficit) warrant further investigation, typically CTA or Doppler USG.
- An Ankle-Brachial Index (ABI) < 0.9 strongly indicates significant arterial injury.
- The superficial femoral artery is the most commonly injured peripheral vessel.
- Compartment syndrome is a critical, limb-threatening complication requiring prompt fasciotomy.
- Temporary vascular shunting is vital in damage control surgery for complex injuries.
- Ligation is a life-saving option for non-critical arteries or in exsanguinating patients during damage control resuscitation (DCR).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

