Burn Assessment - Sizing Up The Sizzle
- TBSA Estimation:
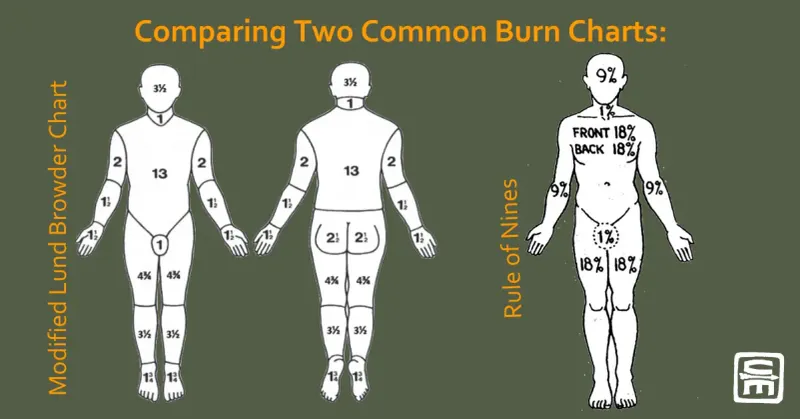
- Rule of Nines (Adults): Head/Neck 9%, Arm 9% (each), Trunk 18% (ant/post each), Leg 18% (each), Perineum 1%.
- Lund-Browder Chart: Most accurate for children.
⭐ Lund-Browder chart is the most accurate method for estimating TBSA in children.
- Palmer Method: Patient's palm ≈ 1% TBSA (scattered burns).
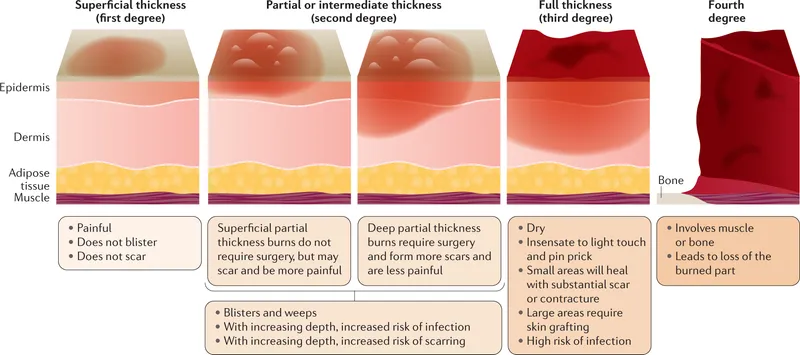
- Burn Depth:
- Superficial (1st°): Epidermis. Red, painful, no blisters. Heals 3-6d.
- Partial-thickness (2nd°):
- Superficial: Papillary dermis. Blisters, painful, blanches. Heals 7-21d.
- Deep: Reticular dermis. Mottled, ↓pain, ±blanching. Scarring. Heals >21d.
- Full-thickness (3rd°): All layers. Leathery, insensate, no blanching. Grafting.
- 4th°: To muscle/bone.
- Burn Severity Classification (ABA Criteria):
- Key Factors for Severity: Inhalation (soot, hoarseness, facial burns), circumferential, elec/chem, trauma, age (<5/>50 yrs).
Pathophysiology & Inhalation - Body's Inferno
- Systemic Effects: Burn → Systemic Inflammatory Response Syndrome (SIRS) (cytokines ↑).
- Cardiovascular: ↓CO, ↑capillary permeability → Burn shock.
- Metabolic: Hypermetabolism & catabolism.
- Immune: Immunosuppression → ↑infection risk.
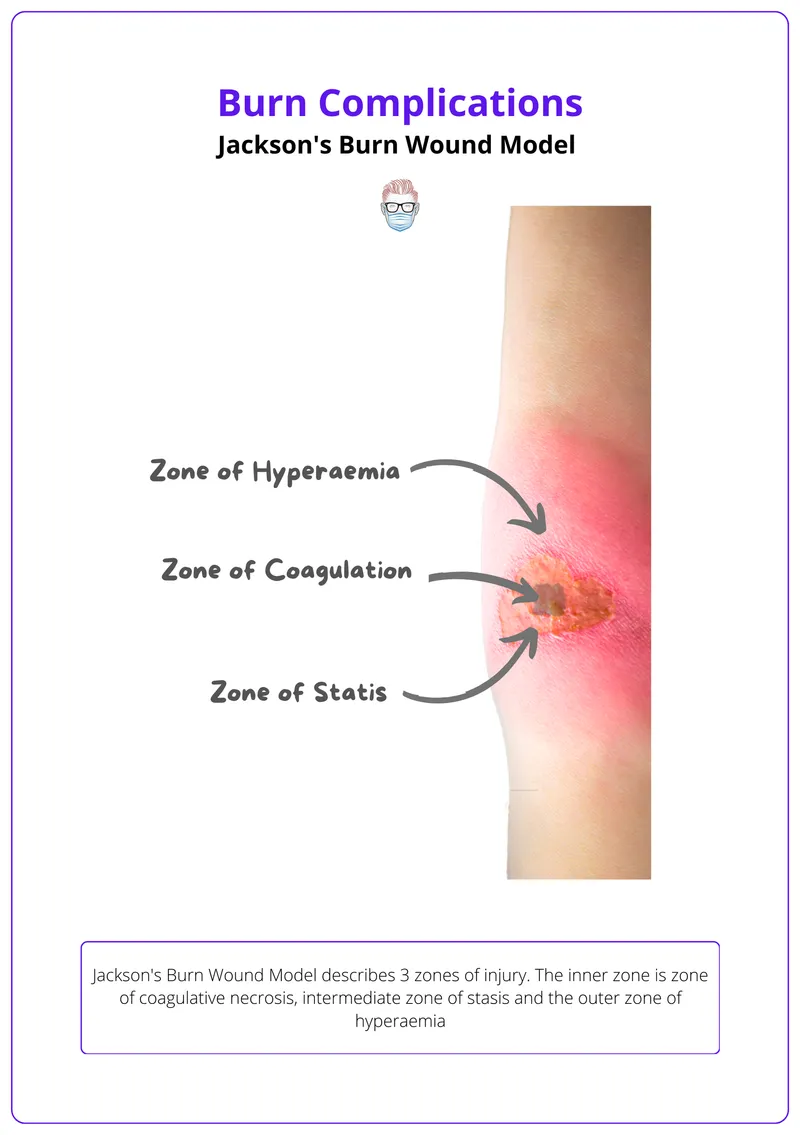
- Jackson's Zones of Injury: Coagulation (central, irreversible necrosis), Stasis (surrounding, potentially salvageable), Hyperemia (outer, vasodilation, recovers).
- Inhalation Injury: Major cause of mortality. Suspect with: facial burns, singed nasal hairs, soot in sputum/oropharynx, hoarseness, wheezing, history of enclosed space fire.
- Upper airway: Supraglottic edema → airway obstruction.
- Lower airway: Chemical tracheobronchitis, mucosal sloughing, ARDS.
- Systemic toxicity: Carbon Monoxide (CO), Cyanide (CN).
- 📌 Mnemonic (Signs of Inhalation Injury - BURNS): Blisters/burns to face/neck, Using accessory muscles, Rales/rhonchi/wheezing, Nasal hair singeing/soot, Stridor/hoarseness.
- Diagnosis & Management:
- Bronchoscopy: Gold standard for diagnosing lower airway injury.
- Early intubation if airway compromise suspected (e.g., stridor, respiratory distress, GCS <8).
- Administer 100% humidified O2.
⭐ Cherry-red skin colour in CO poisoning is a late and unreliable sign; always suspect CO poisoning with high carboxyhemoglobin (COHb) levels in patients from enclosed space fires, even with normal pulse oximetry.
Acute Management - Dousing The Flames
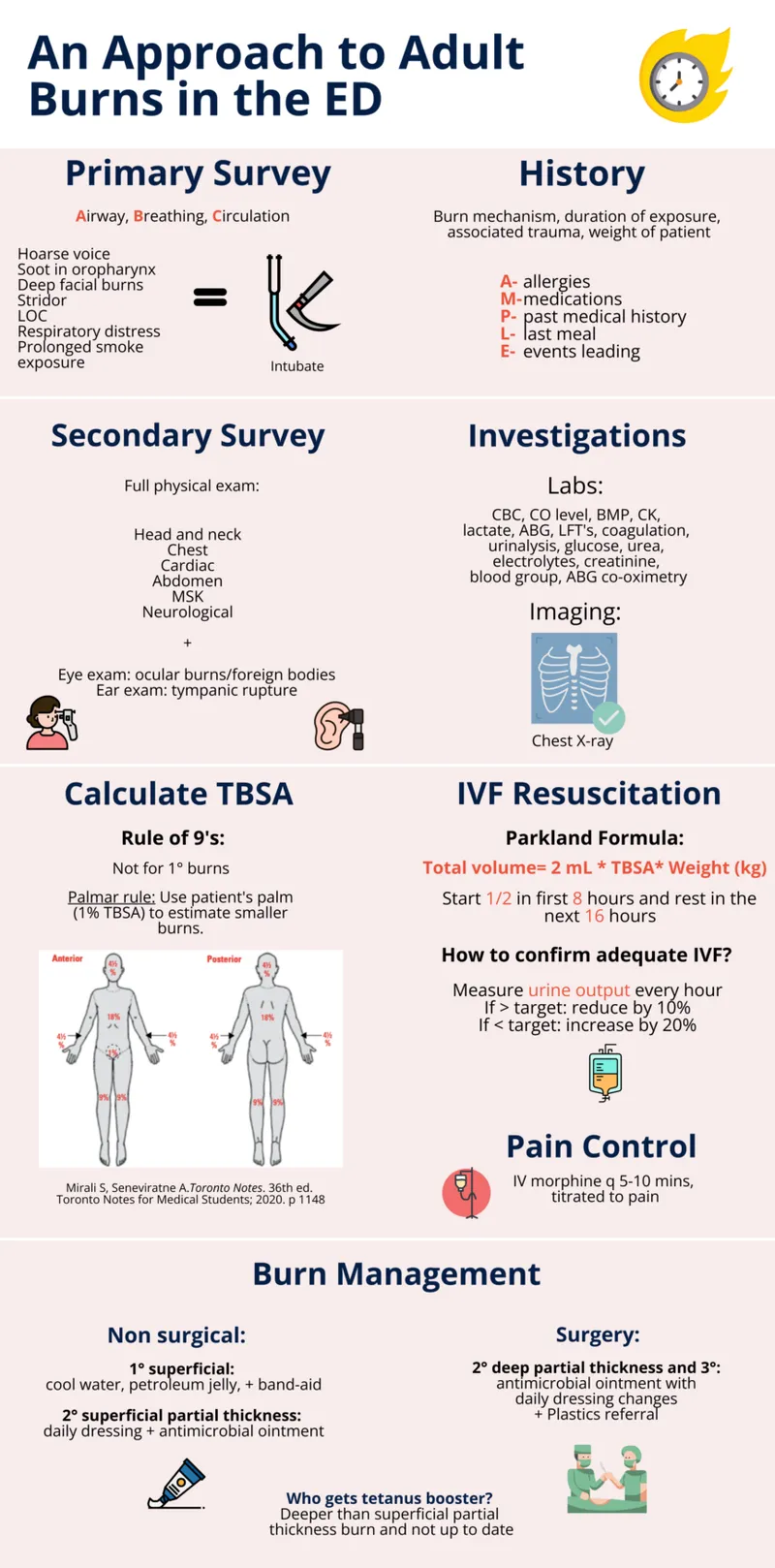
- Primary Survey (ABCDE) 📌:
- Airway: Secure early if inhalation injury suspected (e.g., facial burns, soot, hoarseness, stridor). Consider cricothyroidotomy if intubation fails.
- Breathing: 100% humidified O₂. Monitor for respiratory distress; chest escharotomy if needed.
- Circulation: Stop burning (cool water, not ice). IV access (2 large-bore cannulas, unburnt skin if possible). Commence fluid resuscitation.
- Disability: Assess GCS, pupils. Rule out associated trauma.
- Exposure/Environment: Remove clothing, keep patient warm to prevent hypothermia.
- Fluid Resuscitation (Crystalloids - Ringer's Lactate preferred):
- Parkland Formula: $4 \text{ml} \times \text{Body Wt (kg)} \times % \text{TBSA}$.
- Administration: 1st half in first 8 hours from time of burn, 2nd half in next 16 hours.
- Target Urine Output: Adults 0.5-1 ml/kg/hr; Children 1-1.5 ml/kg/hr.
- Children also need maintenance fluids (D5RL or D5NS).
⭐ The first half of the calculated Parkland fluid volume is administered in the first 8 hours from the time of burn injury, not from the time of hospital admission.
- Adjuncts:
- Analgesia: IV opioids (Morphine).
- Tetanus prophylaxis.
- NG tube: For burns >20% TBSA or intubated patients (prevents aspiration, ileus).
- Stress ulcer prophylaxis (PPIs/H2 blockers).
Wound Care & Complications - Healing The Hurt
- Wound Management:
- Cleaning: Gentle (e.g., chlorhexidine). Debride necrotic tissue.
- Dressings: Non-adherent, absorbent.
- Topical Agents:
- Silver Sulfadiazine (SSD): Painless. Risk: leucopenia, poor eschar penetration.
- Mafenide Acetate: Good eschar penetration. Risk: pain, metabolic acidosis.
- Silver Nitrate (0.5%): Risk: electrolyte imbalance (↓Na, ↓Cl), stains.
- Complications:
- Infection/Sepsis: Leading cause of late death.
- Contractures: Prevent with splinting, physiotherapy.
- Hypertrophic scars, Keloids.
- Marjolin's Ulcer: SCC in chronic burn wound.
- Escharotomy Indications (Circumferential Burns):
- Absent distal pulses; Impaired capillary refill.
- Chest: Respiratory compromise (SpO2 <90% on 100% O2).
⭐ Silver sulfadiazine is widely used but can cause transient leucopenia; Mafenide acetate penetrates eschar well but can cause metabolic acidosis due to carbonic anhydrase inhibition.
High‑Yield Points - ⚡ Biggest Takeaways
- Parkland formula (4ml x %TBSA x Wt) guides fluid resuscitation: 50% in first 8 hrs, remainder in next 16 hrs.
- Rule of Nines for adult TBSA estimation; Lund-Browder chart is more accurate, especially for children.
- Escharotomy is indicated for circumferential full-thickness burns causing compartment syndrome or respiratory compromise.
- Suspect inhalation injury with facial burns, singed nasal hairs, or sooty sputum; early intubation is critical.
- Silver sulfadiazine (SSD) is a common topical antimicrobial; Mafenide acetate penetrates eschar but is painful.
- Electrical burns: high risk of arrhythmias (monitor ECG) and rhabdomyolysis (myoglobinuria).
- Chemical burns: immediate copious water irrigation is key; identify the specific agent if possible (exceptions exist).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

