Initial Approach - Belly Bruises & Bleeds
- ABCDE (ATLS): Prioritize airway, breathing, circulation. Control external hemorrhage.
- Abdominal Exam:
- Inspect: Bruises (seatbelt, Cullen's, Grey Turner's), distension, wounds.
- Auscultate: Bowel sounds (absent/↓ in peritonitis/ileus).
- Palpate: Tenderness, guarding, rigidity, rebound.
- Percuss: Dullness (hemoperitoneum), tympany.
- Key Indicators of Intra-abdominal Bleed:
- Shock: Tachycardia, SBP < 90 mmHg, cool peripheries.
- Positive abdominal findings.
- Falling Hb/Hct.
- Diagnostic Adjuncts:
- FAST: For unstable patients, detects free fluid.
- CT Scan: Gold standard in stable. Details organ/retroperitoneal injury.
- DPL: If FAST unclear/unavail in unstable. Positive: >10mL blood, specific counts.

⭐ Seatbelt Sign: Indicates major force; high risk: bowel, mesenteric, lumbar spine (Chance #) injury.
Investigations - Scan, Scope, or Slice?
Guided by stability & mechanism.
- Unstable Patient:
- eFAST: Initial.
- Positive (hemoperitoneum) → Immediate Laparotomy ("Slice").
- Negative/Equivocal → DPL, or resuscitate & repeat eFAST. CECT if transiently stable.
-
⭐ Unstable blunt trauma + positive eFAST mandates direct laparotomy, avoiding imaging delays.
- eFAST: Initial.
- Stable Patient:
- eFAST: Initial screen.
- CECT Abdomen/Pelvis (Scan): Gold standard. Details injury, grade, active bleed (extravasation), retroperitoneum.
- Laparoscopy (Scope):
- Select penetrating trauma (anterior stab, tangential GSWs) for peritoneal/diaphragmatic assessment.
- Diagnostic & therapeutic.
- Diagnostic Peritoneal Lavage (DPL):
- Rare; if CECT/eFAST unavailable.
- Positive: >10mL gross blood aspirated; lavage: RBC >100,000/mm³, WBC >500/mm³.

Organ-Specific Injuries - Gut Reactions & Repairs
- General Principles: Control hemorrhage, prevent contamination. Repair vs. Resection & Anastomosis vs. Diversion. Damage Control Surgery (DCS) for unstable patients.
- Small Bowel Injury (Most common):
- Blunt (e.g., seatbelt sign, associated Chance fracture) or penetrating.
- Hematoma (non-expanding, intact serosa): Observation.
- Perforation: Primary repair (transverse closure).
- Multiple injuries close together / devitalized segment: Resection & anastomosis.
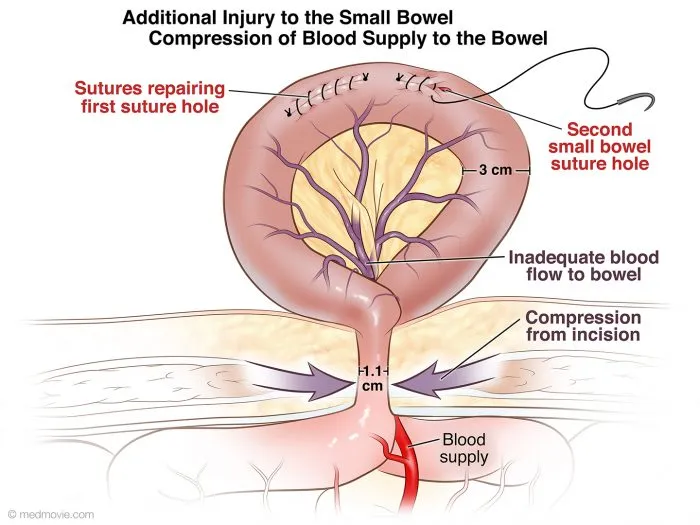
- Large Bowel Injury:
- Higher septic risk due to bacterial load.
- Management based on stability, contamination, time, location:
- Stable, minimal contamination: Primary repair or resection & anastomosis.
- Unstable, gross contamination, left colon: Hartmann's procedure (resection, end colostomy, rectal stump closure).
- Right colon: Right hemicolectomy & ileocolic anastomosis often feasible even with contamination.
- Stomach Injury:
- Rich blood supply, good healing.
- Management: Debridement & 2-layer primary repair.
- Duodenal Injury (Retroperitoneal, high risk):
- Often occult; Kocher maneuver for exposure.
- Hematoma: NG decompression, TPN; surgery if obstruction persists >1-2 weeks.
- Perforation (simple): Primary repair.
- Complex (D1/D2, >75% circumference, tissue loss): Pyloric exclusion + gastrojejunostomy (PE GJ).
⭐ Unexplained retroperitoneal air/fluid on CT, or persistent ↑serum amylase post-trauma, warrants high suspicion for duodenal injury.
- Rectal Injury:
- Intraperitoneal: Primary repair (like colon).
- Extraperitoneal: Proximal diversion (colostomy), presacral drainage, direct repair if accessible. 📌 3 D's: Diversion, Debridement, Drainage (distal washout controversial).
Special Considerations - Crisis Control & Aftermath
- Damage Control Surgery (DCS): For "triad of death" (acidosis, hypothermia, coagulopathy).
- Phase 1: Control hemorrhage/contamination, temporary abdominal closure.
- Phase 2: ICU resuscitation (correct physiology).
- Phase 3: Definitive surgical repair.
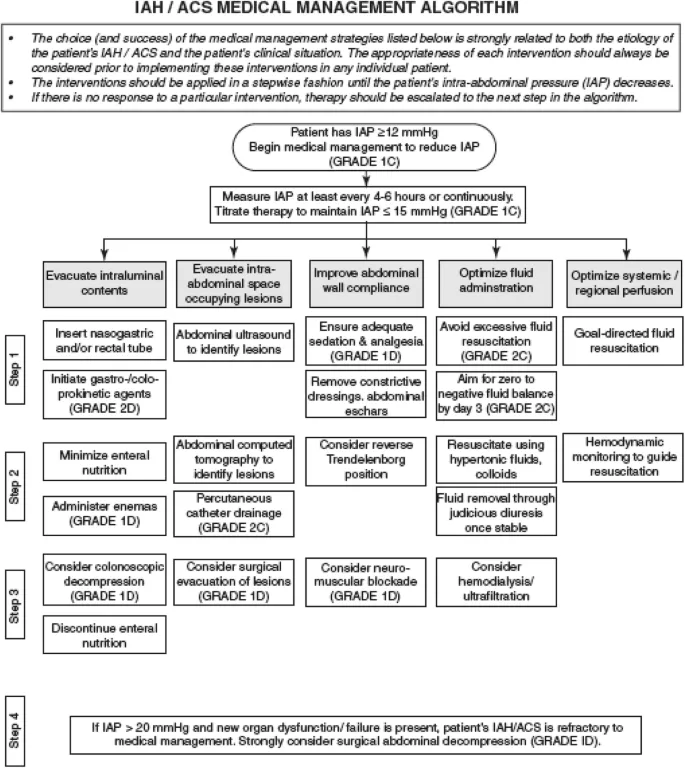
- Abdominal Compartment Syndrome (ACS):
- Intra-abdominal pressure (IAP) > 20 mmHg + new organ dysfunction.
- Tx: Urgent decompressive laparotomy.
- REBOA (Resuscitative Endovascular Balloon Occlusion of Aorta): For non-compressible torso hemorrhage. Zone 1 (supraceliac) / Zone 3 (infrarenal).
- Key Complications: Sepsis, ARDS, MODS. Crucial: VTE prophylaxis.
⭐ ACS mortality can be > 50% if decompressive laparotomy is delayed.
High-Yield Points - ⚡ Biggest Takeaways
- Spleen is most injured in blunt trauma (BAT); small bowel/liver in penetrating (PAT).
- FAST scan for hemoperitoneum in unstable patients; CT scan for stable patients.
- DPL for unstable patients if FAST unclear; >10 mL gross blood is positive.
- Exploratory laparotomy for unstable patients with positive FAST/DPL or evisceration.
- Seatbelt sign indicates high risk of hollow viscus injury & Chance fracture.
- Kehr's sign (left shoulder pain) suggests splenic injury.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

