Pancreas Transplant - Sweet Relief Quest
- Indications:
- Type 1 DM with ESRD (most common for SPK)
- Type 1 DM with recurrent severe metabolic complications (e.g., hypoglycemia, ketoacidosis)
- Selected Type 2 DM (controversial, specific criteria)
- Goals:
- Achieve euglycemia & insulin independence
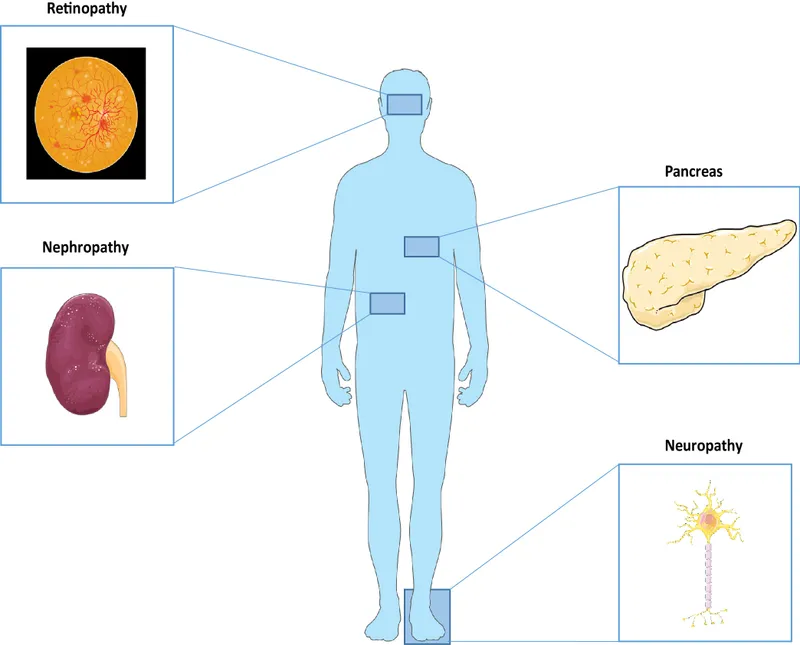
- Prevent/stabilize secondary diabetic complications (retinopathy, neuropathy, nephropathy)
- Improve quality of life
- Patient Selection:
- C-peptide status: Negative or low C-peptide indicates insulin deficiency.
- BMI: Generally <30 kg/m²
- Cardiovascular health: Adequate cardiac function essential.
- Absence of active infection or malignancy.
⭐ Simultaneous Pancreas-Kidney (SPK) transplant is the most common type of pancreas transplant performed worldwide for patients with Type 1 Diabetes and end-stage renal disease (ESRD).
Pancreas Plumbing - Guts & Glory
-
Transplant Types:
- SPK: Simultaneous Pancreas-Kidney (most common; T1DM + ESRD).
- PAK: Pancreas After Kidney (prior kidney transplant).
- PTA: Pancreas Transplant Alone (labile T1DM, good renal function).
-
Surgical Technique:
- Vascular Anastomosis:
- Arterial: Donor iliac artery Y-graft (from donor iliacs) to recipient iliacs.
- Venous: Donor portal vein to recipient SMV (portal drainage, more physiological) or IVC/iliac vein (systemic drainage).
- Exocrine Drainage:
- Enteric (Preferred): Duodenum to jejunum (Roux-en-Y). Pros: More physiological, ↓reflux. Cons: ↑Leak/infection risk.
- Bladder: Duodenum to bladder. Pros: Easy rejection monitoring (urine amylase). Cons: UTIs, acidosis, hematuria.
- Vascular Anastomosis:
⭐ Systemic venous drainage with enteric exocrine drainage is the most common surgical technique.
Rejection Rebuff - Immune Harmony
-
Immunosuppression:
- Induction: Anti-thymocyte globulin (ATG), Alemtuzumab, Basiliximab (IL-2R antagonist).
- Maintenance:
- Tacrolimus (CNI): Key SEs - nephrotoxicity, neurotoxicity.
- Mycophenolate Mofetil (MMF): Key SEs - GI upset, myelosuppression.
- Steroids (Prednisolone): Key SEs - hyperglycemia, Cushingoid.
- 📌 Mnemonic: Tacro Myco Stero (Tacrolimus, Mycophenolate, Steroids).
-
Monitoring for Rejection:
- Clinical: Fever, graft tenderness. Hyperglycemia (⚠️ late, often irreversible).
- Biochemical Markers:
- ↑ Serum Amylase/Lipase (exocrine dysfunction).
- ↓ C-peptide, ↑ Blood Glucose (endocrine dysfunction).
- ↑ HbA1c (glycemic control).
⭐ Monitoring serum lipase/amylase is useful, but hyperglycemia is a late and often irreversible sign of pancreas graft rejection.
-
Diagnosis of Rejection:
- Gold Standard: Graft biopsy (percutaneous/endoscopic).
Transplant Troubles - Pancreatic Perils
Surgical Complications:
- Vascular Thrombosis: Arterial or venous; critical early threat, major cause of graft loss.
- Anastomotic Leak: Enteric (duodenal stump) or vascular; can lead to sepsis.
- Graft Pancreatitis: Non-infectious inflammation; monitor amylase/lipase closely.
- Infection: Surgical site, intra-abdominal abscess, or systemic due to immunosuppression.
- Bleeding: Significant risk at anastomoses or from graft parenchyma.
- Duodenal Segment Issues: (If used) Leak, ulceration, bleeding, perforation, obstruction.
Medical Complications:
- Immunosuppression-Related:
- Nephrotoxicity: Esp. Calcineurin Inhibitors (CNIs) like Tacrolimus.
- Opportunistic Infections: CMV, BK virus, fungal; prophylaxis is key.
- Malignancy: Increased risk of PTLD, skin cancers.
- Metabolic:
- Hyperglycemia/NODAT: Steroid-induced or persistent insulin resistance.
- Dyslipidemia: Common; requires monitoring and active management.
⭐ Graft thrombosis is the leading cause of technical failure and early pancreas graft loss.

High‑Yield Points - ⚡ Biggest Takeaways
- SPK transplant (Simultaneous Pancreas-Kidney) is the most common type, primarily for Type 1 DM with ESRD.
- Enteric drainage of exocrine secretions is now standard, reducing urological complications.
- Vascular thrombosis (especially venous) is the most frequent cause of early graft failure.
- Acute rejection is common; graft biopsy remains the gold standard for diagnosis.
- Standard immunosuppression includes a calcineurin inhibitor, antimetabolite, and steroids.
- Monitor graft function via glucose levels; amylase/lipase are less specific with enteric drainage.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

