Indications & Scoring - Liver Lifeline Logic
Common Indications:
- Decompensated Cirrhosis (Viral, Alc, NASH)
- Acute Liver Failure (ALF)
- Hepatocellular Carcinoma (HCC) (within Milan Criteria)
- Metabolic/Cholestatic diseases (e.g., Wilson's, PSC)
Scoring Systems:
- MELD/PELD: Predicts 3-month mortality. MELD >15 common threshold.
- 📌 Mnemonic (MELD): I Crush Beer Daily (INR, Cr, Bili, Dialysis).
- MELD Components:
Comp. Detail Bilirubin Serum total INR Prothrombin Creatinine Serum Dialysis ≥2x/wk/CRRT
- King's College Criteria: For ALF prognosis/transplant need.
- Milan Criteria (HCC): 1 tumor ≤5cm OR ≤3 tumors ≤3cm each; no major vascular invasion or extrahepatic spread.
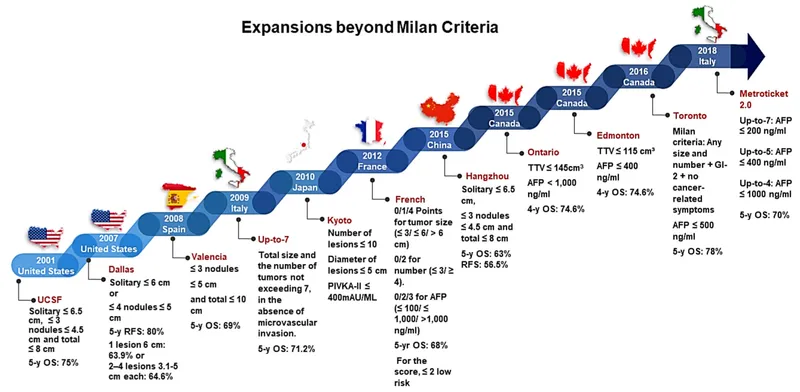
Key Contraindications:
- Absolute: Active sepsis, extrahepatic malignancy, severe cardiopulmonary disease, active substance abuse.
- Relative: Advanced age (>70), morbid obesity.
⭐ MELD score (Bilirubin, INR, Creatinine, Dialysis) is pivotal for liver allocation, predicting 3-month mortality; score >15 often triggers listing for transplant eligibility assessment.
Donor & Recipient Prep - The Perfect Match Mission
- Donors: Deceased (DBD/DCD) or Living (LDLT).
- ABO Compatibility: Crucial. Identical > Compatible.
Donor Evaluation Criteria:
- Deceased Donor (Ideal):
- Age <50 yrs (acceptable up to 60-65).
- BMI <30 kg/m².
- Steatosis (macrovesicular) <30%.
- Negative viral markers (HBsAg, Anti-HCV, HIV).
- Living Donor (LDLT):
- Age 18-55 yrs, voluntary, psychosocially stable.
- BMI <30 kg/m², Steatosis <10-15%.
- Adequate remnant liver volume (>30%), GRWR >0.8%.
Recipient Workup Essentials:
- Comprehensive cardiac, pulmonary, and renal function assessment.
- Infection screen: Viral (CMV, EBV, HIV, HBV, HCV), bacterial, fungal.
- Psychosocial evaluation and nutritional assessment.
⭐ For living donor liver transplantation (LDLT), a Graft-to-Recipient Weight Ratio (GRWR) of at least 0.8% is vital for adequate graft function and donor safety.
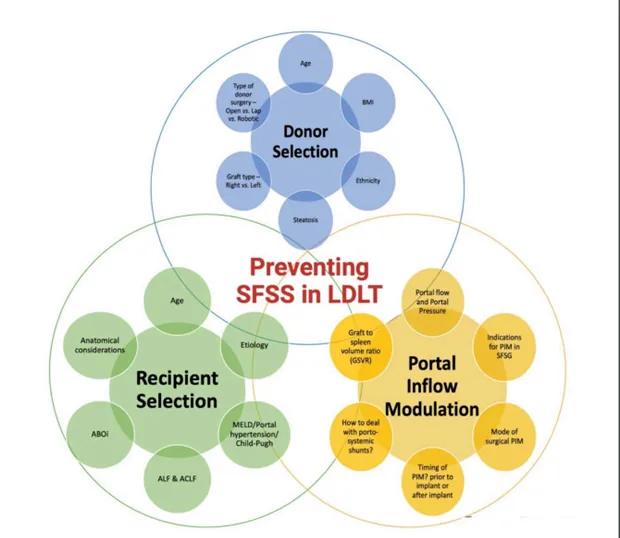
Surgical Highlights - Operation Liver Swap

- OLT: Standard. Piggyback (preserves recipient IVC, donor IVC to hepatic veins/side-clamped IVC) vs. conventional (IVC resection). Piggyback: better hemodynamics.
- Vascular Anastomoses (Order): 1. Suprahepatic IVC/Hepatic Veins 2. Portal Vein 3. Hepatic Artery.
- Biliary Reconstruction: Choledochocholedochostomy (duct-to-duct) or Roux-en-Y hepaticojejunostomy.
- Anhepatic Phase: Native liver out, before graft reperfusion. Veno-venous bypass (VVB) can maintain hemodynamic stability.
⭐ Hepatic artery thrombosis (HAT) is a dreaded early vascular complication, potentially leading to graft loss or biliary strictures.
Post-Op & Hurdles - Immunity & Issues
Immunosuppression:
| Class | Drugs | Key AEs |
|---|---|---|
| CNIs | Tacrolimus, Cyclosporine | Nephro/Neurotoxic, HTN, ↑Glucose. 📌 Tac: TANDH (Tremors, Alopecia, Nephrotoxic, Diabetes, HTN). CSA: Hirsutism, Gingival hyperplasia. |
| Antimetab. | MMF | GI upset, Myelosuppression. |
| Steroids | Prednisolone | Cushingoid, Osteoporosis, ↑Glucose. |
* Hyperacute: Mins-hrs, pre-formed Abs.
* Acute Cellular (ACR): **1-12 wks**, T-cell; Rx: Steroids.
* Chronic: >**6 mo**, ductopenia, arteriopathy.
- Complications:
- Infections: CMV, Fungal (Candida, Aspergillus).
- Vascular: Hepatic Artery Thrombosis (HAT), Portal Vein Thrombosis (PVT).
- Biliary: Leaks, Strictures.
- Disease Recurrence: HCV, HCC.

⭐ Acute cellular rejection is the most common type of rejection, typically occurring within the first few weeks to months post-transplant, and is usually responsive to steroid therapy.
High‑Yield Points - ⚡ Biggest Takeaways
- MELD score (bilirubin, INR, creatinine) dictates allocation priority.
- Milan criteria (1 tumor ≤5cm or ≤3 tumors each ≤3cm) for HCC transplant eligibility.
- Commonest indications: cirrhosis (adults), biliary atresia (children).
- Lifelong immunosuppression (e.g., tacrolimus, MMF) is crucial post-transplant.
- Key complications: rejection, infection (CMV), hepatic artery thrombosis, biliary strictures.
- Living donor liver transplantation (LDLT) offers an alternative to deceased donor organs.
- Orthotopic technique (OLT) is the standard surgical approach.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

