Indications & Workup - Kidney SOS Call
- Primary Indication: End-Stage Renal Disease (ESRD)
- GFR < 15 mL/min/1.73m² or on dialysis.
- Common Causes leading to ESRD:
- Diabetic Nephropathy (most frequent)
- Chronic Glomerulonephritis
- Hypertensive Nephrosclerosis
- Autosomal Dominant Polycystic Kidney Disease (ADPKD)
- 📌 SOS Criteria:
- Stage 5 CKD (ESRD: GFR < 15 or dialysis)
- Optimal medical therapy failed
- Suitable candidate (post-workup)
⭐ Diabetic nephropathy is the leading cause of ESRD requiring kidney transplantation in India.
Donor Selection & Surgery - New Kidney on Block
- Donor Types:
- Living: Related (HLA-identical best), unrelated (altruistic, paired kidney exchange).
- Deceased (Cadaveric): DBD (Donation after Brain Death), DCD (Donation after Circulatory Death).
- Key Donor Criteria:
- ABO compatibility.
- Negative T-cell crossmatch.
- Age 18-65 years (flexible).
- Normal renal function (GFR > 80 mL/min).
- No transmissible diseases (HIV, active Hepatitis B/C, active malignancy).
- Recipient Surgery:
- Gibson incision (extraperitoneal).
- Kidney placed in iliac fossa (usually right).
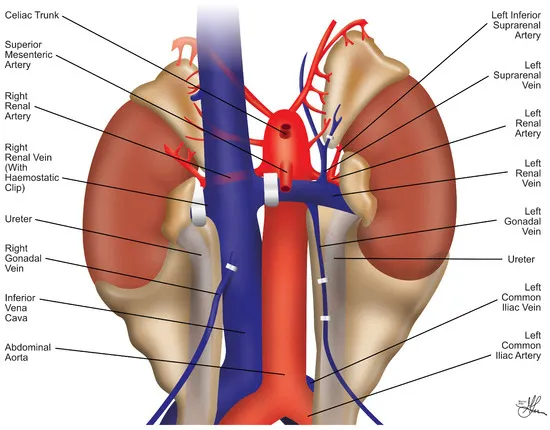
- Vascular Anastomosis:
- Renal artery to external/internal iliac artery.
- Renal vein to external iliac vein.
- Ureteroneocystostomy (e.g., Lich-Gregoir technique).
⭐ Most common site for renal artery anastomosis is the external iliac artery.
Immunosuppression Protocols - Peace Treaty Drugs
- Core Principle: Balance preventing graft rejection & minimizing drug toxicity.
- Phases & Typical Regimens:
- Induction (at transplant):
- Antibody therapy (Basiliximab, ATG) + high-dose steroids.
- Maintenance (long-term):
- Triple Therapy: Calcineurin Inhibitor (CNI: Tacrolimus/Cyclosporine) + Antiproliferative (Mycophenolate Mofetil [MMF]/Azathioprine) + Steroid (Prednisolone).
- CNI-sparing options: mTOR inhibitors (Sirolimus/Everolimus).
- Rejection Treatment:
- Acute Cellular Rejection (ACR): Pulse steroids; ATG for steroid-resistant cases.
- Antibody-Mediated Rejection (AMR): Plasmapheresis, IVIG, Rituximab.
- Induction (at transplant):
- Monitoring: Essential for CNIs (drug levels), renal function, infections, malignancies.
⭐ Mycophenolate Mofetil (MMF) generally offers better efficacy in preventing acute rejection than Azathioprine but is a known teratogen, contraindicated in pregnancy.
Rejection & Complications - Transplant Tremors
- Rejection Types:
- Hyperacute: Pre-formed Ab (ABO/HLA). Mins-hrs. Irreversible.
- Acute Cellular (ACR): T-cell. Days-months. Biopsy: Tubulitis. Rx: Steroids, ATG.
- Acute Humoral (AMR): DSA. Biopsy: C4d+. Rx: Plasmapheresis, IVIG, Rituximab.
- Chronic Allograft Dysfunction (CAD): Months-yrs. Fibrosis, atrophy. Multifactorial.
- Key Complications:
- Infections: CMV, BK virus nephropathy. Prophylaxis vital.
- Malignancy: PTLD (EBV), skin cancers.
- Cardiovascular disease: Major long-term risk.
- Transplant Tremors (CNI-induced):
- Cause: Calcineurin Inhibitors (Tacrolimus > Cyclosporine) neurotoxicity.
- Features: Fine, postural, action tremor. Dose-dependent.
- Mgmt: Optimize CNI levels, ↓dose or switch CNI, Propranolol.
⭐ Tacrolimus shows higher neurotoxicity (tremors, PRES) vs. Cyclosporine.

High‑Yield Points - ⚡ Biggest Takeaways
Error: Failed to generate content for this concept group.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

