Indications & Contraindications - Heart Swap Candidates
Indications:
- End-stage HF: NYHA Class III-IV (refractory)
- Severe systolic dysfunction: LVEF <20%
- Poor prognosis: Peak VO2 <10-14 mL/kg/min
- Refractory life-threatening arrhythmias
Contraindications:
- Absolute:
- Active infection or malignancy
- Irreversible severe pulmonary HTN (fixed $PVR > 5 \text{ Wood units}$)
- Irreversible significant renal/hepatic/pulmonary disease (non-cardiac)
- Active substance abuse; severe non-compliance
- Relative:
- Age >65-70 years
- Severe obesity ($BMI >35 \text{ kg/m}^2$)
- Poorly controlled DM with end-organ damage
- Significant PVD/CVD
⭐ Most common indications: End-stage ischemic cardiomyopathy & dilated cardiomyopathy.
Donor Selection & Management - Gifting a Beat
- Brain Death Criteria: Irreversible loss of all brain & brainstem functions.
- Age: Ideal <55 years (can extend to 65 in select cases).
- Cardiac Function: LVEF >50%, no significant CAD or valvular disease.
- No Active Infection/Malignancy: Screen for HIV, HBV, HCV.
- ABO Compatibility: Identical or compatible.
- PRA Screening: For recipient sensitization; Donor Specific Antibodies (DSA) ideally negative.
- Ischemic Time: Target <4-6 hours.
⭐ Ruling out active infection or malignancy in the donor is critical to prevent disease transmission to the recipient.
Surgical Procedure - Plumbing the Pump
Standard: Orthotopic transplantation (donor heart in normal anatomic position).
-
Techniques:
- Biatrial: Original technique. Involves anastomoses of LA, RA, Aorta, PA.
- Bicaval: Preferred. Anastomoses of LA, SVC, IVC, Aorta, PA.
⭐ Bicaval technique offers improved atrial hemodynamics, ↓ sinus node dysfunction, ↓ tricuspid regurgitation, and ↓ arrhythmias.
-
Key Anastomoses (General Order):
- Left Atrium (LA)
- Right Atrium (RA) / Superior Vena Cava (SVC) & Inferior Vena Cava (IVC)
- Pulmonary Artery (PA)
- Aorta (Ao)
- 📌 Mnemonic (Biatrial): "Lovely Rita Prefers Apples" (LA, RA, PA, Aorta)

Immunosuppression - Taming the Guard Dogs
- Induction: Basiliximab (IL-2R Ab), Anti-thymocyte Globulin (ATG) for high-risk patients.
- Maintenance: Triple therapy aims for long-term graft survival.
| Drug Class | Examples | Mechanism | Key Side Effects (📌 for CNIs) |
|---|---|---|---|
| Calcineurin Inhibitors (CNIs) | Tacrolimus, Cyclosporine | ↓IL-2 production | 📌 Nephro-, Neuro-toxicity, HTN, Hyperglycemia. Tacrolimus trough: 5-15 ng/mL |
| Antimetabolites | Mycophenolate (MMF), Azathioprine | Inhibit lymphocyte proliferation | GI intolerance, Myelosuppression |
| Corticosteroids | Prednisolone | Broad anti-inflammatory | Cushingoid features, Osteoporosis, Hyperglycemia |
Complications - Trouble in Paradise
- Rejection: Major threat; classified by timing, mechanism, histology.
Type Timing Key Features Hyperacute Mins-Hrs Pre-formed Ab (ABO/HLA); thrombosis, graft necrosis. Acute Cellular Wks-Mos T-cell mediated; lymphocytic infiltrate, myocyte damage (ISHLT Grades). Antibody-Med. Days-Wks Donor-Specific Ab (DSA), C4d+; microvascular inflammation, capillaritis. Chronic (CAV) >1 Yr Immune & non-immune; diffuse coronary intimal thickening. 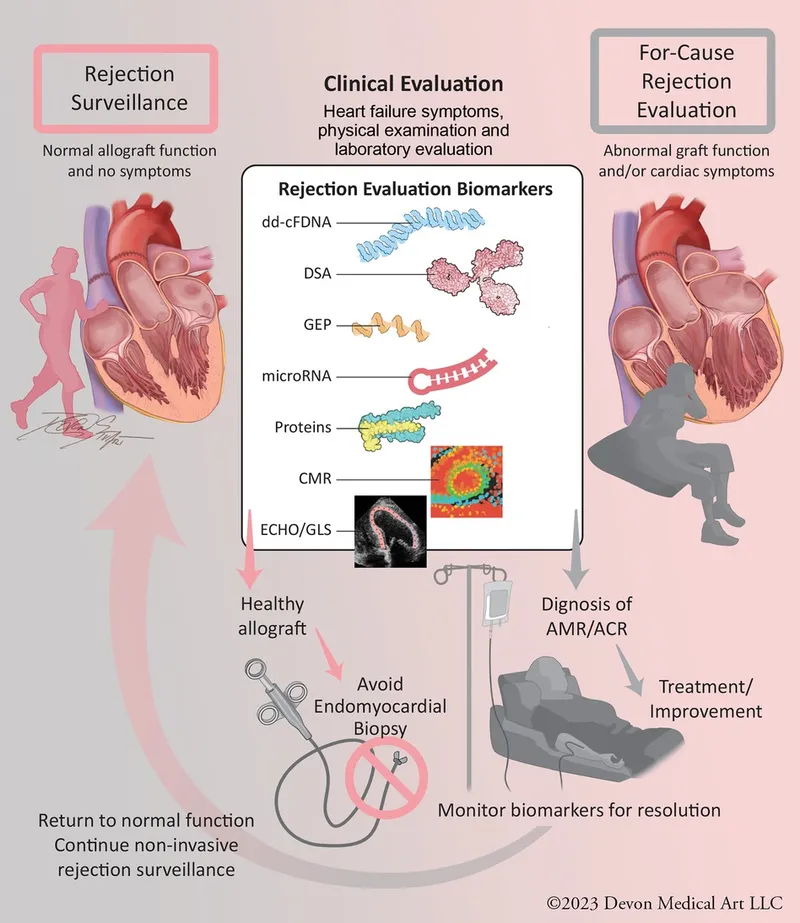
- Infections: High risk. CMV (prophylaxis/pre-emptive), Fungal (Aspergillus), PCP.
- Malignancy: PTLD (EBV-driven), ↑Skin Cancers.
- Drug-Related: Renal dysfunction (CNIs), Hypertension, Dyslipidemia, New-onset diabetes.
⭐ Cardiac Allograft Vasculopathy (CAV) is the leading cause of late graft failure and death post-heart transplant.
High‑Yield Points - ⚡ Biggest Takeaways
- Orthotopic heart transplantation (OHT) is the standard surgical approach.
- Bicaval anastomosis is preferred for superior atrial function and fewer arrhythmias.
- Endomyocardial biopsy (EMB) is gold standard for diagnosing acute cellular rejection.
- Maintenance immunosuppression: CNI, antiproliferative agent, and corticosteroids.
- Cardiac Allograft Vasculopathy (CAV) is a major cause of late graft dysfunction.
- Pravastatin reduces CAV incidence and mortality.
- Absolute contraindications: active infection, recent malignancy, fixed severe pulmonary hypertension.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

