Transplant Rejection - Attack of the Clones
- Recipient's immune system attacks donor alloantigens (MHC/HLA).
- Types & Timing (📌 Mnemonic: Hot Apple Crumble):
-
Hyperacute Rejection:
- Minutes to hours.
- Cause: Pre-formed anti-donor antibodies (e.g., ABO, anti-HLA Class I).
- Mechanism: Type II Hypersensitivity. Results in complement activation, endothelial damage, thrombosis, graft necrosis.
-
Acute Rejection:
- Days to weeks (usually <6 months); most common type.
- Cellular: CD8+ T-cells (cytotoxic) directly damage graft; CD4+ T-cells (helper) mediate inflammation. Type IV HSR.
- Humoral: Anti-donor antibodies (de novo or anamnestic) target graft vasculature. Type II HSR.
-
Chronic Rejection:
- Months to years. Often irreversible, leading to progressive graft failure.
- Mechanism: Complex; involves cellular and humoral immunity, cytokines, growth factors.
- Pathology: Vascular changes (graft arteriosclerosis), interstitial fibrosis, parenchymal atrophy.
-
- Diagnosis: Graft biopsy is the gold standard.
- Prevention: HLA matching, immunosuppressive drugs.
⭐ Acute cellular rejection, primarily mediated by T-lymphocytes, is the most common form of rejection and is often reversible with increased immunosuppression.
Post-Transplant Infections - Bugs on Board
Post-transplant infections impact outcomes. Timing reveals likely pathogens. Immunosuppression level is key.

- Common Pathogens & Concerns:
- CMV: Pneumonitis, GI disease, hepatitis. Prophylaxis/pre-emptive therapy common.
- PJP: Interstitial pneumonia. TMP-SMX prophylaxis.
- Aspergillus: Invasive pulmonary disease, high mortality.
- BK Virus: Polyomavirus nephropathy in renal transplants.
- Key Prophylaxis Durations:
- PJP: TMP-SMX for 6-12 months.
- CMV: Valganciclovir/Ganciclovir for high-risk (D+/R-), typically 3-6 months.
- Fungal (Candida): Fluconazole for early post-op period.
- HSV/VZV: Acyclovir/Valacyclovir if seropositive.
⭐ CMV is the most common opportunistic infection in Solid Organ Transplant (SOT) recipients, typically occurring 1-6 months post-transplant, causing fever, leukopenia, or organ-specific disease.
Drug Side Effects & PTLD - Pills & Perils
- Calcineurin Inhibitors (CNIs): Nephrotoxicity, neurotoxicity, HTN, hyperglycemia.
- Cyclosporine: 📌 "Cyclo Spor Hirsute Gums" (Hirsutism, Gingival hyperplasia).
- Tacrolimus: Alopecia, ↑diabetes risk.
- Antiproliferatives:
- Mycophenolate (MMF): GI upset (diarrhea), leukopenia.
- Azathioprine: Myelosuppression, pancreatitis.
- mTOR Inhibitors (Sirolimus, Everolimus):
- Hyperlipidemia, impaired wound healing, mouth ulcers, pneumonitis.
- Corticosteroids:
- Cushingoid features, hyperglycemia, osteoporosis, ↑infection risk.
- PTLD (Post-Transplant Lymphoproliferative Disorder):
- EBV-driven lymphoma; risk ↑ with immunosuppression intensity.
- Sx: Fever, lymphadenopathy.
- Rx: Reduce immunosuppression, Rituximab.
⭐ PTLD is most commonly associated with Epstein-Barr Virus (EBV) infection in transplant recipients.
GVHD & Other Complications - Graft's Grudge
- Graft-versus-Host Disease (GVHD): Donor T-cells attack recipient tissues. 📌 Targets: Skin, Liver, Gut.
- Acute GVHD: Develops <100 days. Affects skin (maculopapular rash), liver (↑bilirubin, ↑LFTs), GIT (diarrhea, pain).
- Chronic GVHD: Develops >100 days. Autoimmune-like; multi-organ (skin, mouth, eyes, joints, lungs).
- Prophylaxis/Treatment: Immunosuppressants (CNIs, methotrexate), steroids.
- Surgical Complications:
- Vascular: Arterial/venous thrombosis, stenosis.
- Organ-specific: Biliary strictures/leaks (liver); lymphocele, urinoma (kidney).
- General: Wound infection, dehiscence.
- Long-term Sequelae:
- Malignancy: PTLD (EBV-associated), skin cancers (SCC > BCC), Kaposi sarcoma.
- Cardiovascular disease (accelerated).
- Nephrotoxicity (CNIs).
- Opportunistic infections.
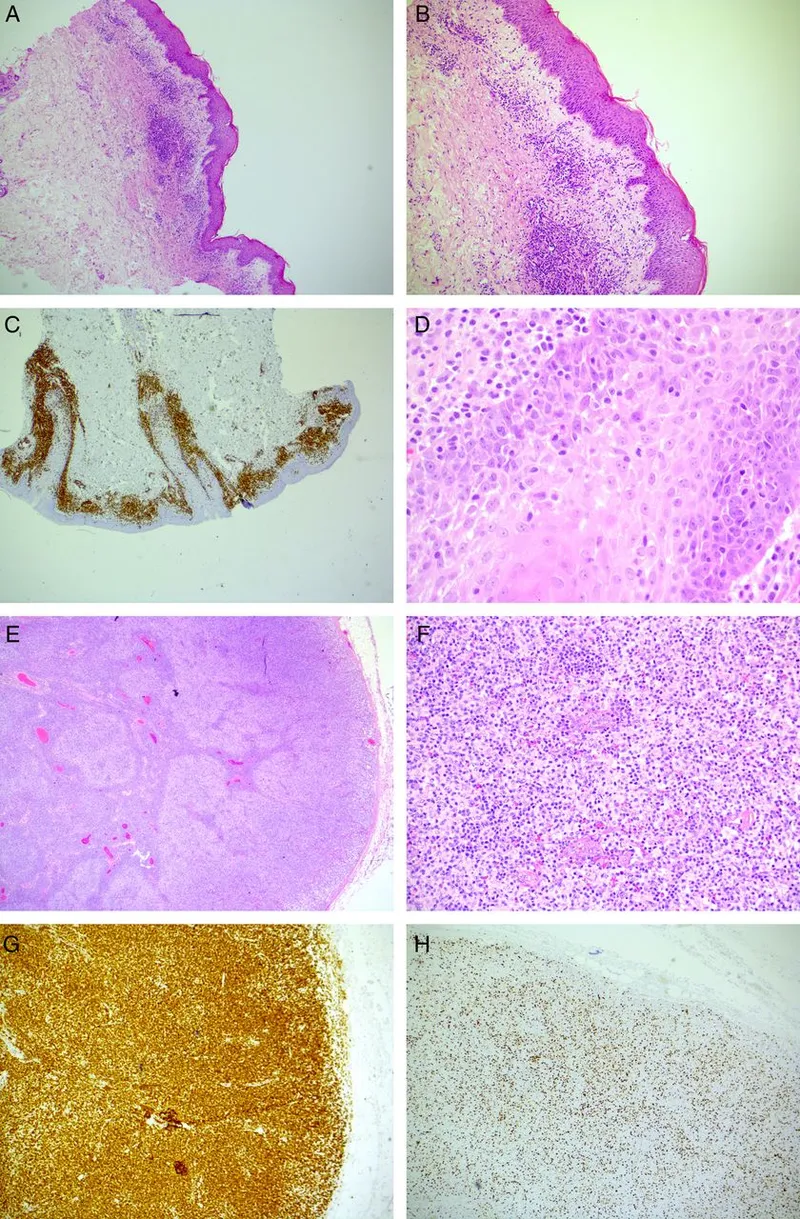
⭐ Post-Transplant Lymphoproliferative Disorder (PTLD) is a significant EBV-related malignancy risk, especially in the first year.
High‑Yield Points - ⚡ Biggest Takeaways
- Hyperacute rejection is antibody-mediated (Type II hypersensitivity), occurring minutes to hours post-transplant.
- Acute rejection, typically T-cell mediated (Type IV), occurs days to weeks later; it's the most common type.
- Chronic rejection involves fibrosis and scarring, leading to graft loss over months to years.
- Opportunistic infections like CMV, PJP, and BK virus are significant post-transplant risks.
- Increased risk of malignancies, especially PTLD (EBV-related) and skin cancers.
- Calcineurin inhibitor toxicity (e.g., nephrotoxicity, neurotoxicity) is a major long-term concern.
- Graft-versus-host disease (GVHD) is a critical complication, especially in bone marrow transplants but can occur in solid organs too.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

