Targeted Therapy Concepts - Precision Strikes
- Principle: Drugs targeting specific molecules (proteins, genes) vital for cancer cell growth & survival.
- Action: Blocks specific cancer signals; distinct from chemotherapy's broad cytotoxicity.
- Key Features:
- Targets: EGFR, HER2, VEGF, BRAF, ALK, BCR-ABL.
- Biomarkers: Predictive; guide patient selection (e.g., KRAS for anti-EGFR therapy).
- Drug Classes:
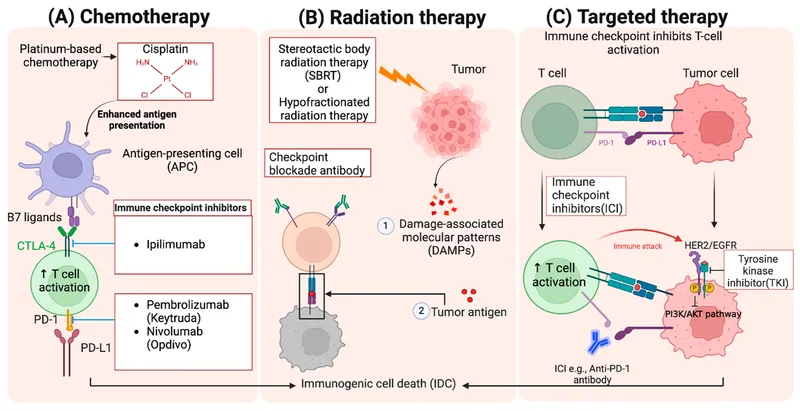
- Monoclonal Antibodies (-mab): Target extracellular/surface molecules (e.g., Trastuzumab for HER2+ breast cancer).
- Small Molecule Inhibitors (-nib): Target intracellular molecules (e.g., Imatinib for CML).
- Benefits: ↑Efficacy in selected patients; often ↓severe side effects than chemo.
- Limitations: Acquired resistance; target heterogeneity.
⭐ KRAS mutation in colorectal cancer predicts resistance to anti-EGFR monoclonal antibodies (e.g., Cetuximab).
Targeted Therapy Concepts - Unlocking Cancer's Code
- Principle: Drugs targeting specific molecules (proteins, genes) crucial for cancer cell growth, progression, and spread. "Lock and key" action against molecular aberrations.
- Action: Interfere with aberrant signaling pathways. Biomarker testing (e.g., EGFR, HER2, BRAF, BRCA) essential to identify susceptible patients.
- Key Classes & Targets:
- Tyrosine Kinase Inhibitors (TKIs) (small molecules):
- EGFR: Gefitinib, Erlotinib
- HER2: Lapatinib
- BCR-ABL: Imatinib
- ALK: Crizotinib
- BRAF: Vemurafenib
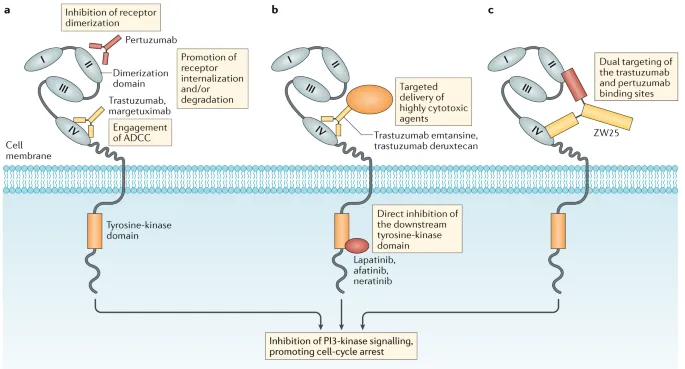
- Monoclonal Antibodies (mAbs) (large molecules):
- HER2: Trastuzumab
- EGFR: Cetuximab
- VEGF (Angiogenesis): Bevacizumab
- PARP Inhibitors: Olaparib (for BRCA mutations)
- mTOR Inhibitors: Everolimus
- Tyrosine Kinase Inhibitors (TKIs) (small molecules):
- Advantages: Higher specificity, potentially fewer severe side effects than traditional chemotherapy; improved therapeutic window.
- Challenges: Drug resistance (primary/acquired), unique side-effect profiles (e.g., skin rash, cardiotoxicity).
⭐ Imatinib, a TKI targeting BCR-ABL, revolutionized Chronic Myeloid Leukemia (CML) treatment.
Targeted Therapy Concepts - Surgeon's Smart Bombs
- Precision drugs attacking specific molecules (genes, proteins) vital for cancer cell growth and survival.
- Key Mechanisms:
- Tyrosine Kinase Inhibitors (TKIs): Intracellularly block aberrant signaling (e.g., Imatinib).
- Monoclonal Antibodies (mAbs): Extracellularly target cell surface receptors or ligands (e.g., Trastuzumab, Bevacizumab).
- Biomarker testing is crucial for patient selection:
- HER2 for Trastuzumab.
- EGFR mutations for Gefitinib/Erlotinib.
- KRAS wild-type for Cetuximab/Panitumumab.
- Challenges include acquired resistance and unique side-effect profiles (e.g., skin rash with EGFR inhibitors).
| Drug | Class | Target(s) | Key Surgical Indication(s) |
|---|---|---|---|
| Imatinib | TKI | BCR-ABL, c-KIT | GIST (Gastrointestinal Stromal Tumor) |
| Trastuzumab | mAb | HER2 | HER2+ Breast Cancer, Gastric Cancer |
| Bevacizumab | mAb | VEGF | Colorectal Ca, RCC, Ovarian Ca |
| Cetuximab | mAb | EGFR | KRAS wt Colorectal Ca, H&N Cancer |
Targeted Therapy Concepts - Evolving Battlefront
- Challenges: Drug resistance is a major hurdle.
- Primary (Intrinsic) Resistance: Cancer cells don't respond from the outset.
- Pre-existing mutations (e.g., KRAS in EGFR therapy for CRC).
- Tumor heterogeneity.
- Acquired (Secondary) Resistance: Develops after initial response.
- New mutations in the target (e.g., T790M in EGFR for NSCLC).
- Activation of bypass pathways.
- Phenotypic switching (e.g., EMT).
- Primary (Intrinsic) Resistance: Cancer cells don't respond from the outset.
- Overcoming Resistance:
- Combination therapies.
- Next-generation inhibitors.
- Intermittent dosing strategies.
- Future Directions:
- Liquid biopsies (ctDNA) for monitoring resistance & guiding therapy.
- Novel targets & immunotherapies.
- AI in drug discovery & personalized medicine.
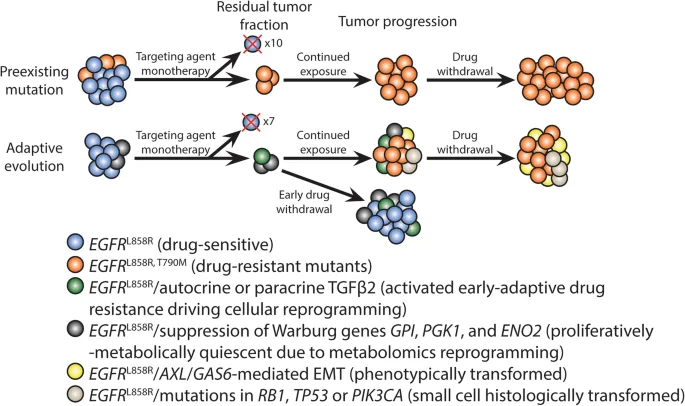
⭐ Acquired resistance to Imatinib in CML is often due to point mutations in the ABL kinase domain, with T315I being a common culprit conferring broad TKI resistance (except Ponatinib).
High‑Yield Points - ⚡ Biggest Takeaways
- Monoclonal antibodies (mAbs) end in "-mab"; Tyrosine Kinase Inhibitors (TKIs) in "-tinib".
- Trastuzumab targets HER2/neu receptor, crucial in HER2+ breast and gastric cancers.
- Rituximab targets CD20 antigen on B-lymphocytes, used for lymphomas.
- Bevacizumab inhibits VEGF, blocking angiogenesis in colorectal, lung, renal cancers.
- Imatinib targets BCR-ABL tyrosine kinase in CML and c-KIT in GIST.
- EGFR inhibitors (e.g., Cetuximab) require KRAS wild-type status for colorectal cancer treatment.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

