Understanding Metastasis - Mets 101: Seed & Soil
- Metastasis: Spread of malignant cells from primary tumor to form secondary tumors at distant, non-contiguous sites.
- Seed & Soil Hypothesis (Paget, 1889):
- "Seed": Circulating Tumor Cells (CTCs) with metastatic potential.
- "Soil": Favorable distant organ microenvironment (e.g., specific growth factors, chemokines).
- Explains organotropism: non-random, site-specific metastasis.
- Metastatic Cascade:
- Local invasion → Intravasation → Survival in circulation → Extravasation → Micrometastasis → Angiogenesis → Colonization.
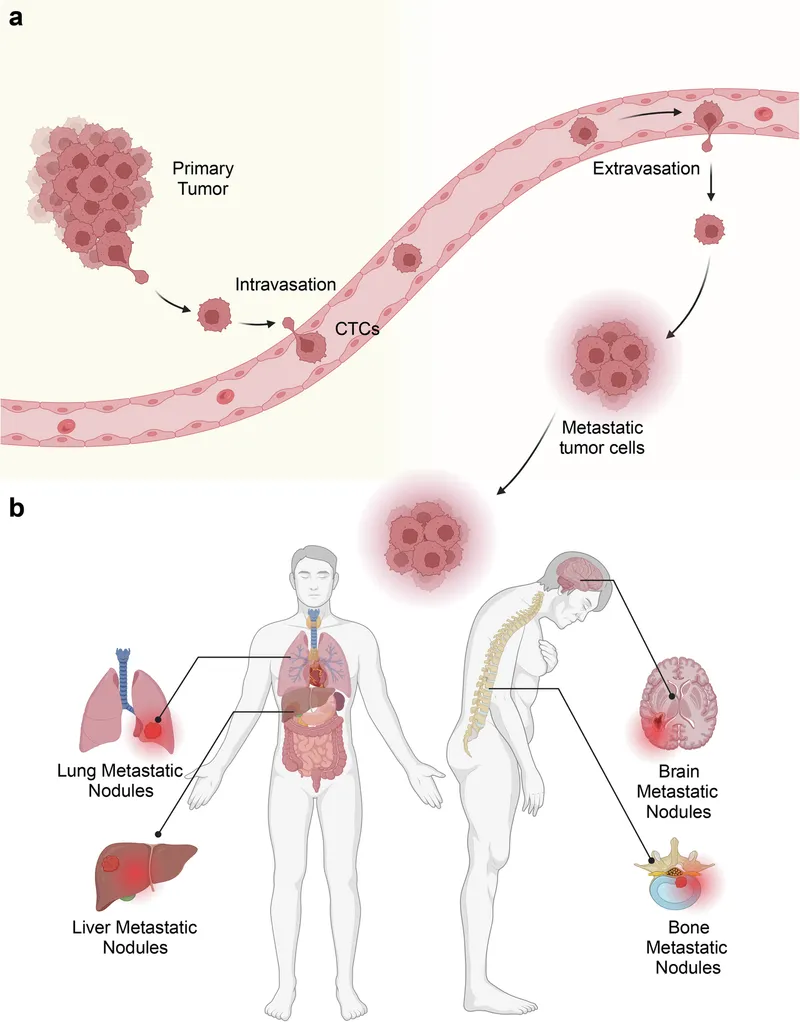
- Local invasion → Intravasation → Survival in circulation → Extravasation → Micrometastasis → Angiogenesis → Colonization.
⭐ Common metastatic sites (fertile "soil"): Lung, Liver, Bone, Brain. (📌 LLBB: Love Large Beer Bottles).
Diagnosing & Staging Metastases - Scan, Scope, Stage!
- Scan (Imaging Workup):
- CECT (Chest, Abdomen, Pelvis): Baseline.
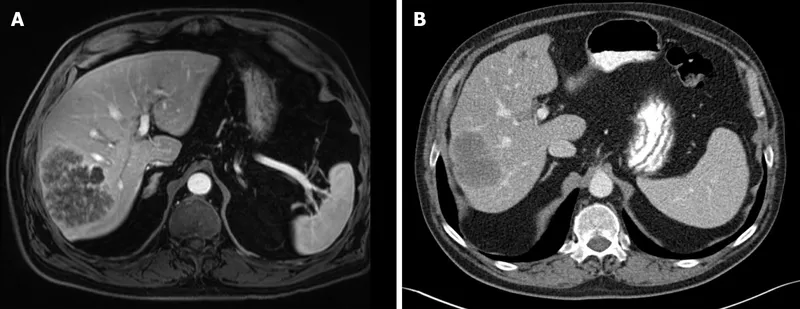
- MRI: Brain, liver, bone specifics.
- PET-CT: Whole-body survey for occult disease, response assessment.
- 📌 Positive Emission Tomography Can Tell all!
- Scope & Biopsy (Confirmation):
- Image-guided or endoscopic biopsy of suspicious lesions.
- Histopathology: Confirms metastasis, identifies primary if unknown.
- Molecular markers (e.g., ER, HER2, PD-L1): Guides targeted therapy.
- Stage (Assessment):
- AJCC TNM Staging (8th ed.): Defines M1 (metastatic) disease.
- Performance Status (ECOG/Karnofsky): Guides treatment feasibility.

⭐ PET-CT is superior to conventional imaging for detecting distant metastases in many cancers, altering management in up to 20-30% of cases.
Surgical Management of Metastases - Cut the Clones!
Surgical removal of metastases (metastasectomy) aims for cure or prolonged survival in selected patients with oligometastatic disease.
-
Indications for Metastasectomy:
- Primary tumor controlled or controllable.
- Limited number and sites of metastases (oligometastases).
- Patient medically fit for major surgery.
- No effective alternative systemic therapy or progression despite it.
- Favorable tumor biology (e.g., long disease-free interval).
-
Patient Selection:
- Good performance status (ECOG 0-1).
- Adequate organ reserve.
- Resectability of all known disease (aim for R0).
-
Common Sites & Considerations:
- Liver: Most common for CRC; aim for ≥1 cm margin.
- Lung: CRC, sarcoma, RCC; wedge, segmentectomy, or lobectomy.
- Brain: Solitary, accessible lesions; often with radiotherapy.
- Adrenal: Isolated metastasis, e.g., from lung cancer.
-
Core Principles:
- Achieve R0 resection (microscopically negative margins).
- Preserve maximal organ function.
- Repeat metastasectomy is feasible in select cases.
-
MDT Approach: Crucial for decision-making, involving surgeons, oncologists, radiologists.
⭐ For colorectal liver metastases, 5-year survival after complete R0 resection can reach 40-50% in appropriately selected patients.
Non-Surgical & Palliative Approaches - Ease & Eradicate Extras
Error: Failed to generate content for this concept group.
High‑Yield Points - ⚡ Biggest Takeaways
- Oligometastases: Limited metastatic burden potentially curable with local therapies (surgery, SBRT).
- Liver metastasectomy: Key for colorectal cancer (CRC); R0 resection is crucial.
- Lung metastasectomy: Improves survival in selected sarcomas and CRC patients.
- CRS + HIPEC: For specific peritoneal metastases (e.g., appendiceal, ovarian, mesothelioma).
- Brain metastases: Surgery/SRS for limited lesions; WBRT for multiple.
- Bone metastases: Surgery for stabilization/decompression; radiotherapy and systemic agents are vital.
- Careful patient selection and multimodal treatment are essential for optimal outcomes.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

