Survivorship Basics - Beyond the Battle
- Definition: An individual is a cancer survivor from diagnosis through the balance of life. Includes family, friends, and caregivers.
- Phases (NCI Model):
- Acute Survivorship: Diagnosis & initial treatment. Focus: active cancer therapy, symptom management.
- Extended Survivorship: End of initial treatment to months after. Focus: recovery, managing short-term effects, emotional impact.
- Permanent/Long-term Survivorship: Years post-treatment. Focus: managing long-term/late effects, quality of life, ongoing surveillance for recurrence or new cancers.
- Core Goals:
- Prevention & management of late effects.
- Surveillance for recurrence & second primary cancers.
- Psychosocial well-being & support.
- Coordinated follow-up care.
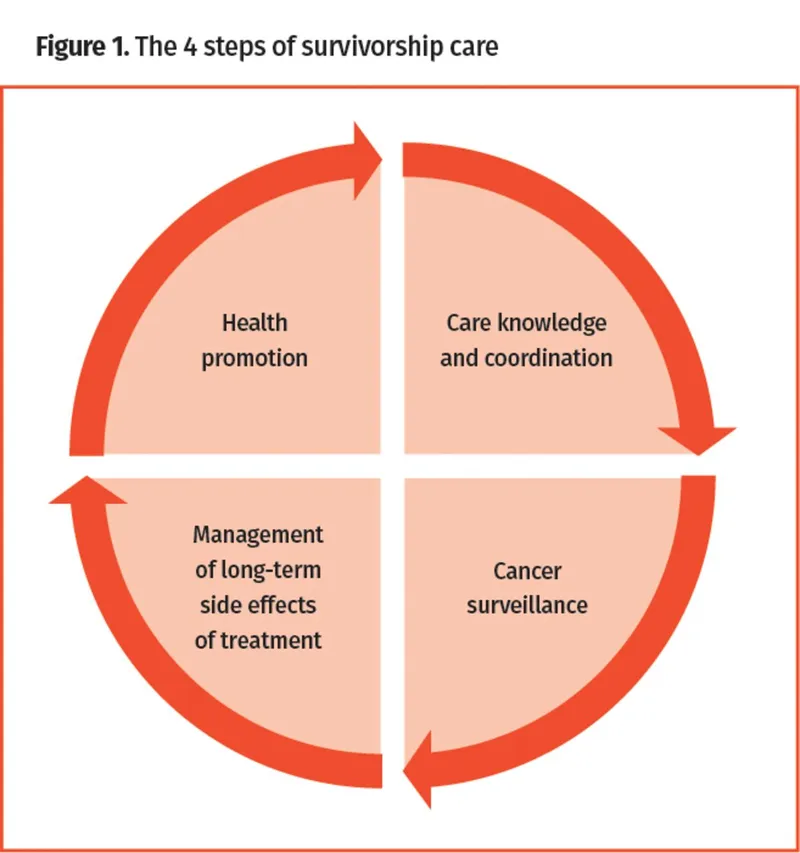
⭐ Survivorship Care Plans (SCPs) are essential, providing a treatment summary, follow-up schedule, and information on potential late effects and wellness strategies for the patient and primary care provider (PCP).
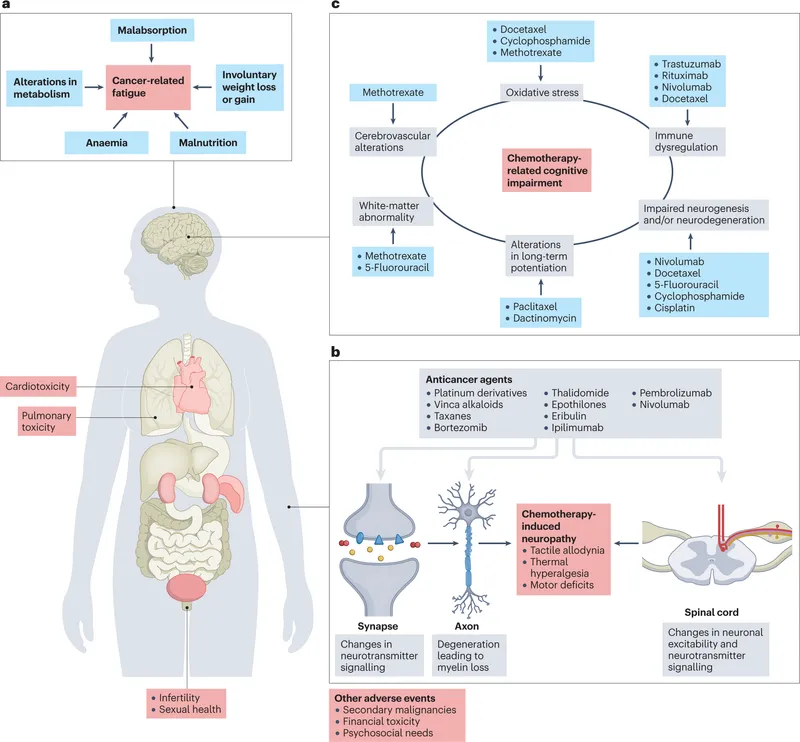
Late Effects of Cancer Tx - Lingering Shadows
- Cardiovascular Toxicity:
- Anthracyclines (Doxorubicin): Dose-dependent cardiomyopathy (< 450-550 mg/m²).
- Trastuzumab: Reversible LV dysfunction.
- Radiation: Pericarditis, CAD, valvulopathy.
- Pulmonary Toxicity:
- Bleomycin, Busulfan: Pulmonary fibrosis.
- Radiation: Pneumonitis/fibrosis.
- Endocrine & Reproductive:
- Hypothyroidism (Neck RT).
- Infertility, premature gonadal failure (Alkylating agents, RT).
- Musculoskeletal:
- Osteoporosis/fractures (Steroids, AIs).
- Avascular necrosis.
- Neurological:
- Peripheral neuropathy (Vincas, Taxanes, Platinum).
- "Chemo brain": Cognitive impairment.
- Second Malignancies:
- t-AML/MDS (Alkylating agents, Topo II inhibitors like Etoposide, RT).
- RT-induced solid tumors (e.g., sarcomas, thyroid Ca).
⭐ RT-induced sarcomas: 5-15 yrs latency period.
- Psychosocial:
- Anxiety, depression, PTSD.
- Chronic fatigue, persistent pain.
- Body image, sexual dysfunction.
- Other:
- Lymphedema (Axillary/inguinal node dissection/RT).
- CKD (Cisplatin).
Survivorship Care - Watching Horizon
- Goal: Smooth transition from active treatment; optimize Quality of Life (QoL), monitor for recurrence, manage late effects.
- Survivorship Care Plan (SCP): Cornerstone; individualized.
- Treatment summary (diagnosis, therapies).
- Follow-up plan (surveillance, screening for new cancers).
- Potential late/long-term effects & management.
- Wellness strategies (diet, exercise, mental health).
- Key Focus Areas:
- Early detection of recurrence.
- Screening for Second Primary Malignancies (SPMs).
- Managing late effects (e.g., cardiotoxicity, neuropathy, lymphedema, psychosocial issues).
- Addressing comorbidities.
- Approach: Multidisciplinary Team (MDT) vital. Emphasize patient education & empowerment.
⭐ A personalized Survivorship Care Plan (SCP) significantly improves coordination of care and addresses long-term health needs of cancer survivors.
Health Promotion in Survivors - Thriving Anew
- Goal: Enhance QoL, prevent recurrence/second cancers, manage long-term effects.
- Lifestyle Pillars:
- Nutrition: Plant-rich diet, healthy weight (BMI 18.5-24.9 kg/m²).
- Physical Activity: ≥150 min/wk moderate or ≥75 min/wk vigorous aerobic exercise; strength training ≥2x/wk.
- Avoid Tobacco: Crucial for all.
- Limit Alcohol: Per national guidelines.
- Psychosocial Well-being:
- Screen for distress (anxiety, depression); offer support/counseling.
- Preventive Measures:
- Vaccinations: Annual flu, pneumococcal (per guidelines).
- Sun protection: SPF ≥30 & protective clothing.
- Address Specific Needs:
- Manage: sexual dysfunction, "chemo brain", bone health (Ca/Vit D).

- Manage: sexual dysfunction, "chemo brain", bone health (Ca/Vit D).
⭐ Regular physical activity post-diagnosis ↓ recurrence & mortality risk in common cancers (breast, colorectal, prostate).
High‑Yield Points - ⚡ Biggest Takeaways
- Cancer survivorship starts at diagnosis, encompassing the entire cancer journey.
- Focus: surveillance for recurrence, second primary cancers, and managing late effects.
- Key late effects: cardiotoxicity, neuropathy, lymphedema, infertility, psychosocial issues.
- Risk of second primary cancers is ↑ due to treatment or genetics.
- Survivorship Care Plans (SCPs) guide long-term follow-up and patient education.
- Integral psychosocial support addresses anxiety, depression, and fear of recurrence.
- Promote healthy lifestyle: diet, exercise, smoking cessation for better long-term health.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

