Hallmarks of Cancer - Rebel Cell Rules
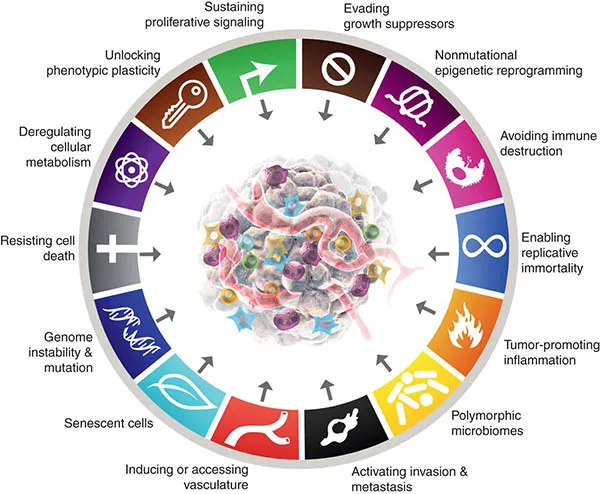
- Sustaining proliferative signaling: Uncontrolled cell growth.
- Evading growth suppressors: Ignoring "stop" signals (e.g., p53, RB loss).
- Resisting cell death: Bypassing apoptosis.
- Enabling replicative immortality: Unlimited cell divisions (telomerase).
- Inducing angiogenesis: Forming new blood vessels (VEGF).
- Activating invasion & metastasis: Spreading to distant sites.
- Deregulating cellular energetics: Warburg effect (aerobic glycolysis).
- Avoiding immune destruction: Hiding from immune system.
- Genome instability & mutation: ↑ Genetic alterations.
- Tumor-promoting inflammation: Inflammation aiding cancer.
⭐ Loss of function of the TP53 tumor suppressor gene is the most common genetic alteration in human cancers, occurring in >50% of cases.
Oncogenes & TSGs - Genes Gone Wild
- Oncogenes: Arise from proto-oncogenes; drive cell growth (gain-of-function).
- "Gas pedal" ➔ Uncontrolled proliferation.
- Activation: Mutation, amplification, translocation.
- Examples: RAS, MYC, HER2/neu (ERBB2), ABL, EGFR.
- Dominant: Single allele mutation is sufficient.
- Tumor Suppressor Genes (TSGs): Normally halt cell cycle, induce apoptosis, or repair DNA.
- "Brake pedal" ➔ Failure to control growth.
- Inactivation: Mutations, deletions, methylation (loss-of-function).
- Knudson's "two-hit" hypothesis often applies.
- Examples: p53, RB1 (retinoblastoma), BRCA1/2, APC, PTEN.
- 📌 Oncogenes = On (accelerate); TSGs = Stop (brake).
⭐ p53, the "guardian of the genome," is mutated in over 50% of human cancers.
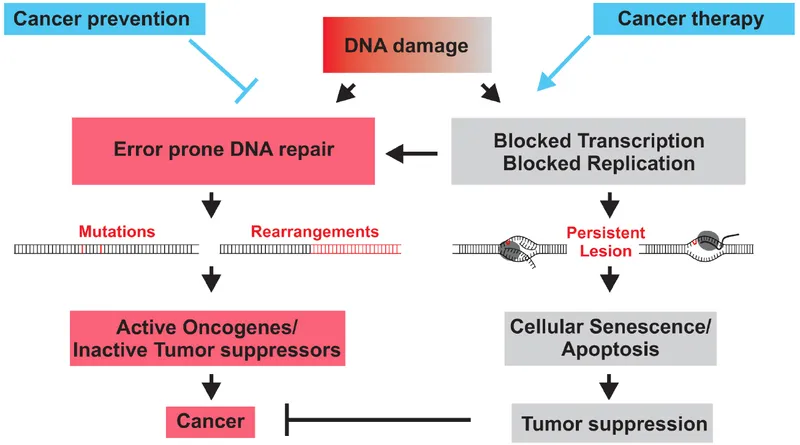
Cell Cycle & Regulation - Cell Cycle Chaos
- Phases: G1 (growth), S (DNA synthesis), G2 (mitotic prep), M (mitosis). (📌 Mnemonic: Go Sally Go Make)
- Key Regulators:
- Cyclins (D, E, A, B) activate CDKs (e.g., CDK4/6, CDK2, CDK1).
- CDK Inhibitors (CKIs e.g., p16, p21, p27) halt progression.
- Checkpoints (Fail-safes):
- G1/S (Restriction Point): Governed by Rb, p53. Checks DNA integrity.
- G2/M: Ensures DNA replication complete, damage repaired.
- Spindle Assembly (M): Confirms correct chromosome attachment.
- Cancer = Dysregulation:
- Checkpoint failure (e.g., TP53, RB1 gene mutations) → uncontrolled proliferation.
- Oncogenes (e.g., Cyclin D) overexpressed; Tumor Suppressor Genes lost.
⭐ TP53, the "guardian of the genome," is mutated in over 50% of human cancers, causing G1/S checkpoint failure & genomic instability.
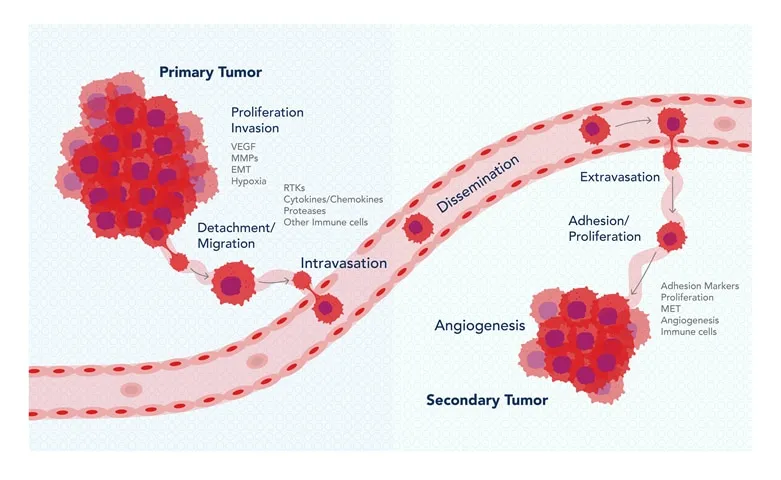
Metastasis & Angiogenesis - The Great Escape
- Metastasis: Cancer cells spread from primary to distant sites, forming secondary tumors.
- Routes: Lymphatic (common for carcinomas), Hematogenous (common for sarcomas), Transcoelomic.
- Common Sites: Lung, Liver, Bone, Brain (📌 LLBB: "Love Large Big Breakfast").
- Mechanism: "Seed and Soil" (Paget) - tumor cells ("seed") require a favorable microenvironment ("soil").
- Angiogenesis: Formation of new blood vessels; vital for tumor growth > 1-2 mm & metastasis.
- "Angiogenic Switch": Balance shifts to favor pro-angiogenic factors.
- Pro-angiogenic: VEGF, bFGF, PDGF.
- Anti-angiogenic: Thrombospondin-1, Angiostatin.
- 💡 Anti-VEGF therapy (e.g., Bevacizumab) is a key strategy.
⭐ VEGF is a primary driver of tumor angiogenesis.
High‑Yield Points - ⚡ Biggest Takeaways
- Oncogenes (e.g., RAS, MYC) drive cancer by promoting uncontrolled cell growth.
- Inactivation of tumor suppressor genes like p53 (genome guardian) and RB is critical for cancer development.
- Metastasis, the spread to distant sites, is the main cause of cancer mortality.
- Angiogenesis (new blood vessel formation, e.g., via VEGF) is essential for tumor growth.
- Cancer arises from a multi-step accumulation of genetic/epigenetic changes.
- Key hallmarks include evading apoptosis, limitless replication, and tissue invasion_._
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

