Prevention Strategies - Setting the Stage
- Patient Optimization:
- Nutrition, smoking cessation.
- Glycemic control: Target <180-200 mg/dL.
- MRSA decolonization if indicated.
- Antibiotic Prophylaxis: 📌 "TIME": Timing, Indication, Medication, End.
- Timing: Within 60 min before incision.
- Selection: Procedure-specific (based on common pathogens).
- Re-dosing: Long procedures (e.g., >2 half-lives, >4h), major blood loss (>1.5L).
- Discontinuation: Within 24h post-op.
⭐ Vancomycin infusion should start within 120 minutes before surgical incision due to longer infusion time.
- Skin & Hair:
- Skin Prep: Chlorhexidine-alcohol (CHG-Alc) preferred; apply from center to periphery.
- Hair Removal: Clip (not shave) immediately before surgery if hair interferes with surgery.
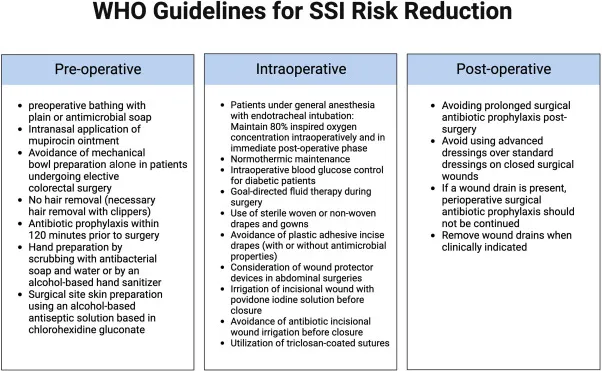

Prevention Strategies - Sterile Fortress
- OR Environment:
- Positive pressure ventilation (>15 ACH), HEPA filters for air purity.
- Limited OR traffic; strict surface cleaning & disinfection protocols.
- Surgical Team:
- Strict hand hygiene (surgical scrub). 📌 Mnemonic: "Clean Hands Save Lives."
- Sterile attire: gowns, double gloves (recommended), masks, caps/hoods.
- Surgical Technique (Aseptic & Atraumatic):
- Gentle tissue handling; minimize devitalized tissue, hematoma, and dead space.
- Judicious electrocautery use; select appropriate suture materials.
- Wound irrigation (e.g., normal saline); consider impervious wound protectors.
- Instrument Sterilization:
- Autoclaving: steam at 121°C (250°F) for 15-20 min at 15 psi. Verify with indicators.
- Sterile Field Maintenance:
- Unyielding maintenance of sterile drapes and instrument field integrity.
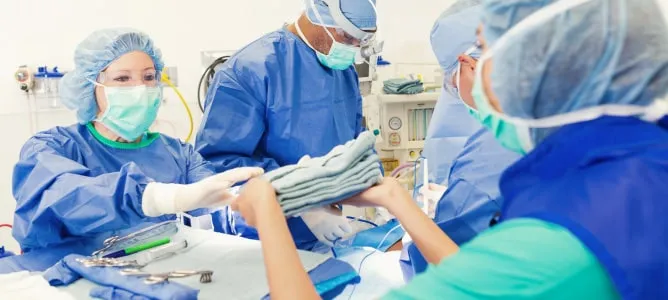
- Unyielding maintenance of sterile drapes and instrument field integrity.
⭐ Maintaining intraoperative normothermia (core temperature >36°C) is crucial; hypothermia significantly ↑ SSI risk.
Prevention Strategies - Healing Shield
- Wound Management:
- Maintain sterile dressing for 24-48h post-op.
- Strict hand hygiene before & after dressing changes.
- Choose dressing type based on wound characteristics (e.g., absorbent for exudative wounds).
- SSI Surveillance:
- Monitor for Surgical Site Infection (SSI) using CDC criteria: superficial, deep, organ/space.
- Signs: 📌 REEDA (Redness, Edema, Ecchymosis, Discharge, Approximation); also look for increasing pain, swelling, purulent discharge, or fever.
- Timing: Usually manifests within 30 days post-op, or within 1 year if an implant is present.
- Key Systemic Measures:
- Optimize glycemic control.
- Appropriate post-op antibiotic use: Discontinue prophylactic antibiotics within 24h for most surgeries.
⭐ Most SSIs manifest between the 5th and 10th post-operative day.
Prevention Strategies - Checklist Champions
- Care Bundles: Grouped evidence-based practices performed collectively to improve outcomes (e.g., SCIP measures).
- WHO Surgical Safety Checklist: Crucial for enhancing teamwork and communication.
- Sign In: Before anaesthesia induction (patient ID, site, consent).
- Time Out: Before skin incision (critical steps, antibiotics).
- Sign Out: Before patient leaves OR (specimens, equipment).
⭐ The WHO Surgical Safety Checklist has been shown to significantly reduce both morbidity and mortality.
- SSI Prevention Bundles: Specific sets of interventions for high-risk surgeries.
- Example: Colorectal Surgery Bundle
- Pre-op: Oral antibiotics + mechanical bowel prep.
- Intra-op: Appropriate antibiotic prophylaxis, maintain normothermia, strict glucose control (target < 200 mg/dL).
- Example: Colorectal Surgery Bundle
High‑Yield Points - ⚡ Biggest Takeaways
- Hand hygiene is the cornerstone of SSI prevention.
- Administer prophylactic antibiotics (e.g., Cefazolin) within 1 hour before surgical incision.
- Use chlorhexidine-alcohol for skin antisepsis; superior to povidone-iodine.
- Maintain intraoperative normothermia (core temp >36°C) to reduce SSI risk.
- Optimize perioperative glycemic control (target blood glucose <180-200 mg/dL).
- If hair removal is needed, use clippers immediately pre-surgery; avoid razors.
- Strict aseptic techniques and minimal OR traffic are vital to prevent SSIs.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

