OR Environment & Design - Fortress Against Bugs
- Zoning: Defines access & attire.
- Unrestricted: Street clothes.
- Semi-restricted: Scrubs, cap.
- Restricted (OR proper): Scrubs, cap, mask.
- Air Quality (Critical):
- Positive Pressure: 10-15 Pa higher than corridors.
- Air Changes: ≥20 ACH (total); ≥4 fresh air.
- HEPA Filters: Remove 99.97% of 0.3 µm particles.
- Laminar flow: For ultra-clean ORs (e.g., implants).
- Physical Environment:
- Temperature: 20-23°C.
- Humidity: 30-60%.
- Surfaces: Seamless, non-porous, easily cleanable.
- Lighting: Shadowless, adjustable.
- Traffic Control: Minimize movement.
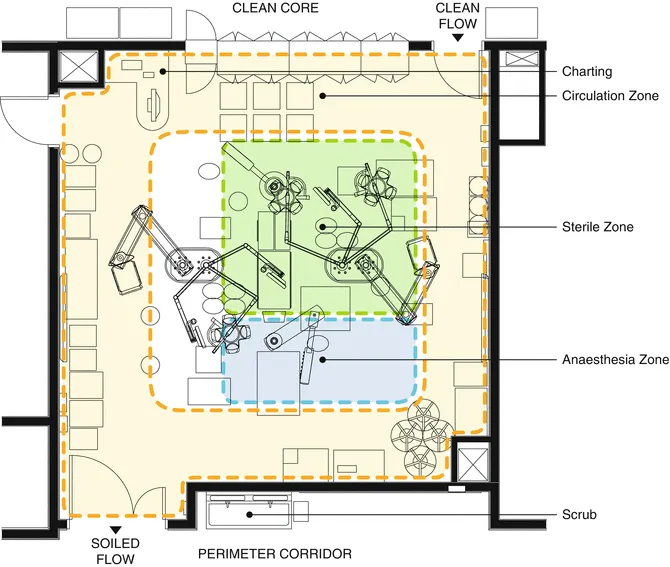
⭐ Positive pressure (10-15 Pa) in OR suite prevents entry of contaminated air from less clean adjacent areas.
Sterilization & Disinfection - The Germ Warfare
- Sterilization: Kills ALL microbes, including spores.
- Moist Heat (Autoclave): 121°C, 15 psi, 15-20 min. For instruments. 📌 Autoclave All Alive.
- Prions: 134°C, 3-5 min.
- Dry Heat (Hot Air Oven): 160°C for 2 hrs / 170°C for 1 hr. For glassware, oils.
- Chemical: ETO: heat-sensitive items (plastics); 2% Glutaraldehyde: >10 hrs (endoscopes); Plasma (H₂O₂).
- Radiation: Gamma rays for disposables.
- Moist Heat (Autoclave): 121°C, 15 psi, 15-20 min. For instruments. 📌 Autoclave All Alive.
- Disinfection: Kills most microbes; spores may survive.
- High-level: 2% Glutaraldehyde (<45 min), Peracetic acid.
- Intermediate: Alcohols (70%), Iodophors, Phenolics.
- Low-level: QACs (Quaternary Ammonium Compounds).
- Antisepsis: On living tissue (Povidone-iodine, Chlorhexidine).
- Monitoring Sterilization:
- Biological indicators (spore tests) = gold standard.
⭐ Geobacillus stearothermophilus spores are used to monitor steam autoclaves. oka
- Biological indicators (spore tests) = gold standard.
Surgical Team Protocol - The Sterile Sentinels
- Goal: Prevent SSI via strict team discipline & aseptic techniques.
- Hand Hygiene (Surgical Hand Antisepsis):
- Method: Timed scrub or counted strokes.
- Agents: Chlorhexidine (preferred), Povidone-Iodine.
- Duration: Initial scrub 3-5 min; subsequent 2-3 min.
- Surgical Attire:
- Clean, dedicated scrubs (non-sterile).
- Head cover (all hair & scalp covered).
- High-filtration surgical mask (fit-tested if N95).
- Shoe covers (optional, per hospital policy).
- Sterile Gowning & Gloving:
- Performed after hand antisepsis.
- Gown: Sterile, fluid-resistant.
- Gloves: Sterile; double-gloving recommended (esp. ortho/trauma).
- 📌 Gloves Over Gown cuff (closed gloving technique preferred).
- Maintaining Sterility in OR:
- Face sterile field; never turn back.
- Keep sterile items & hands above waist/table level.
- Minimize movement & talking near sterile field.
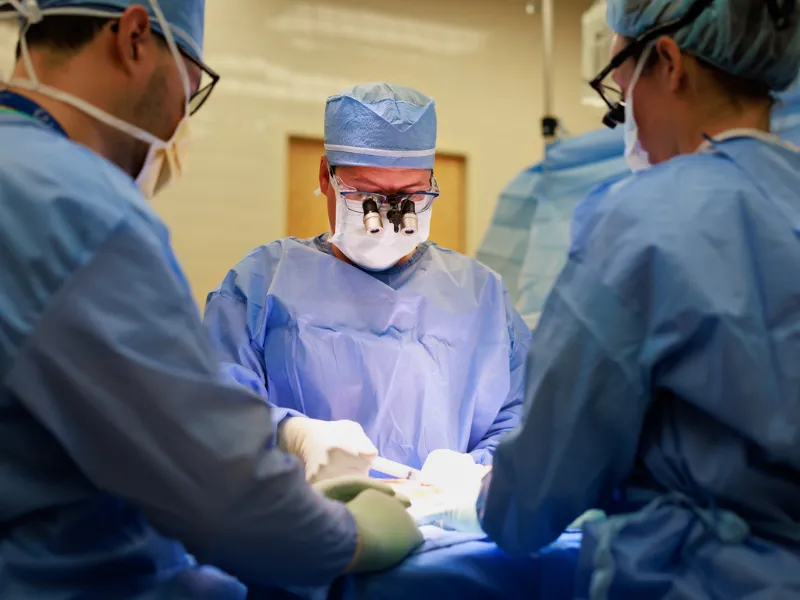
⭐ Movement of personnel should be minimized when sterile fields are open. Doors to the OR should be kept closed. Traffic in/out of the OR is a major source of airborne contaminants.
Patient & Intra-op Asepsis - Shielding the Host
- Patient Prep:
- Pre-op shower: Chlorhexidine Gluconate (CHG).
- Hair removal: Clipping (preferred over shaving) immediately pre-surgery if interfering.
- Skin antisepsis: Povidone-iodine or Chlorhexidine-alcohol; crucial drying time.
- Intra-op Measures:
- Sterile surgical drapes: Isolate operative field.
- Strict adherence to sterile field.
- Minimize OR traffic & door openings.
- Gentle tissue handling; wound irrigation.
⭐ Chlorhexidine-alcohol solutions for skin antisepsis demonstrate superior efficacy in reducing SSIs compared to povidone-iodine. oka
High‑Yield Points - ⚡ Biggest Takeaways
- OT ventilation: Maintain positive pressure with ≥15 air changes/hour (minimum 3 fresh).
- HEPA filters: Essential for removing 99.97% of airborne particles ≥0.3 µm.
- Surgical attire: Includes scrub suit, cap, mask; shoe covers are often used.
- Surgical hand antisepsis: Critical before gloving; use chlorhexidine or povidone-iodine.
- Prophylactic antibiotics: Administer IV within 60 minutes before surgical incision.
- Instrument sterilization: Autoclaving (steam sterilization) is the preferred method.
- OR traffic: Keep movement to a minimum to reduce airborne contamination.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

