Post-Anesthesia Care - Wake Up Call
- PACU (Post-Anesthesia Care Unit): Critical recovery area for patients immediately post-op.
- Aims: Stabilize vital signs, manage pain & PONV (Postoperative Nausea and Vomiting), ensure airway patency, detect early complications.
- Patient Reception & Initial Assessment:
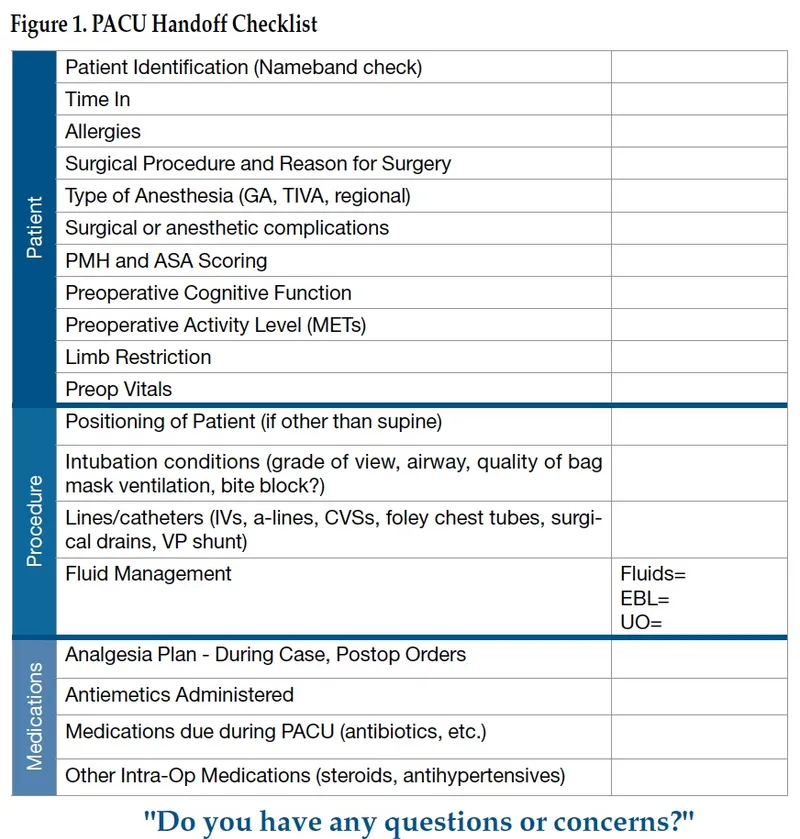
- Handover: Structured (e.g., SBAR) from OR team.
- Connect monitors: ECG, SpO₂, NIBP, Temp.
- Rapid ABCDE assessment: Airway, Breathing, Circulation (inc. surgical site), Disability (LOC), Exposure.
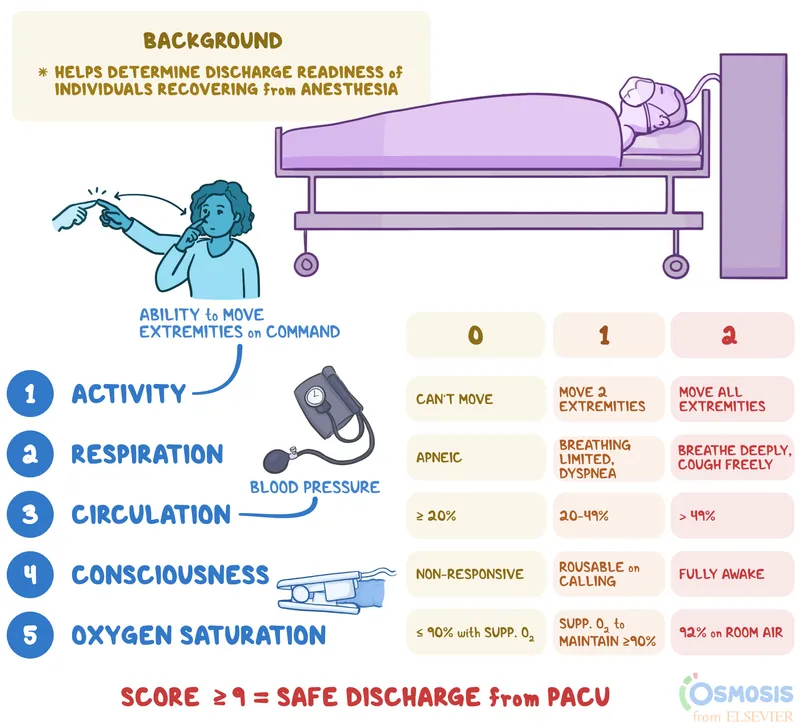
- Baseline vitals, pain score, Aldrete score.
⭐ The Aldrete score is pivotal for assessing post-anesthesia recovery; a score of ≥9 is commonly required before PACU discharge.
Post-Anesthesia Care - Complication Central
PACU: manage immediate adverse events. Early recognition & intervention are vital.
- Key PACU Issues & Actions:
- Hypoxemia: SpO2 <90%. Causes: Airway obstruction, hypoventilation. Mgmt: ↑FiO2, airway support.
- Hypotension: SBP <90 mmHg or >20% ↓ from baseline. Causes: Hypovolemia, vasodilation. Mgmt: Fluids, vasopressors.
- Hypertension: SBP >180 mmHg or >20% ↑ from baseline. Causes: Pain, anxiety, hypoxia. Mgmt: Analgesia, antihypertensives.
- PONV (Postoperative Nausea & Vomiting): Mgmt: Ondansetron 4mg IV, dexamethasone.
- Pain: Mgmt: Multimodal analgesia (opioids, NSAIDs, regional techniques).
- Shivering/Hypothermia: Core temp <36°C. Mgmt: Forced air warming, meperidine 12.5-25mg IV.
- Delayed Emergence: Causes: Residual drugs, metabolic imbalance, neurologic event. Mgmt: Supportive, rule out causes, reversal agents (naloxone, flumazenil if indicated).
⭐ Hypoxemia (SpO2 <90%) is a critical early PACU complication, often due to airway obstruction or hypoventilation.
Post-Anesthesia Care - Monitor & Medicate
- Key Monitoring (PACU):
- Vitals: HR, BP (MAP > 65 mmHg), RR, SpO2 (> 94%), Temp. Continuous ECG.
- Airway: Patency, breathing pattern, auscultation.
- Neurology: LOC (Aldrete score), pain (VAS/NRS).
- Renal: Urine output > 0.5 mL/kg/hr.
- Surgical: Site (bleeding, hematoma), drains.
- PONV: Assess frequency & severity.
- Essential Medications:
- Oxygen: Supplemental O2 to maintain SpO2.
- Analgesia: Multimodal - Opioids (e.g., Fentanyl IV), NSAIDs, Paracetamol.
- Antiemetics: Ondansetron 4-8 mg IV, Dexamethasone.
- Fluids: IV crystalloids, guided by hemodynamics & losses.
- Shivering:
⭐ Shivering increases oxygen consumption by up to 400-500%; active warming and drugs like pethidine are key.
- Pethidine 12.5-25 mg IV, warm blankets, forced-air warmers.
Post-Anesthesia Care - Road to Recovery Ward
- Goal: Safe PACU discharge. Patient must be stable.
- Key Discharge Criteria:
- Vitals: Stable (BP, HR, RR, Temp); SpO2 >92% (or baseline).
- Pain: Controlled (VAS <4).
- Nausea/Vomiting (N/V): Minimal/treated.
- Consciousness: Awake, oriented (or baseline).
- Surgical Site: No active bleeding/hematoma.
- Scoring Systems Aid Decision:
- Modified Aldrete Score: ≥9 (activity, respiration, circulation, consciousness, O2 sat).
- PADSS (ambulatory): ≥9 (vitals, activity, N/V, pain, bleeding).
⭐ Patients must demonstrate stable vital signs, adequate pain control, and minimal nausea/vomiting, often guided by a score like Modified Aldrete (≥9) or PADSS (≥9 for ambulatory), before PACU discharge.
High‑Yield Points - ⚡ Biggest Takeaways
- Aldrete score (≥9) guides PACU discharge; assesses activity, respiration, circulation, consciousness, O2 saturation.
- Commonest PACU issues: PONV, hypoxemia, hypotension, pain.
- Manage postoperative shivering with warming; meperidine for severe cases.
- Airway obstruction (e.g., tongue fall, laryngospasm) is critical; requires immediate intervention.
- Delayed emergence may indicate residual anesthesia, metabolic issues, or neurological injury.
- Prioritize pain control using multimodal analgesia.
- Monitor urine output (target >0.5 mL/kg/hr) for adequate perfusion_
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

