Cardiovascular Comorbidities - Heart Matters Most
- Risk Stratification:
- Revised Cardiac Risk Index (RCRI) for Major Adverse Cardiac Events (MACE):
- Components: High-risk surgery, Hx Ischemic Heart Disease (IHD), Hx Congestive Heart Failure (CHF), Hx Cerebrovascular Accident (CVA)/Transient Ischemic Attack (TIA), Insulin-dependent Diabetes Mellitus, Preoperative Creatinine >2 mg/dL.
- Score 0: 0.4% MACE; 1: 0.9%; 2: 6.6%; ≥3: 11%.
- Revised Cardiac Risk Index (RCRI) for Major Adverse Cardiac Events (MACE):
- Hypertension (HTN):
- Goal: BP <140/90 mmHg.
- Delay elective surgery if BP >180/110 mmHg.
- Continue β-blockers. Consider holding ACE inhibitors/ARBs on surgery day (risk of hypotension).
- Ischemic Heart Disease (IHD):
- Post-Myocardial Infarction (MI): Delay elective surgery >60 days.
- Post-Percutaneous Coronary Intervention (PCI): Bare Metal Stent (BMS) 4-6 weeks; Drug-Eluting Stent (DES) 6-12 months.
- Aspirin: Continue for high CV risk; stop 7 days prior if high bleed risk surgery.
- Heart Failure (HF):
- Optimize volume status & medical therapy. Ejection Fraction (EF) <35% indicates ↑ risk.
- Valvular Heart Disease:
- Severe Aortic Stenosis (AS): Aortic Valve Area (AVA) <1 cm², mean gradient >40 mmHg. High risk; consider Aortic Valve Replacement (AVR) pre-op.
⭐ Continuation of beta-blockers perioperatively is crucial for patients on chronic therapy.
Respiratory & Diabetic Care - Lungs & Glucose Go-Tos
Respiratory - Preoperative:
- Smoking cessation: 4-8 weeks prior.
- PFTs for high-risk (e.g., FEV1 < 50%).
- Asthma: Continue meds; pre-op steroids if FEV1 < 80% or recent exacerbation.
- COPD: Optimize bronchodilators.
Respiratory - Postoperative:
- Incentive spirometry, deep breathing.
- Early mobilization, adequate analgesia.

Diabetes Mellitus - Perioperative:
- Goal: HbA1c < 8%.
- Medications:
- Stop Metformin 24-48h prior.
- Hold other oral hypoglycemics (OHAs) day of surgery.
- Adjust insulin: Continue basal, hold/reduce prandial.
- Monitoring: Frequent blood glucose (BG).
⭐ Target perioperative BG: 140-180 mg/dL. IV insulin if BG consistently > 180 mg/dL.
📌 Lungs: Stop smoking, PFTs, Optimize meds, Post-op physio. 📌 Glucose: HbA1c <8%, Hold OHAs (Metformin early), Insulin adjust, Target 140-180 mg/dL.
Renal & Hematologic Management - Kidney & Clotting Care
- Renal Function Assessment & Care:
- Calculate eGFR pre-op. Cockcroft-Gault: $CrCl = \frac{((140 - Age) \times Wt_{kg} \times [0.85 \text{ if female}])}{(72 \times SCr_{mg/dL})}$.
- Adjust drug dosages if eGFR < 60 mL/min/1.73m².
- Maintain euvolemia; avoid nephrotoxic agents to prevent AKI.
- Hematologic Considerations:
- Anemia: Consider transfusion if Hb < 7-8 g/dL, or if patient is symptomatic.
- Anticoagulation Management:
- Warfarin: Stop 5 days pre-op. Target INR < 1.5.
- LMWH: Stop 12-24h (prophylactic dose) or 24-48h (therapeutic dose) pre-op.
- DOACs: Stop 1-5 days pre-op, depending on specific agent and renal function.
- Thrombocytopenia: Aim for platelet count > 50,000/μL for most surgeries; > 100,000/μL for neurosurgery/ophthalmic surgery.
⭐ For elective surgery, Warfarin is typically stopped 5 days prior and bridged with LMWH if high thrombotic risk.

Hepatic & Other Endocrine - Glands & Gut Guards
- Hepatic Dysfunction:
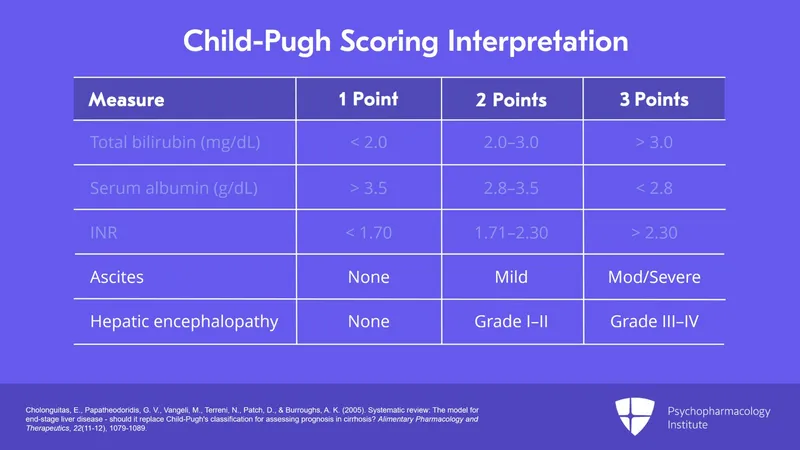
- Assess severity: Child-Pugh (Bilirubin, Albumin, INR, Ascites, Encephalopathy), MELD (Bilirubin, INR, Creatinine).
- Optimize: Correct coagulopathy (Vit K, FFP), manage ascites, treat encephalopathy.
- Delay elective surgery if acute hepatitis or decompensation.
- Thyroid Disorders:
- Hypothyroid: Continue levothyroxine. Severe (myxedema) - postpone elective surgery.
- Hyperthyroid: Achieve euthyroid state pre-op (antithyroid drugs, β-blockers). Risk of thyroid storm.
- Adrenal Gland:
- Adrenal Insufficiency: 📌 Stress dose steroids.
- Minor surgery: Hydrocortisone 25mg IV pre-op.
- Moderate: Hydrocortisone 50-75mg IV pre-op, then taper.
- Major: Hydrocortisone 100-150mg IV pre-op, then taper.
- Pheochromocytoma: Pre-op α-blockade (e.g., phenoxybenzamine) then β-blockade.
- Adrenal Insufficiency: 📌 Stress dose steroids.
⭐ Patients on chronic steroids (e.g., >5mg prednisone daily for >3 weeks, or equivalent) require perioperative stress dose steroids.
High‑Yield Points - ⚡ Biggest Takeaways
- Continue beta-blockers; hold ACEi/ARBs on surgery day.
- Target perioperative glucose 140-180 mg/dL for diabetics.
- Delay elective surgery: 4-6 weeks post-MI, 6 months post-Drug Eluting Stent.
- Smoking cessation ≥4-8 weeks preoperatively significantly reduces pulmonary risk.
- Bridge anticoagulation (e.g., warfarin to heparin) for high-risk thromboembolic patients.
- Optimize severe COPD/asthma; ensure euthyroid state before thyroid surgery.
- Child-Pugh score assesses risk in liver disease; correct coagulopathy_
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

