Drain Basics - Why We Drain
- Primary Goals:
- Eliminate existing collections: pus, blood, serous fluid, gas.
- Prevent potential fluid/air accumulation in dead spaces.
- Monitor output for early detection of leaks (e.g., anastomotic, biliary).
- Characterize drained fluid (e.g., chyle, CSF, pancreatic).
- Common Scenarios:
- Abscess drainage.
- Post-surgery: high risk of seroma/hematoma.
- Monitoring anastomotic integrity.
- Contaminated or extensive surgical fields.

⭐ Prophylactic drains aim to reduce surgical site infections (SSIs) by eliminating collections that serve as culture media for bacteria and can help obliterate dead space, reducing infection risk and promoting healing by apposition of tissues.
Drain Types - Tube Toolkit
- Key Categories: Open/Closed, Passive/Active (Suction).
- Drain Comparison:
| Type | System | Suction | Examples | Mechanism / Key Use |
|---|---|---|---|---|
| Penrose | Open | Passive | - | Capillary action; Superficial wounds, abscesses. ⚠️ High infection risk. |
| Corrugated | Open | Passive | Rubber/Plastic sheet | Channels fluid; Similar to Penrose. |
| T-tube | Closed | Passive | Common Bile Duct | Gravity drainage (e.g., bile). |
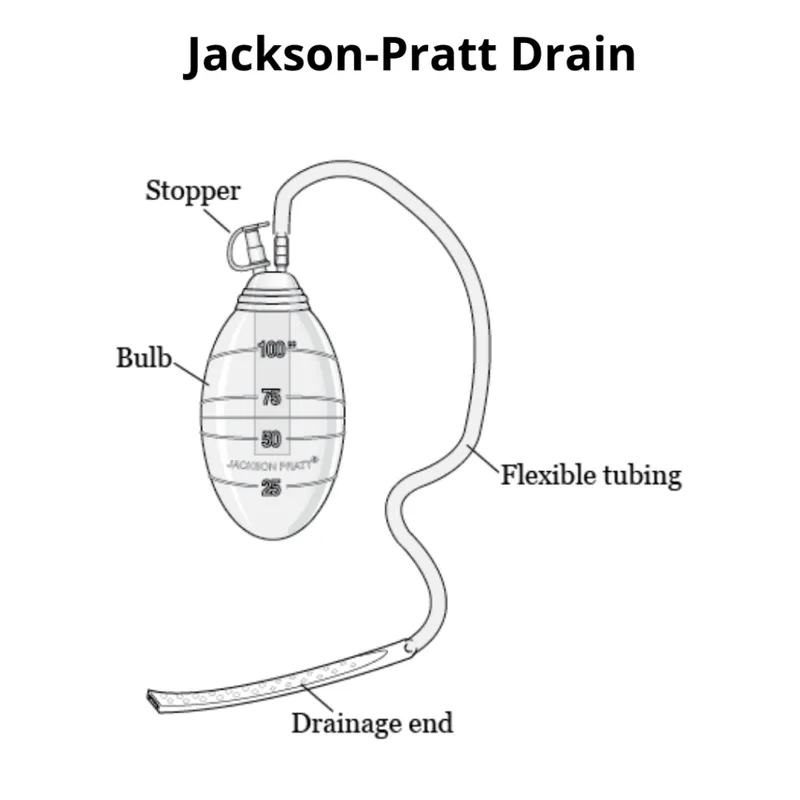
| Jackson-Pratt (JP) | Closed | Active | Bulb ("grenade") | Low-pressure suction; Prevents seroma (e.g., mastectomy). |
| Blake | Closed | Active | Fluted silicone channels | Low-pressure suction; Similar to JP, less tissue trauma. |
| Hemovac/Redivac | Closed | Active | Spring-loaded reservoir | High-pressure suction; Large volume drainage (ortho). |
⭐ Exam Favourite: Jackson-Pratt (JP) drains utilize gentle, active, closed suction via a compressible bulb, making them effective for minimizing dead space and evacuating fluid in areas like post-mastectomy or thyroidectomy sites.
Drain Care - Watch & Ward
- Site Care (Aseptic):
- Daily inspect: Redness, swelling, tenderness, leak.
- Dressing: Keep clean, dry; sterile change PRN.
- Secure drain: Prevent kinking or dislodgement.
- Output Monitoring (Record QCC):
- Quantity: Volume/24h (aim < 30-50 mL for removal).
- Color: Serous, serosanguinous, purulent, bilious, chylous.
- Consistency: Thin, thick. Report abrupt changes.
- Patency & Function:
- Ensure no kinks, dependent loops.
- Milking/stripping: Only if specifically indicated.
- Verify suction for active drains.
- Troubleshooting Flow:
⭐ High-Yield: Sudden ↓ drain output with persistent local/systemic signs often indicates blockage, not true fluid resolution.
Drain Issues - Pull & Problems
-
Drain Pull Criteria:
- Output: < 25-50 mL/day (or < 0.5-1 mL/kg/day).
- Fluid: Serous, non-purulent.
- Clinical: Improving, afebrile, no local infection.
- Chest tube: No air leak, < 200 mL/24h, lung expanded.
⭐ T-tube (biliary): Remove 2-6 wks post-cholangiogram (no leak, patent duct).
-
Removal How-To:
- Aseptic. Gentle, steady pull.
- Chest tube: Valsalva on removal.
- Occlusive dressing.
-
Common Issues & Fixes:
- Blockage: (Kinks, clots) → Milk, gentle flush.
- Infection: (Local/systemic) → Culture, antibiotics, ?remove.
- Pain: Analgesia, check position.
- Displacement: Re-secure, confirm placement.
- Erosion: (Vessel/viscus) → Rare; urgent surgery.
- High Output: Monitor fluid/electrolytes.
High‑Yield Points - ⚡ Biggest Takeaways
- Drains: Eliminate dead space, prevent fluid collections (hematoma, seroma, pus), monitor leaks.
- Closed suction drains (e.g., Jackson-Pratt) preferred over open drains (e.g., Penrose) for lower infection risk.
- Drain removal: Guided by low output (< 30-50 mL/24h), serous fluid, not fixed duration.
- Complications: Infection (most common), blockage, pain, erosion into structures.
- Prophylactic drains in clean surgery: Often avoided; may ↑ infection risk.
- T-tubes (CBD): Removed after cholangiogram confirms patency (usually 10-14 days).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

