Flap Fundamentals - Skin Deep Dive
- Flap: Tissue segment with its intrinsic blood supply, moved from a donor to a recipient site.
- Pedicle: Base of the flap containing its nourishing blood vessels.
- Donor Site: Area from which the flap is harvested.
- Recipient Site: Defect area where the flap is transferred.
- Indications: Cover exposed vital structures (bone, tendon, nerves), reconstruct complex defects, provide padding, restore function or sensation.
⭐ A flap is tissue moved from a donor to recipient site, maintaining its own blood supply.
Flap Classification - Name That Flap!
| Flap Type | Blood Supply Description | Example(s) |
|---|---|---|
| Random Pattern | Dermal/subdermal plexus, no named vessel | Local skin flaps |
| Axial: Direct Cutaneous | Named direct cutaneous artery | Groin flap (SCIA) |
| Axial: Fasciocutaneous | Named artery via fascial perforators | Anterolateral thigh (ALT) |
| Axial: Musculocutaneous | Named artery via muscular perforators | TRAM, Latissimus Dorsi |
| Axial: Septocutaneous | Named artery via septal perforators | Radial forearm flap |
| Free Flap | Detached pedicle, microvascular anastomosis required | Any of above as free tissue |
- Cutaneous: Skin, subcutaneous tissue.
- Fasciocutaneous: Skin, subcutaneous tissue, fascia.
- Myocutaneous: Skin, subcutaneous tissue, muscle.
- Osteocutaneous: Skin, subcutaneous tissue, bone (± muscle/fascia).
By Method of Transfer:
- Advancement: Slides directly forward.
- Rotation: Pivots around a fixed point.
- Transposition: Pivots over intervening intact tissue.
- Interpolation: Tunneled under/over a tissue bridge to a nearby defect.
- Free: Detached from original blood supply and reanastomosed at recipient site.

⭐ Free flaps require microvascular anastomosis for revascularization and offer the most versatility in reconstruction.
Flap Physiology - Blood Flow Glow
- Angiosomes (Taylor): 3D tissue units supplied by a source artery; interconnected via choke vessels. Key for flap design.
- Delay Phenomenon: Incising flap borders 1-2 weeks pre-transfer.
- Mechanism: Induces ischemia, dilates choke vessels, ↑ neovascularization.
- Benefit: Conditions flap, ↑ survival.
- Factors Affecting Survival:
- Systemic: Smoking, diabetes.
- Local: Infection, radiation.
- Technical: Tension, pedicle kinking.
- Ischemia-Reperfusion Injury: Damage post-reperfusion (free radicals). Critical ischemia: Muscle ~4-6 hrs; Skin ~8-12 hrs.
⭐ The delay phenomenon, typically achieved by incising flap borders 1-2 weeks before transfer, conditions a flap to ischemia and significantly improves its survival rate.
Flap Design & Complications - Stitch & Glitch
- Design Principles:
- Random flaps: Max $L:W \approx 1.5:1$ (site-dependent).
- Axial flaps: Aligned with a named artery.
- Tension-free closure: Essential.
- Free flaps: Utilize reverse planning.
- Flap Monitoring:
- Clinical signs: Color, temperature, capillary refill (<3s), turgor.
- Handheld Doppler.
- 📌 Compromise Signs:
- Arterial: Pale, Cool, ↓CR.
- Venous: Congested, Dusky, ↑CR.
- Complications & Management:
- Common: Necrosis (arterial/venous; partial/total), hematoma, seroma, infection.
- Principles: Optimize patient, local wound care, debridement, antibiotics.
- Donor Site:
- Aim for minimal morbidity.
- Manage: Primary closure or skin graft.
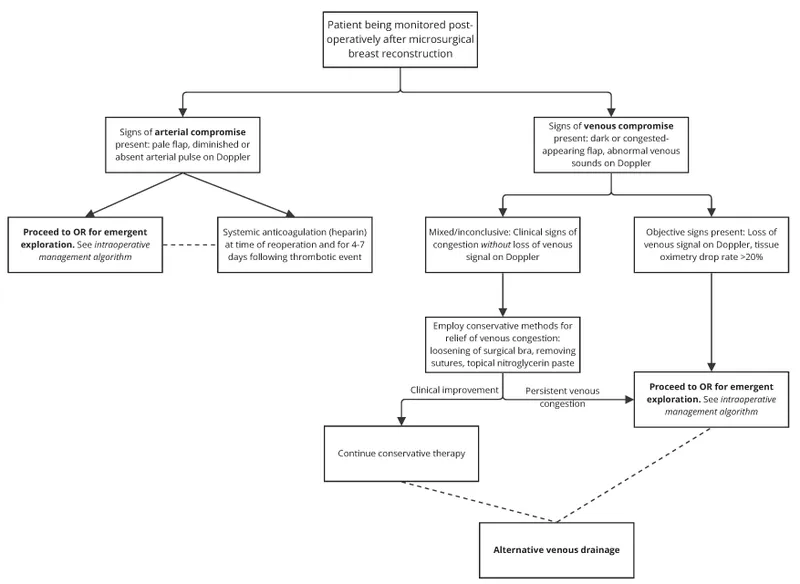
⭐ Venous congestion is often a more critical and earlier indicator of impending flap failure than arterial insufficiency, requiring prompt intervention.
High‑Yield Points - ⚡ Biggest Takeaways
- Flap survival hinges on adequate blood supply: arterial inflow, venous outflow.
- Delay phenomenon conditions flaps, improving vascularity and survival.
- Random flaps rely on dermal plexus; axial flaps include a named artery.
- Pedicled flaps maintain original blood supply; free flaps need microvascular anastomosis.
- Venous thrombosis is the commonest cause of flap failure.
- Key flaps: Latissimus Dorsi (muscle), Radial Forearm (fasciocutaneous), DIEP (perforator).
- Monitor viability: color, capillary refill, temperature, Doppler signals antegrade and retrograde flow in flap vessels after surgery to ensure flap survival and detect complications early for timely intervention and salvage of flap if compromised by thrombosis or kinking of vessels or hematoma formation under flap compressing vessels or infection leading to flap necrosis or failure of flap to take up at recipient site due to poor vascularity of recipient site or technical error during surgery or patient factors like smoking or diabetes or peripheral vascular disease or radiation therapy to recipient site or systemic illness or medication like vasopressors or anticoagulants or immunosuppressants or chemotherapy or radiotherapy to donor site or previous surgery at donor site or trauma to donor site or infection at donor site or poor nutritional status of patient or obesity or advanced age of patient or co-morbidities of patient like hypertension or cardiac disease or renal disease or liver disease or respiratory disease or hematological disorder or autoimmune disease or connective tissue disorder or psychiatric illness or substance abuse or non-compliance of patient with post-operative instructions or follow-up care or rehabilitation program or physiotherapy or occupational therapy or speech therapy or psychological counseling or social support or financial assistance or vocational training or job placement or home care or nursing care or palliative care or hospice care or end-of-life care or organ donation or tissue donation or blood donation or stem cell donation or bone marrow donation or corneal donation or skin donation or body donation for medical research or education or anatomical dissection or plastination or museum display or art exhibition or public awareness or health promotion or disease prevention or screening test or diagnostic test or prognostic test or therapeutic intervention or surgical procedure or medical device or drug therapy or vaccine or gene therapy or cell therapy or immunotherapy or radiotherapy or chemotherapy or hormone therapy or targeted therapy or palliative therapy or supportive care or complementary medicine or alternative medicine or traditional medicine or integrative medicine or holistic medicine or mind-body medicine or energy medicine or spiritual healing or faith healing or prayer or meditation or yoga or tai chi or qigong or reiki or acupuncture or acupressure or massage or aromatherapy or herbal medicine or homeopathy or naturopathy or ayurveda or unani or siddha or chiropractic or osteopathy or reflexology or hydrotherapy or balneotherapy or thalassotherapy or climatotherapy or heliotherapy or phototherapy or chromotherapy or music therapy or art therapy or dance therapy or drama therapy or play therapy or animal-assisted therapy or pet therapy or equine therapy or dolphin therapy or hippotherapy or horticultural therapy or wilderness therapy or adventure therapy or ecotherapy or nature therapy or forest bathing or shinrin-yoku or earthing or grounding or biofeedback or neurofeedback or hypnosis or guided imagery or visualization or progressive muscle relaxation or autogenic training or breathing exercises or mindfulness or cognitive behavioral therapy or dialectical behavior therapy or acceptance and commitment therapy or interpersonal therapy or psychodynamic therapy or psychoanalysis or group therapy or family therapy or couples therapy or marital therapy or sex therapy or counseling or coaching or mentoring or peer support or self-help group or online support group or support network or social network or community resources or public services or government programs or non-governmental organizations or charitable foundations or voluntary associations or patient advocacy groups or consumer organizations or professional societies or academic institutions or research centers or healthcare facilities or hospitals or clinics or pharmacies or laboratories or diagnostic centers or imaging centers or rehabilitation centers or nursing homes or hospices or home health agencies or emergency medical services or ambulance services or air ambulance services or poison control centers or blood banks or organ procurement organizations or tissue banks or eye banks or sperm banks or milk banks or cord blood banks or stem cell banks or bone marrow registries or clinical trial registries or research ethics committees or institutional review boards or data safety monitoring boards or regulatory agencies or health authorities or ministries of health or departments of health or public health agencies or centers for disease control and prevention or world health organization or pan american health organization or unicef or unaids or global fund or gavi or gates foundation or wellcome trust or rockefeller foundation or ford foundation or carnegie corporation or macarthur foundation or kaiser family foundation or commonwealth fund or robert wood johnson foundation or pew charitable trusts or an
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

