Body Contouring Basics - Shaping the Silhouette
- Aim: Surgically reshape body contours by removing excess skin and stubborn fat deposits, typically after massive weight loss (MWL) or due to aging/genetics. Addresses functional (e.g., rashes, mobility) and aesthetic concerns.
- Key Candidacy Factors:
- Weight stability: Maintained for 6-18 months.
- BMI: Ideally < 30 kg/m²; up to 35 kg/m² may be considered.
- Nutrition: Adequate (e.g., Albumin > 3.0-3.5 g/dL, Hb > 10 g/dL).
- Smoking: Cessation 4-8 weeks pre- and post-operatively is crucial.
- Realistic expectations & psychological stability.
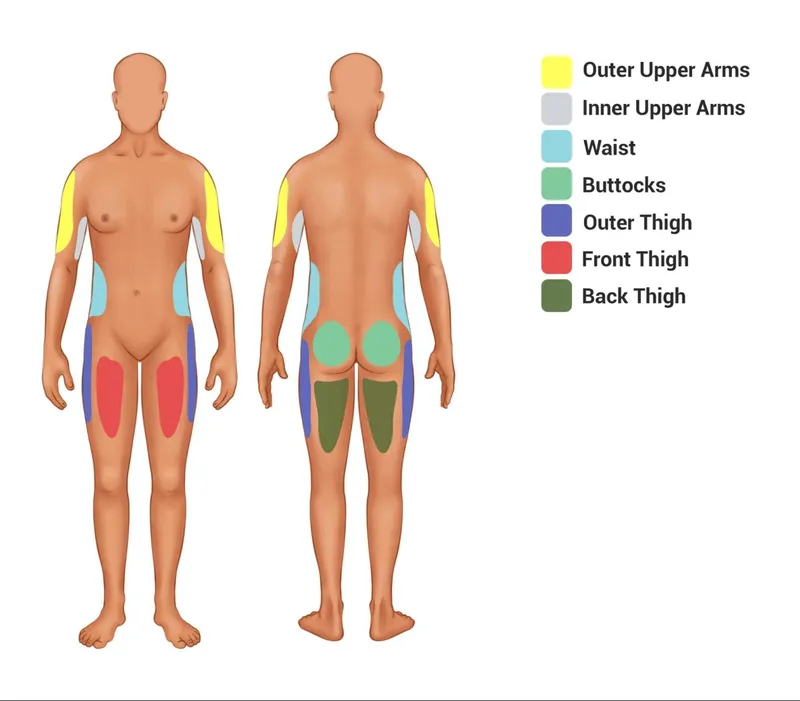
- Common Procedures: Abdominoplasty (tummy tuck), brachioplasty (arm lift), thighplasty (thigh lift), mastopexy (breast lift).
⭐ Ideal patient: Stable weight, realistic expectations, non-smoker, BMI < 30 kg/m² for many procedures.
Liposuction Lowdown - Fat Farewell
-
Tumescent Technique:
- Fluid: Lidocaine, Epinephrine, Saline (📌 'LES' is More for safety).
- Max lidocaine: 7mg/kg with epinephrine.
- Benefits: ↓ blood loss, local anesthesia, vasoconstriction.
-
Liposuction Modalities:
Type Mechanism Adv. Disadv. Uses SAL Manual, vacuum Standard, versatile Surgeon fatigue General UAL Ultrasonic emulsification Fibrous areas, ↓ blood loss Thermal risk, learning curve Gynecomastia, fibrous, revisions PAL Vibrating cannula ↓ Fatigue, faster, large vol. Vibration Large vol., fibrous LAL Laser: melts fat, tightens skin Skin tightening, small areas Burn risk, small vol. Small deposits, face/neck, laxity -
Key Considerations:
- Large Volume Liposuction (LVL): > 5000 mL total aspirate; requires careful fluid management.
- Zones of Adherence: Preserve for natural contour (e.g., gluteal crease).

⭐ Safest maximum aspirate for outpatient liposuction: 5L total aspirate (fat + fluid).
Excisions & Elegance - Tailoring Tissues
Surgical removal of excess skin and fat (dermolipectomy) to reshape and tone body regions. Common after massive weight loss (MWL) or due to aging.
Comparison: Major Excisional Lifts
| Lift | Indications | Key Anatomical Structures | Common Incision Types | Common Complications |
|---|---|---|---|---|
| Abdominoplasty | Excess abdominal skin/fat, rectus diastasis | Scarpa's fascia, rectus m., umbilicus | Low transverse, periumbilical, fleur-de-lis | Seroma, hematoma, VTE, skin necrosis |
| Brachioplasty | Upper arm skin/fat laxity ("bat wings") | Brachial fascia, med. brachial cut. n. | Medial arm (linear/T-scar) | Hypertrophic scarring, nerve injury, edema |
| Thighplasty | Medial/anterior thigh skin/fat laxity | Fascia lata, great saphenous v. | Medial thigh, groin crease, vertical | Prominent scars, lymphedema, dehiscence |
Abdominoplasty Type Selection:
⭐ Preservation of Scarpa's fascia is crucial for lymphatic drainage and reducing seroma in abdominoplasty.
Healing & Hazards - The Recovery Roadmap
- Key Recovery Aspects:
- Compression garments: 4-6 weeks.
- Drains: Remove when <30ml/24h.
- Early ambulation. Smoking cessation vital.
- DVT Prophylaxis: 📌 'COMPRESS' (Compression, Mobilization, Prophylaxis (LMWH), Risk Assessment, Education, Stop smoking, Sequential devices).
- Common Complications:
| Complication | Prevention | Key Management |
|---|---|---|
| Seroma | Drains, compression | Aspiration, sclerotherapy, surgery |
| Hematoma | Hemostasis, BP control | Evacuation (large), observation (small) |
| DVT/PE | COMPRESS protocol adherence | Anticoagulation |
| Infection | Asepsis, prophylactic antibiotics (e.g., Cefazolin 1-2g IV) | Antibiotics, drainage, debridement |
| Skin Necrosis | Preserve blood supply, avoid tension, no smoking | Debridement, wound care, revision |

- Post-bariatric: Optimize nutrition; higher wound complication risk.
High‑Yield Points - ⚡ Biggest Takeaways
- Patient selection is crucial: stable weight, BMI <30-35 kg/m², and realistic expectations are paramount.
- Liposuction (SAL, UAL, PAL) targets localized adiposity; the tumescent technique minimizes blood loss.
- Abdominoplasty corrects skin laxity and diastasis recti; it is not primarily a weight loss procedure.
- Massive Weight Loss (MWL) patients often require staged excisional procedures like body lifts or brachioplasty.
- Common complications include seroma, hematoma, skin necrosis, and contour irregularities.
- DVT prophylaxis is vital; screen for Body Dysmorphic Disorder (BDD) as a contraindication to aesthetic procedures.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

