Pediatric Trauma Overview - Little Patients, Unique Risks
- Unique Vulnerabilities:
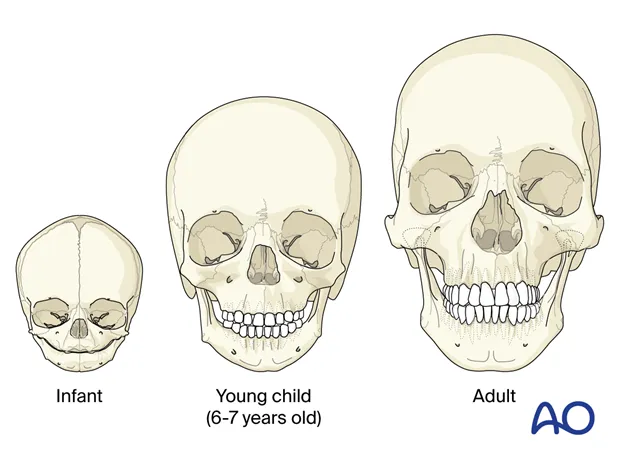
- Anatomy: Large head, pliable bones, compliant chest wall.
- Physiology: ↑ Surface Area to Volume ratio (hypothermia risk), single kidney often unprotected, ↑ metabolic rate (rapid O₂ desaturation).
- Epidemiology (Leading death cause >1 yr):
- Mechanisms: Falls (commonest), Motor Vehicle Accidents (MVA, highest mortality), pedestrian, bicycle, Non-Accidental Trauma (NAT).
- Trauma Patterns:
- Blunt > Penetrating.
- Polytrauma is the rule, not the exception.
- Key Principle:
- Tri-modal death distribution underscores that prevention is key.
⭐ The 'Rule of Nines' for burns is modified in children (Lund-Browder chart is more accurate) due to different body proportions.
Primary Survey & Resuscitation - Kid-Sized ATLS
- Airway: Smaller, anterior larynx; narrowest at cricoid (uncuffed ETT <8yrs). Sniffing position. RSI considerations.
- Breathing: ↑RR, diaphragmatic. Pliable chest (occult pneumo/hemothorax). Needle thoracostomy: 2nd ICS MCL or 4th/5th ICS AAL.
- Circulation: Tachycardia = early shock. Hypotension = LATE. BP formula: $(Age \text{ in yrs} \times 2) + 70$ (systolic lower limit). Fluid: 20ml/kg crystalloid bolus (up to 3x), then 10-20ml/kg PRBCs. IO access vital. Broselow tape.

- Disability: Pediatric GCS (or AVPU). Glucose check (hypoglycemia risk).

- Exposure: Prevent hypothermia (high risk, large surface area).
⭐ In children, hypotension is a late sign of shock; tachycardia, altered mental status, and poor peripheral perfusion are earlier indicators.
Specific Injuries Part 1 - Head, Chest & Abdomen
- Head Trauma:
- Most common cause of pediatric trauma death.
- GCS <8: intubate.
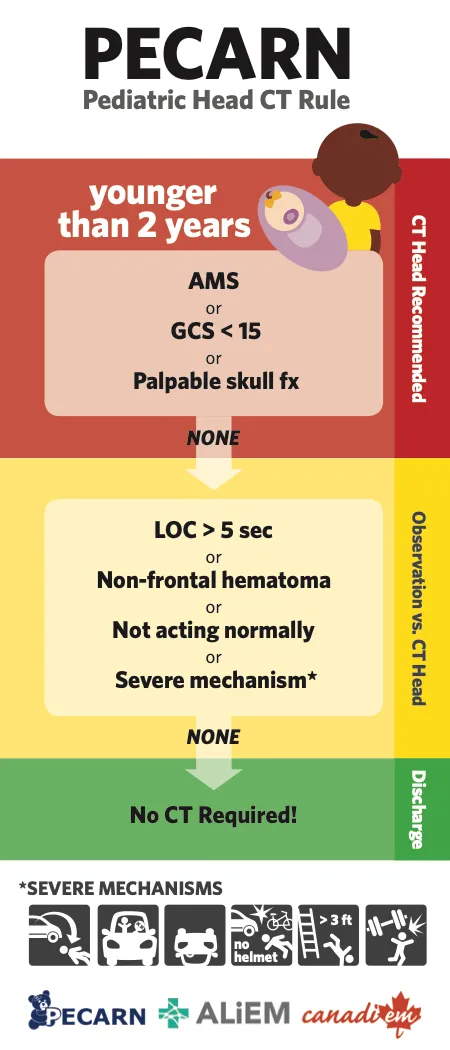
- PECARN for CT use in minor head trauma.
- Diffuse Axonal Injury (DAI) common.
- Cushing's triad (bradycardia, hypertension, irregular respirations): late sign.
- Chest Trauma:
- Rib fractures rare; indicate severe force.
- Multiple in infant: consider Non-Accidental Trauma (NAT).
- Pulmonary contusion: most common chest injury.
- Tension pneumothorax: clinical diagnosis, immediate needle decompression.
- Rib fractures rare; indicate severe force.
- Abdominal Trauma:
- Spleen (most common), liver, kidney.
- Non-Operative Management (NOM) highly successful.
- Specific injuries: Duodenal hematoma (handlebar injury), pancreatic injury.
- FAST scan for initial assessment.
- ⭐
The presence of a 'seatbelt sign' (abdominal wall bruising) after an MVA significantly increases suspicion for intra-abdominal injuries, particularly hollow viscus perforation and lumbar spine fractures.
Specific Injuries Part 2 - MSK & NAT Alerts
- MSK Trauma:
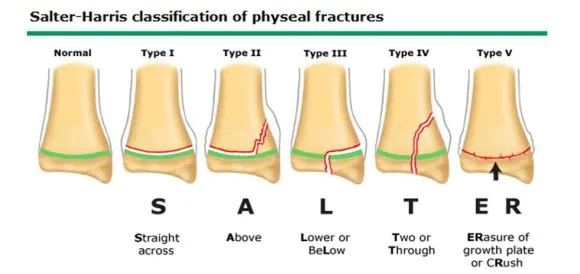
- Growth Plate Injuries: Salter-Harris 📌 SALTER: I-Slipped, II-Above, III-Lower, IV-Through, V-ERasure/cRush.
- Supracondylar Humerus Fx: Neurovascular compromise risk (Volkmann's).
- Femur Fx: Significant blood loss. Rx: spica/traction/ORIF (age-dependent).
- Compartment Syndrome: Pain out of proportion.
- Growth Plate Injuries: Salter-Harris 📌 SALTER: I-Slipped, II-Above, III-Lower, IV-Through, V-ERasure/cRush.
- Non-Accidental Trauma (NAT):
- Suspect: Inconsistent history, delay, specific patterns.
- Fractures: Posterior ribs, metaphyseal (corner/bucket-handle), sternal, scapular, spinous process; multiple, varied healing.
- Shaken Baby: Subdural hematoma, retinal hemorrhages, DAI.
- Burns: Stocking/glove, cigarette.
- Mandatory reporting.
⭐ Metaphyseal corner fractures and posterior rib fractures are highly specific indicators of non-accidental trauma in infants.
High‑Yield Points - ⚡ Biggest Takeaways
- Blunt trauma is the leading injury mechanism in children.
- Head injury is the primary cause of pediatric traumatic death.
- Suspect Non-Accidental Injury (NAI) with inconsistent history or specific patterns.
- Spleen is the most commonly injured abdominal organ in blunt trauma.
- Initial fluid: 20 mL/kg isotonic crystalloid; use Broselow tape for drug dosing.
- Unique pediatric physiology (e.g., ↑SA:V ratio) impacts trauma management.
- Consider SCIWORA (Spinal Cord Injury Without Radiographic Abnormality).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more