Neonatal Respiratory Physiology - Tiny Breaths, Big Challenges
- Transition at Birth: Crucial lung fluid clearance (vaginal squeeze, lymphatics).
- Surfactant: Reduces alveolar surface tension; produced by Type II pneumocytes.
- Deficiency leads to Respiratory Distress Syndrome (RDS).
- Production begins 24-28 weeks; mature levels by 35 weeks.
- Lecithin/Sphingomyelin (L/S) ratio >2 indicates lung maturity.
- Lung Mechanics:
- Highly compliant chest wall (cartilaginous ribs) → paradoxical movement.
- Relatively non-compliant lungs initially.
- ↑ Airway resistance (narrower airways).
- Low Functional Residual Capacity (FRC).
- Respiratory Control: Immature; prone to periodic breathing and apnea (especially if <34 weeks gestation).
- Oxygen Consumption: High, approx. $6-8 \text{ mL/kg/min}$ (double adult rate).
⭐ Neonates are obligate nose breathers and primarily diaphragmatic breathers during the first few months of life due to anatomical and physiological factors. This makes them vulnerable to nasal obstruction.
Neonatal Cardiovascular Adaptation - Heart's First Beats
- Birth: Critical switch from fetal to neonatal circulation.
- Key Hemodynamic Changes:
- Cord clamping → ↑ Systemic Vascular Resistance (SVR).
- First breath, lung expansion → ↓ Pulmonary Vascular Resistance (PVR).
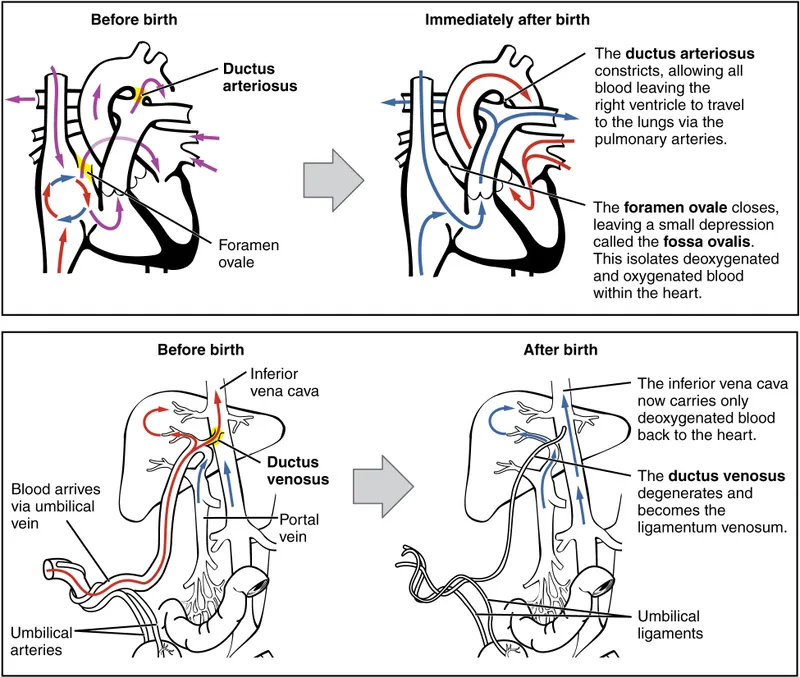
- Fetal Shunt Closure Mechanisms:
- Foramen Ovale (FO): ↑ Left Atrial Pressure (LAP) > Right Atrial Pressure (RAP) → functional closure.
- Ductus Arteriosus (DA): ↑ PaO2, ↓ Prostaglandins (PGE2) → constriction.
⭐ DA patency is PGE-dependent; Indomethacin (NSAID) promotes closure.
- Ductus Venosus (DV): Cessation of umbilical venous flow → closure.
- HR: 120-160 bpm. BP: Gradual postnatal ↑.
Neonatal Thermoregulation - Keeping Warmth Within
- High risk of hypothermia: ↑ surface area/mass ratio, ↓ subcutaneous fat, immature thermoregulation.
- Heat Loss (📌 CCRE):
- Conduction (direct contact with cold surfaces)
- Convection (air currents)
- Radiation (to cooler objects, no contact)
- Evaporation (from wet skin/respiratory tract)
- Heat Production:
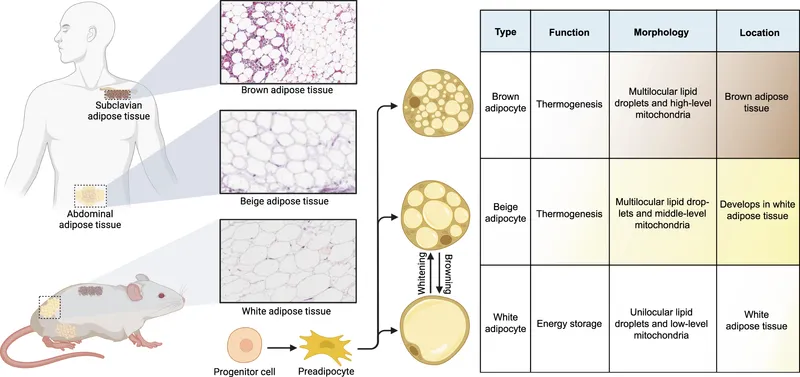
- Non-Shivering Thermogenesis (NST): Brown Adipose Tissue (BAT) is primary.
- Shivering: Minimal, poorly developed.
- Neutral Thermal Environment (NTE): Ambient temperature range (32-35°C for term neonates) minimizing O2 consumption & metabolic demand.
- Cold Stress Consequences: Hypoglycemia, metabolic acidosis, ↑O2 demand, apnea, ↓surfactant production.
⭐ Brown Adipose Tissue (BAT) is the primary site for non-shivering thermogenesis (NST), crucial for neonatal heat production due to its rich mitochondrial content.
- Prevention: Immediate drying, pre-warmed surfaces/blankets, radiant warmers, incubators, skin-to-skin contact.
 oka
oka
Neonatal Fluid, Electrolyte & Glucose Homeostasis - Balancing Act
- Fluid Balance:
- High TBW (70-80%), mainly ECF.
- Maintenance fluids (ml/kg/day): Day 1: 60-80; Days 2-7: 80-120; >7 days: 120-150.
- ↑ IWL, esp. preterm.
- Electrolytes (mEq/kg/day):
- Na+: 1-3.
- K+: 1-2.
- Ca2+: Monitor for hypocalcemia.
- Glucose Control:
- Hypoglycemia: BG < 45 mg/dL.
- GIR: Target 4-6 mg/kg/min.
- $GIR (mg/kg/min) = (% Dextrose \times IV Rate_{ml/hr}) / (6 \times Weight_{kg})$
⭐ Neonates have limited glycogen, making hypoglycemia a key risk during surgical stress.
Neonatal Gastrointestinal & Hematologic Aspects - Growth Foundations
- GI Immaturity:
- Reduced motility & enzyme activity: predisposes to NEC, feeding intolerance.
- Low Lower Esophageal Sphincter (LES) pressure: ↑Gastroesophageal Reflux (GER).
- Delayed gastric emptying.
- Gut "closure": gradual (days-weeks), affects macromolecule absorption.
- Hematologic Peculiarities:
- Physiological anemia of infancy: Hb nadir at 8-12 weeks.
- Fetal Hemoglobin (HbF) predominates: ↑O₂ affinity, left shift in ODC.
- Vitamin K: All newborns require prophylactic Vitamin K (1mg IM).
⭐ Prophylactic Vitamin K (1mg IM) is crucial for all newborns to prevent Vitamin K Deficiency Bleeding (VKDB), especially before any surgical procedure. oka
High‑Yield Points - ⚡ Biggest Takeaways
- Neonates are prone to hypothermia from large surface area/volume ratio and minimal fat.
- Higher fluid requirements (80-100 mL/kg/day) due to ↑ insensible losses and immature kidneys.
- Surfactant deficiency is key in Respiratory Distress Syndrome (RDS).
- Circulatory transition failure can result in Persistent Pulmonary Hypertension (PPHN).
- Hypoglycemia risk is high due to limited glycogen stores; monitor glucose.
- Immature liver contributes to jaundice and coagulopathy; Vitamin K is essential.
- Immature immune system increases susceptibility to sepsis.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

