Intro & Etiology - Tiny Troubles Begin
- Congenital anomalies: Structural/functional defects present at birth. Incidence: 2-3% of live births; a major cause of infant mortality.
- Classification:
- Malformations: Primary structural defect (e.g., VSD).
- Deformations: Extrinsic mechanical forces on normal tissue (e.g., clubfoot).
- Disruptions: Breakdown of previously normal tissue (e.g., amniotic bands).
- Dysplasias: Abnormal cellular organization within a tissue (e.g., skeletal dysplasia).
- Etiology:
- Genetic (~20-25%): Chromosomal (e.g., Trisomy 21), single gene.
- Environmental (~10%): Teratogens (e.g., TORCH, thalidomide, alcohol).
- Multifactorial (~20-25%): Gene-environment interactions.
- Unknown (~40-50%).
- Critical Period: Organogenesis (embryonic period, 3-8 weeks post-conception) is when susceptibility to teratogens is highest.
⭐ Most congenital malformations arise during the embryonic period (3rd-8th week of gestation), the critical window for organogenesis. oka
Key GI Anomalies - Gut Gremlins
- Esophageal Atresia (EA) & Tracheoesophageal Fistula (TEF): Most common type C (distal TEF). Polyhydramnios. Inability to pass NG tube. 📌 VACTERL association.
- Pyloric Stenosis: Non-bilious projectile vomiting at 2-8 weeks. Palpable "olive". Ultrasound: thickened pylorus (muscle >4mm, length >14mm). Hypochloremic, hypokalemic metabolic alkalosis.
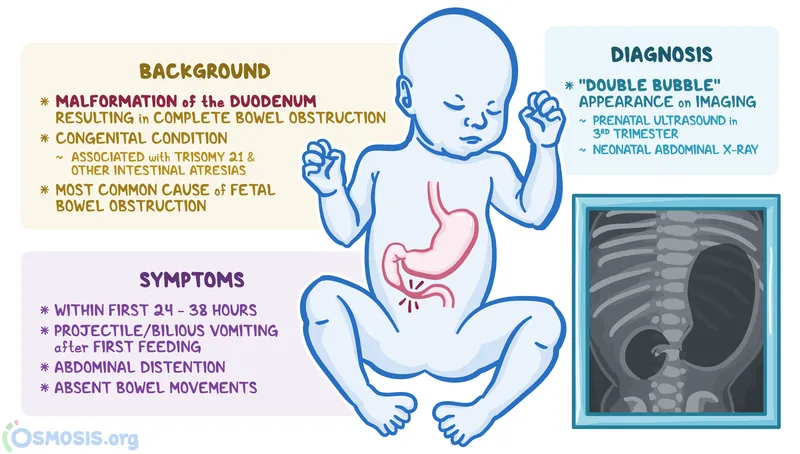
- Duodenal Atresia: Bilious vomiting. "Double bubble" sign on X-ray. Associated with Down syndrome.
- Hirschsprung's Disease: Aganglionic segment. Failure to pass meconium in 24-48 hrs. Diagnosis: rectal biopsy.
⭐ Most common site for Hirschsprung's is the rectosigmoid colon.
Abdominal Wall & Diaphragm - Outies & Innies
- Omphalocele: Midline defect at umbilicus, sac covered (amnion/peritoneum). Cord on sac. ↑Associated anomalies (cardiac, Trisomy 13/18, Beckwith-Wiedemann).
- Mgmt: Protect sac, NG tube, staged closure.
- Gastroschisis: Right paraumbilical defect, no sac. Normal cord. Exposed bowel, edematous. ↓Associated anomalies (intestinal atresia).
- Mgmt: Silo bag, NG tube, fluids, staged closure.
- Congenital Diaphragmatic Hernia (CDH): Posterolateral (Bochdalek 85%) defect. Contents in chest, severe pulmonary hypoplasia, scaphoid abdomen.
- Mgmt: Intubate, gentle ventilation, NG tube, delayed repair.

- Mgmt: Intubate, gentle ventilation, NG tube, delayed repair.
⭐ Pulmonary hypoplasia is primary determinant of CDH mortality & morbidity.
Neural Tube & CNS - Brainy Birth Bumps
- Neural Tube Defects (NTDs): Failed neural tube closure (3rd-4th week gestation).
- Anencephaly: Absent cranial vault & cerebral hemispheres.
- Encephalocele: Herniation of brain/meninges via skull defect.
- Myelomeningocele: Protrusion of meninges & spinal cord; often with Chiari II.
- Spina Bifida Occulta: Vertebral arch defect, often skin dimple or hair tuft.
- Hydrocephalus: ↑ CSF volume/pressure. Symptoms: ↑ head circumference, bulging fontanelle, sunsetting eyes.
- Communicating: Impaired CSF absorption.
- Non-communicating (Obstructive): CSF flow blockage (e.g., aqueductal stenosis).

- Chiari Malformations: Cerebellar tonsillar herniation. Type II associated with myelomeningocele.
⭐ Maternal folic acid supplementation (0.4 mg/day pre-conception & early pregnancy) significantly ↓ NTD risk.
Diagnosis & Management Principles - Spot & Sort Steps
-
Diagnosis:
- Antenatal: USG (e.g., anomaly scan 18-20 wks), maternal serum markers. Allows planning.
- Postnatal: Clinical exam, targeted imaging (X-ray, USG), genetic tests if needed.
-
Management Flow:
-
Key Principles: Multidisciplinary team, informed consent, family-centered care.
⭐ VACTERL association (Vertebral, Anal, Cardiac, Tracheo-Esophageal fistula, Renal, Limb) requires systematic screening for all components when one is identified.
High‑Yield Points - ⚡ Biggest Takeaways
- TEF: Type C most common; polyhydramnios, postnatal choking & cyanosis.
- CDH: Bochdalek (left posterolateral) most common; causes pulmonary hypoplasia.
- Pyloric Stenosis: Non-bilious projectile vomiting (2-8 wks), olive mass, hypochloremic alkalosis.
- Duodenal Atresia: Down syndrome association; bilious vomiting, double bubble sign.
- Hirschsprung's Disease: Aganglionosis (rectal biopsy); delayed meconium, rectosigmoid common.
- Omphalocele: Midline, sac present, other anomalies. Gastroschisis: Right of umbilicus, no sac.
- Malrotation with Volvulus: Neonatal bilious emesis (emergency!); Ladd's bands, corkscrew sign.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

