Intro & Patho - Blocked Bile Blues
- Progressive, idiopathic fibro-obliterative disease of neonatal extrahepatic (± intrahepatic) bile ducts.
- Results in: cholestasis → biliary cirrhosis → end-stage liver disease.
- Classic triad: persistent jaundice (conjugated), acholic stools, dark urine.
- Types:
- Embryonic/Fetal (10-20%): Jaundice from birth. Often with anomalies (e.g., BASM - Biliary Atresia Splenic Malformation).
- Perinatal/Acquired (80-90%): Jaundice develops after a few weeks. Possible viral/immune trigger.
⭐ Perinatal/acquired form (80-90%) is more common than embryonic/fetal form, typically presenting after a jaundice-free interval.
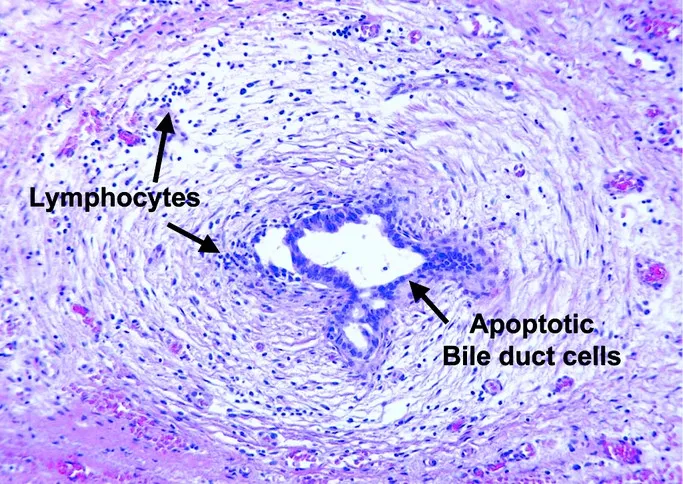
- Pathogenesis: Unknown insult (viral/immune?) → cholangiocyte damage → inflammation → progressive fibrosis & obliteration of biliary tree.
Signs & Dx - Yellow Alert Clues
Yellow Alert Clues (Clinical):
- Persistent Jaundice: >2 wks (term), >3 wks (preterm)
- Acholic Stools (pale/clay-colored)
- Dark Urine (conjugated bilirubin)
- Hepatomegaly (firm, progressive)
Diagnostic Pathway:
- Labs: ↑ Direct Bilirubin, ↑ GGT, ↑ ALP.
- Ultrasound (USG):
- Key: Triangular Cord (TC) sign (>4mm), absent/small gallbladder.
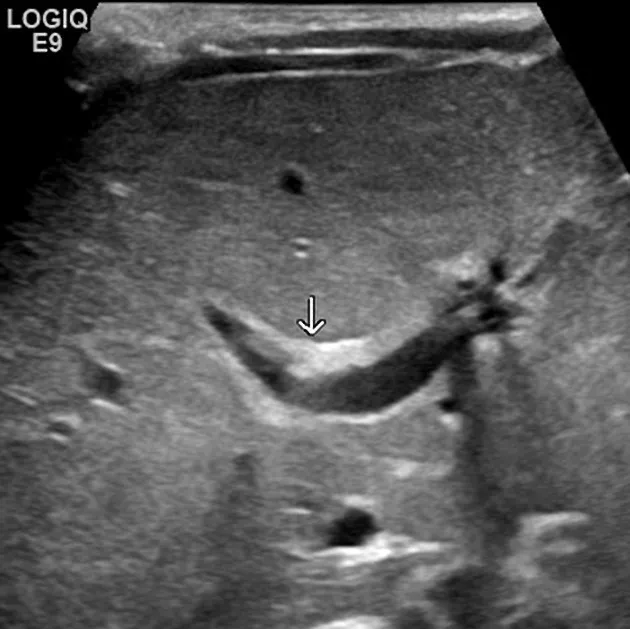
-
⭐ The 'triangular cord sign' on ultrasound (echogenic fibrous tissue anterior to portal vein) is highly suggestive of Biliary Atresia.
- HIDA Scan: (Phenobarbital x 5 days) → No gut excretion by 24 hrs.
- Liver Biopsy: Bile duct proliferation, plugs, portal fibrosis. Confirms.
- Intraoperative Cholangiogram (IOC): Definitive.
Treatment Time - Kasai's Conduit Cure
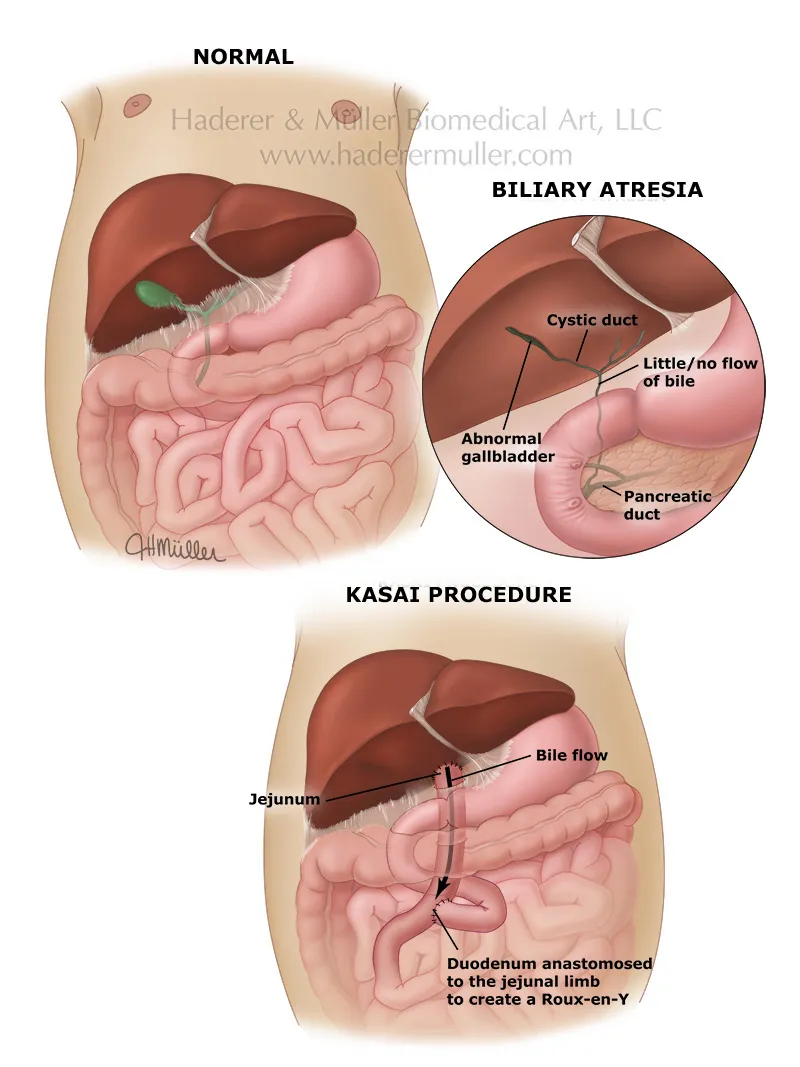
- Kasai Portoenterostomy (Hepatoportoenterostomy):
- Primary surgery; Roux-en-Y jejunal loop to porta hepatis.
- Crucial timing: Ideally before 60 days of life.
⭐ Kasai portoenterostomy performed before 60 days of life offers the best chance of bile drainage and native liver survival.
- Goal: Establish bile flow, delay cirrhosis.
- Post-Kasai Management:
- Prophylactic antibiotics (vs. cholangitis).
- Ursodeoxycholic acid (UDCA) for bile flow.
- Fat-soluble vitamins (A, D, E, K) support.
- Liver Transplantation:
- Indicated for Kasai failure or end-stage liver disease.
- Ultimate treatment for most.
 oka
oka
Outcomes & Issues - Future Flow Forecast
- Kasai Portoenterostomy:
- Success ↑ if age < 60-90 days at surgery.
- Aim: Achieve bile drainage, clear jaundice.
- Common Complications:
- ⭐ > Ascending cholangitis is the most common complication after Kasai portoenterostomy, often recurrent.
- Portal hypertension: Varices, splenomegaly.
- Fat malabsorption: Deficiencies of vitamins A, D, E, K.
- Progressive biliary cirrhosis.
- Long-Term Outlook:
- Majority require liver transplantation (LT).
- Native liver survival: ~30-50% at 5 years post-Kasai.
- Post-LT survival rates are high.
- Follow-up:
- Regular LFTs, ultrasound.
- Nutritional support (MCT oil, fat-soluble vitamins).
- UDCA, prophylactic antibiotics (variable use).
High‑Yield Points - ⚡ Biggest Takeaways
- Persistent neonatal jaundice (>2 weeks), acholic stools, dark urine, and hepatomegaly are cardinal signs.
- Key lab findings: ↑ conjugated bilirubin and significantly ↑ serum GGT.
- Intraoperative cholangiogram is the gold standard for diagnosis.
- Kasai portoenterostomy (hepatoportoenterostomy) is the initial surgical intervention, ideally performed before 60-90 days of age.
- Liver transplantation is often required for failed Kasai or late diagnosis.
- Frequently associated with polysplenia syndrome (Biliary Atresia Splenic Malformation - BASM).
- Type III (atresia at the porta hepatis) is the most common anatomical variant (>90%).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

