Introduction & Anatomy - Pancreas Under Pressure
- Pancreatic trauma: Rare (<5% abdominal injuries), but high morbidity/mortality (~20-30%).
- Retroperitoneal organ; vulnerable to crushing force against vertebral column.
- Head: C-loop of duodenum, CBD, GDA.
- Neck: Overlies SMV/portal vein.
- Body/Tail: Splenic vessels, proximity to left kidney/spleen.
- Main pancreatic duct (Wirsung): Critical for exocrine function; injury dictates management.
- Mechanisms: Blunt (MVCs, direct blow) > Penetrating (GSW, stab).
- Associated injuries common (>80%), complicating diagnosis & management.
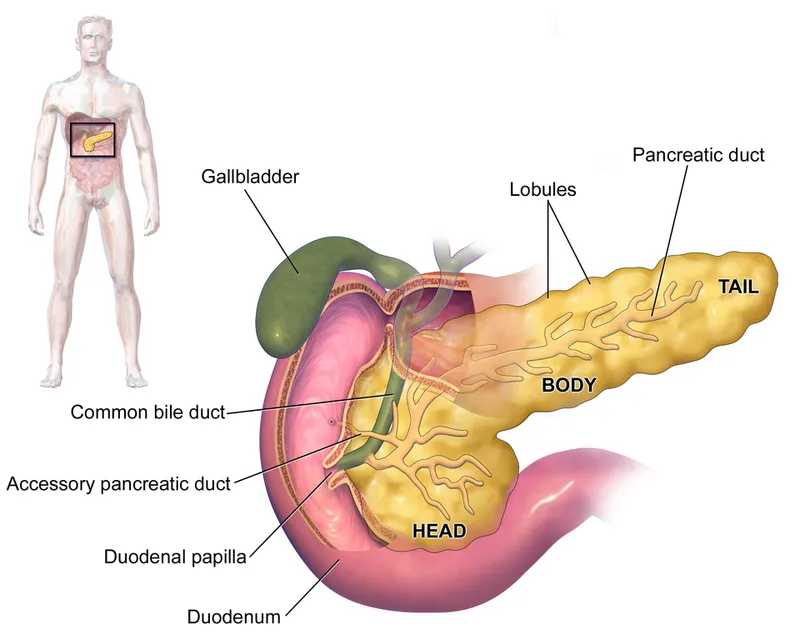
⭐ The majority of pancreatic injuries (~60-70%) occur in the body and tail due to their anterior position relative to the vertebral column and less protection compared to the head embedded in the duodenum.
- Delayed diagnosis is a key factor for ↑ complications (pseudocyst, fistula, abscess).
Classification & Diagnosis - Spotting the Damage
- AAST Pancreatic Injury Scale (OIS): Standard for grading injury severity.
- Grade I: Minor contusion/laceration; capsule intact; no duct injury.
- Grade II: Major contusion/laceration; capsule breached; no duct injury or major tissue loss.
- Grade III: Distal transection or parenchymal injury with duct injury.
- Grade IV: Proximal transection (right of SMV) or parenchymal injury involving ampulla; with duct injury.
- Grade V: Massive disruption of pancreatic head (shattered pancreas); devascularization.
⭐ AAST Grade III and higher injuries (main pancreatic duct involvement) usually necessitate operative intervention or endoscopic stenting.
- Clinical Clues: Epigastric pain/tenderness post-trauma (e.g., handlebar, direct blow).
- Lab Markers:
- Serum Amylase/Lipase: ↑Lipase more specific & sensitive. Can be normal initially; serial values key.
- Imaging Modalities:
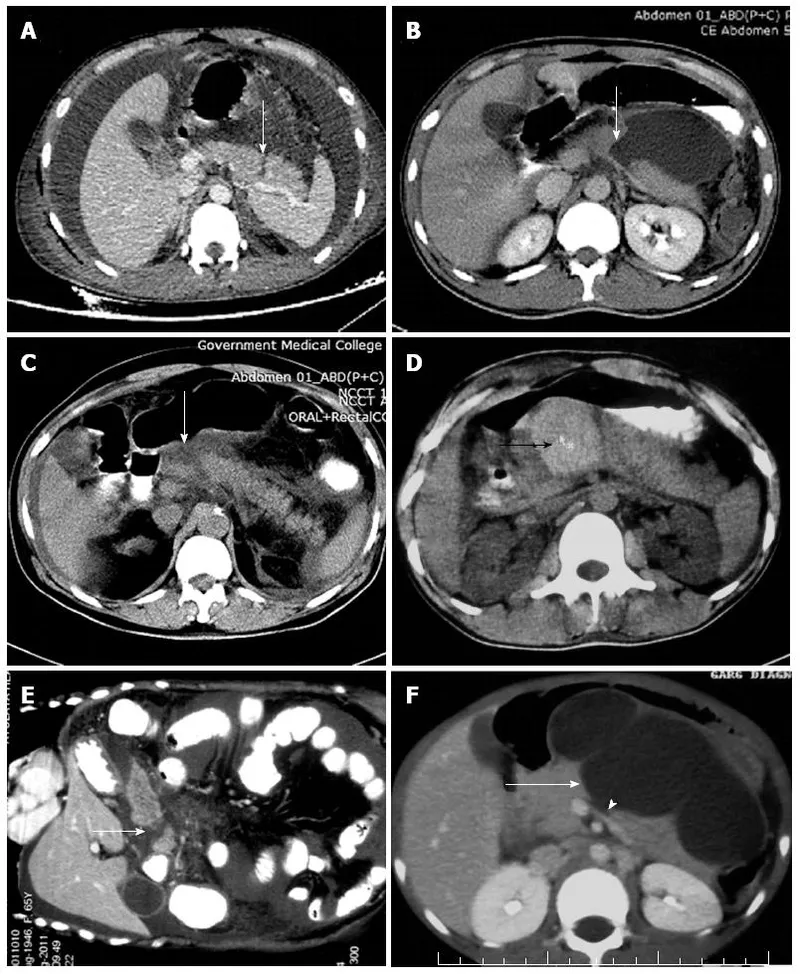
- CECT Abdomen: Primary diagnostic tool in hemodynamically stable patients.
- Findings: Gland laceration, hematoma, peripancreatic fluid, transection.
- Delayed scan (6-8h) may improve duct visualization.
- MRCP (Magnetic Resonance Cholangiopancreatography): Superior for delineating ductal anatomy if CECT is equivocal or high suspicion of duct injury.
- ERCP (Endoscopic Retrograde Cholangiopancreatography): Gold standard for diagnosing duct injury; offers therapeutic potential (e.g., stenting).
- CECT Abdomen: Primary diagnostic tool in hemodynamically stable patients.
Management Principles - Fixing the Break
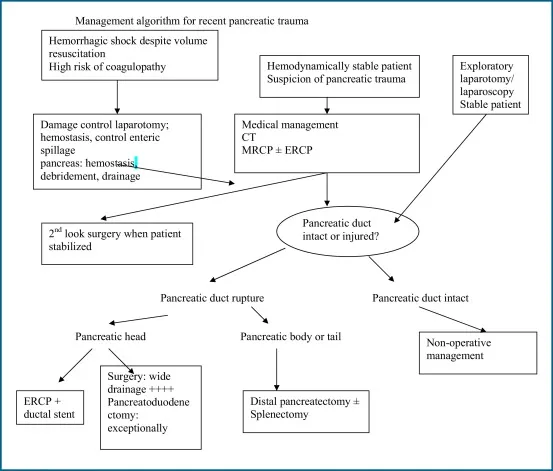
- Initial: ABCDEs.
- Non-Operative Management (NOM):
- Criteria: Stable, AAST Grade I/II, no major duct injury.
- Care: Observe, NPO, IV fluids, analgesia. ERCP + stent for minor leaks.
- Operative Management (OM):
- Indications: Unstable, peritonitis, AAST Grade III-V, major duct injury, NOM failure.
- Goals: Control bleeding, debride, manage duct, drain.
- Procedures:
- Grade I/II (no duct): Drainage, suture.
- Grade III (body/tail, duct): Distal pancreatectomy (± splenectomy).
⭐ Distal pancreatectomy: most common resection in pancreatic trauma.
- Proximal/Complex (duct): Roux-en-Y pancreaticojejunostomy.
- Grade V (head): Whipple (rare); damage control first.
- Drainage: Essential; closed-suction drains.
- Damage Control: For unstable; staged surgery.
Complications & Prognosis - Aftermath & Outlook
- Early Complications:
- Pancreatic fistula (most common, ~20-40%)
- Intra-abdominal abscess, sepsis
- Hemorrhage (e.g., pseudoaneurysm)
- Acute post-traumatic pancreatitis
- Late Complications:
- Pancreatic pseudocyst (Acute Peripancreatic Fluid Collection if <4 wks, pseudocyst if >4 wks)
- Chronic pancreatitis
- Exocrine/Endocrine insufficiency (diabetes)
- Prognosis:
- Mortality: 5-30%; ↑ with ductal/vascular injury.
- Morbidity: Mainly fistula, abscess.
- Higher AAST grade predicts worse outcomes.
⭐ Pancreatic fistula is the most frequent complication post-pancreatic trauma, often managed conservatively but may need drainage.
High‑Yield Points - ⚡ Biggest Takeaways
- Blunt abdominal trauma is the most common etiology.
- Delayed presentation is characteristic due to retroperitoneal location.
- Serum amylase/lipase can be unreliable initially; serial monitoring is key.
- Contrast-enhanced CT (CECT) is the primary diagnostic tool.
- ERCP is crucial for evaluating main pancreatic duct (MPD) injury.
- Management is dictated by hemodynamic stability and pancreatic duct status.
- Operative repair or resection (e.g., distal pancreatectomy, Whipple) for severe injuries with duct involvement or instability.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

