Gross Anatomy - Pancreas Unveiled: Prime Position
- Location: Primarily retroperitoneal (except tail); epigastrium & left hypochondrium (L1-L2 vertebrae).
- Parts & Relations:
- Head: Cradled by C-loop of duodenum. Uncinate process hooks posterior to Superior Mesenteric Vein (SMV) & Artery (SMA).
- Neck: Overlies SMV, portal vein formation.
- Body: Crosses aorta, L2 vertebra; posterior to stomach.
- Tail: Reaches splenic hilum; only intraperitoneal part. 📌 Mnemonic: "Tail In Peritoneum" (TIP).
- Arterial Supply:
- Head/Uncinate: Superior (from Gastroduodenal Artery) & Inferior (from SMA) pancreaticoduodenal arteries.
- Body/Tail: Splenic artery branches.
- Venous Drainage: Parallels arteries; drains to portal system (SMV, splenic vein).

⭐ The uncinate process of the pancreas passing posterior to the superior mesenteric vessels (SMV and SMA) is a critical surgical landmark and a common site for tumor involvement affecting resectability.
Vascular & Ductal System - Red Rivers & Duct Tales
Arterial Supply:
- Pancreaticoduodenal Arcades: Key anastomotic loops.
- Superior Pancreaticoduodenal A. (SPDA): from Gastroduodenal A. (GDA ← Celiac Trunk)
- Inferior Pancreaticoduodenal A. (IPDA): from Superior Mesenteric A. (SMA)
- Splenic Artery Branches: (Supply body/tail)
- Dorsal Pancreatic A.
- Great Pancreatic A. (Arteria Pancreatica Magna)
- Caudal Pancreatic A.
Venous Drainage: (Generally mirrors arterial supply)
- Pancreaticoduodenal Veins → drain into Superior Mesenteric Vein (SMV) / Portal Vein (PV)
- Splenic Vein + SMV = Portal Vein (forms posterior to pancreatic neck)
Ductal System:
- Main Pancreatic Duct (Wirsung):
- Runs tail → head; joins Common Bile Duct (CBD) → forms Ampulla of Vater.
- Opens at Major Duodenal Papilla (2nd part of duodenum).
- Diameter: Head ~3mm, Body ~2mm, Tail ~1mm (📌 3-2-1 Rule).
- Accessory Pancreatic Duct (Santorini):
- Drains superior/anterior part of head; opens at Minor Duodenal Papilla.
- Pancreas Divisum: Commonest congenital anomaly; failure of ventral & dorsal duct fusion.

⭐ The Portal Vein is formed by the confluence of the Splenic Vein and Superior Mesenteric Vein (SMV) posterior to the neck of the pancreas, a critical surgical landmark during pancreatectomy.
Histo & Exocrine Role - Cell City & Enzyme Elixir
- Histology - The "Cell City":
- Acinar cells: Pyramidal, house zymogen granules (inactive enzyme precursors).
- Centroacinar cells: Pale cells at duct origin within acinus; secrete bicarbonate.
- Ductal cells: Cuboidal; secrete large volumes of bicarbonate-rich fluid.
- Exocrine Function - The "Enzyme Elixir":
- Daily secretion: 1.5-3 L of alkaline pancreatic juice (pH ~8).
- Key Enzymes:
- Proteolytic: Trypsinogen, Chymotrypsinogen.
- Lipolytic: Lipase, Colipase.
- Amylolytic: Amylase.
- Bicarbonate ($HCO_3^-$): Neutralizes acidic chyme from stomach.
- Primary Stimulators:
- Cholecystokinin (CCK): ↑ Enzyme release from acini.
- Secretin: ↑ $HCO_3^-$ and water secretion from ducts.

⭐ Trypsinogen is activated to trypsin by duodenal enterokinase (enteropeptidase). Trypsin then auto-catalyzes more trypsinogen and activates other zymogens (e.g., chymotrypsinogen to chymotrypsin), a critical step preventing pancreatic auto-digestion.
Endocrine Role & Embryology - Sugar Bosses & Budding Beginnings
- Islets of Langerhans (Endocrine Pancreas): Scattered cell clusters.
- β-cells (60-70%): Insulin (↓ blood glucose), Amylin.
- α-cells (20-25%): Glucagon (↑ blood glucose).
- δ-cells (5-10%): Somatostatin (inhibits insulin, glucagon, GH).
- PP/γ-cells (1-2%): Pancreatic Polypeptide (inhibits exocrine secretion, gallbladder contraction).
- 📌 Mnemonic: Inside Beta, Glucagon Around (Insulin by Beta cells in center, Glucagon by Alpha cells in periphery).
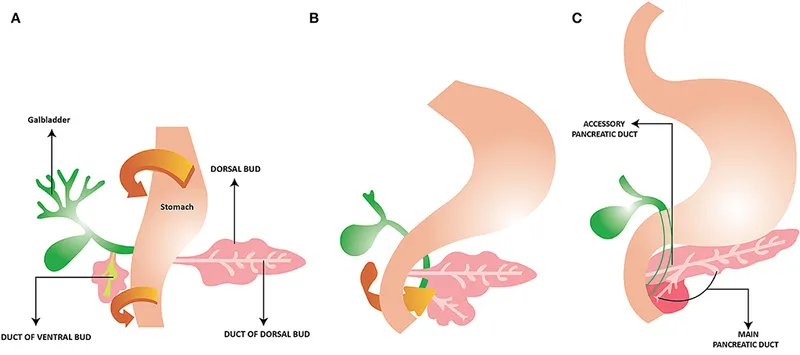
- Embryology: Dual origin from foregut endoderm.
- Dorsal bud → Superior head, body, tail.
- Ventral bud → Inferior head, uncinate process.
- Rotation & fusion by 5th-7th week gestation.
- Duct of Wirsung (main): Ventral duct + distal dorsal duct.
- Duct of Santorini (accessory): Proximal dorsal duct.
⭐ Annular pancreas, a congenital anomaly, results from failure of complete migration and fusion of the ventral bud, potentially causing duodenal obstruction.
High‑Yield Points - ⚡ Biggest Takeaways
- Head of pancreas in duodenal C-loop; tail at splenic hilum.
- Main duct (Wirsung) joins CBD at ampulla of Vater; regulated by sphincter of Oddi.
- Accessory duct (Santorini) opens at minor papilla, superior to major.
- Arterial supply: Celiac trunk (gastroduodenal, splenic arteries) & SMA (inferior pancreaticoduodenal).
- Endocrine: Islets produce Insulin (β-cells), Glucagon (α-cells), Somatostatin (δ-cells).
- Exocrine: Acinar cells secrete digestive zymogens (amylase, lipase, proteases).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

