Etiology & Pathophysiology - Ignition & Inferno
- Common Causes (Ignition):
- Gallstones (most common, ~40%): Ampullary obstruction.
- Alcohol (~30%): Acinar cell sensitization, premature enzyme activation.
- Hypertriglyceridemia (TG > 1000 mg/dL).
- Post-ERCP.
- Drugs (e.g., thiazides, azathioprine, valproate).
- 📌 Other causes: I GET SMASHED (mnemonic for less common etiologies like Idiopathic, Trauma, Steroids, Mumps, Autoimmune, Scorpion sting, Hypercalcemia, etc.).
- Pathophysiology (Inferno):
- Core Defect: Intra-acinar premature activation of trypsinogen to trypsin.
- Autodigestion: Activated enzymes (trypsin, chymotrypsin, elastase, phospholipase A2) digest pancreas & peripancreatic tissues.
- Inflammatory Cascade: Release of cytokines (TNF-α, IL-1, IL-6) → local inflammation, edema, necrosis, hemorrhage.
- Systemic Impact: Can lead to Systemic Inflammatory Response Syndrome (SIRS), ARDS, renal failure, multi-organ failure (MOF).
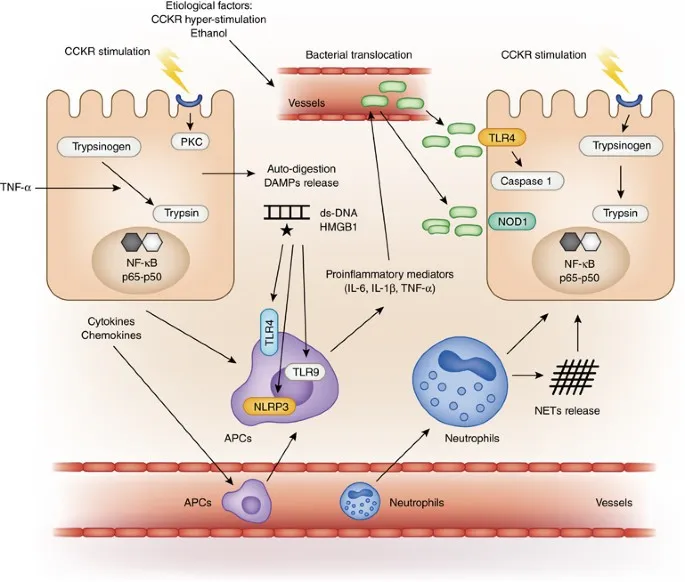
⭐ Trypsinogen activation within acinar cells, not primarily in the ductal system, is the critical initiating event in most cases of acute pancreatitis leading to autodigestion and inflammation.
Clinical Features & Diagnosis - Spotting the Sizzle
- Symptoms:
- Abdominal Pain: Severe, constant epigastric, radiates to back; sudden onset.
- Nausea & Vomiting.
- Fever, tachycardia.
- Signs:
- Epigastric tenderness.
- Cullen's sign (periumbilical ecchymosis).
- Grey Turner's sign (flank ecchymosis) - indicates severe disease.
- Diagnostic Criteria (Need ≥2 of 3):
- Characteristic abdominal pain.
- Serum amylase and/or lipase >3x upper limit of normal (ULN).
- Characteristic findings on imaging (US, CT, MRI).
- Key Investigations:
- Labs: ↑Amylase, ↑Lipase (more specific), ↑WBC, ↑CRP, ↓Ca.
- Imaging: US (initial, for gallstones); CECT Abdomen (gold standard for severity/necrosis, after 48-72h if severe).

⭐ Serum lipase is more specific and remains elevated longer than amylase in acute pancreatitis.
Severity Assessment & Prognosis - Measuring the Mayhem
- Objective: Stratify risk for severity, organ failure (OF), mortality.
- Scoring Systems:
- Ranson's Criteria: Admission & 48h. 📌 "GA LAW", "C HOBBS". Score ≥3 = severe AP.
- BISAP: <24h. (BUN >25 mg/dL, Imp. mental status, SIRS, Age >60 yrs, Pleural Effusion). Score ≥3 = ↑ mortality.
- APACHE II: ICU standard, complex.
- Mod. Marshall: Defines OF (Resp, Renal, CV); score ≥2/system = OF.
- CTSI (CT Severity Index): Balthazar grade + Necrosis. Max 10 (score ≥7 severe).
- Atlanta Classification (Revised):
- Mild: No OF, no local/systemic complications.
- Mod. Severe: Transient OF (<48h) OR local/systemic complications without persistent OF.
- Severe: Persistent OF (>48h).
⭐ Persistent organ failure (>48h) is key determinant of severe AP.
Management & Complications - Dousing & Dealing
- Initial Management (First 24-72h):
- Fluid Resuscitation: Aggressive IV crystalloids (Lactated Ringer's, 5-10 mL/kg/hr bolus, then 250-500 mL/hr). Target: UOP >0.5 mL/kg/hr, ↓HR, ↓Hct.
- Pain Control: IV opioids (fentanyl, hydromorphone).
- Nutrition: Mild AP: early oral low-fat diet. Severe AP: early enteral nutrition (nasojejunal) if NPO >3-5 days.
- Specific Interventions:
- Antibiotics: NOT prophylactic. For infected necrosis (carbapenems). Diagnose by CT-FNA or gas on CT.
⭐ Prophylactic antibiotics do not prevent infection and may increase fungal superinfections.
- ERCP: Within 24h for severe gallstone pancreatitis + cholangitis; within 72h if biliary obstruction.
- Antibiotics: NOT prophylactic. For infected necrosis (carbapenems). Diagnose by CT-FNA or gas on CT.
- Complications & Management:
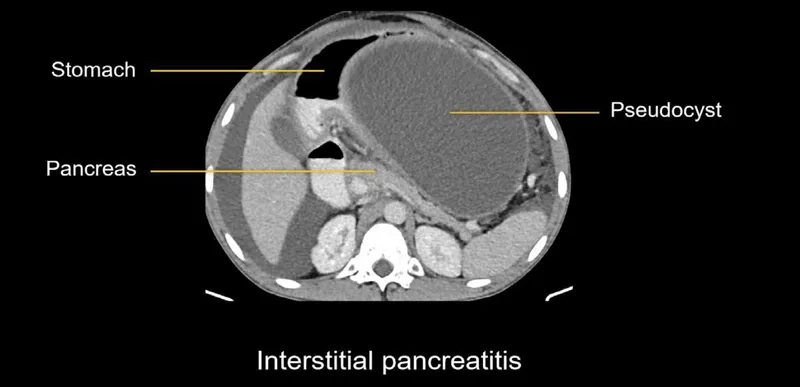
- Local: Pseudocyst (>4 wks): Drain if symptomatic, >6 cm, or complicated. Walled-Off Necrosis (WON) (>4 wks): Step-up approach (drainage then necrosectomy) if infected/symptomatic.
- Systemic: ARDS, AKI, SIRS, MODS, hypocalcemia.
High‑Yield Points - ⚡ Biggest Takeaways
- Gallstones and alcohol are the most common etiological factors for acute pancreatitis.
- Serum lipase is a more specific and sensitive diagnostic marker than serum amylase, remaining elevated longer.
- Severity assessment is critical using scores like Ranson's criteria or APACHE II.
- Contrast-Enhanced CT (CECT) is the imaging modality of choice for detecting necrosis and complications.
- Initial management focuses on aggressive intravenous fluid resuscitation, analgesia, and bowel rest (NPO).
- Infected pancreatic necrosis is a life-threatening complication requiring antibiotics and often surgical debridement.
- Pancreatic pseudocyst is a common late complication, typically managed if symptomatic or large.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

