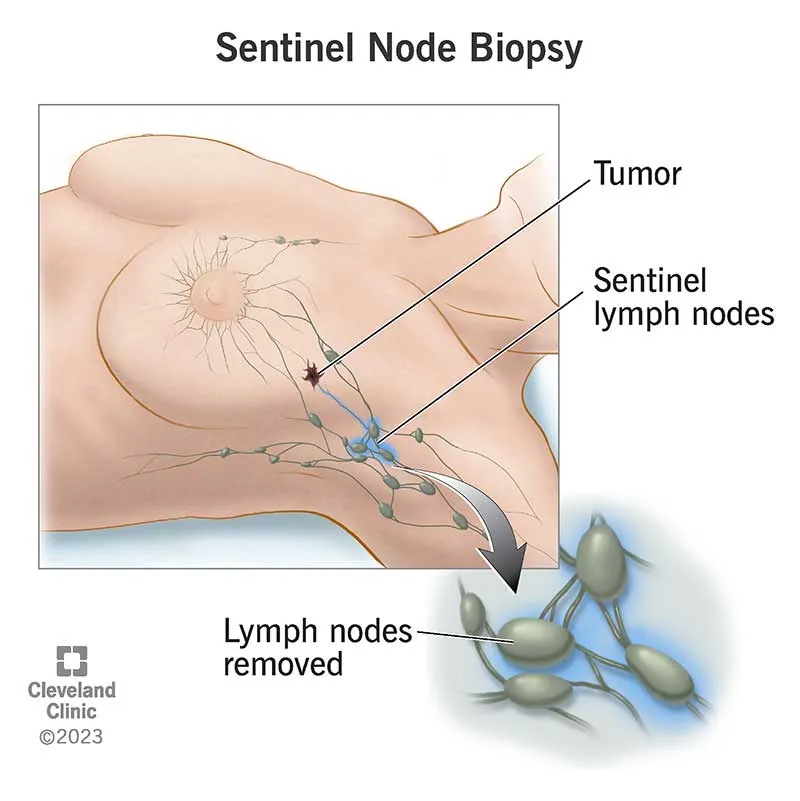
Sentinel Lymph Node Concepts - Node Navigator Intro
- Sentinel Lymph Node (SLN) Definition: The first lymph node(s) that directly receives lymphatic drainage from a primary tumor. Its histological status predicts the status of other regional nodes.
- Principle of SLN Biopsy (SLNB):
- Involves identifying, removing, and examining the SLN(s).
- A negative SLN suggests other nodes in the basin are also free of metastasis, potentially avoiding more extensive surgery.
- Rationale for SLNB:
- Accurate Staging: Crucial for determining cancer stage and guiding adjuvant therapy.
- Reduced Morbidity: Avoids unnecessary complete lymph node dissection, thus minimizing risks like lymphedema and nerve injury.

⭐ The sentinel lymph node is the first lymph node(s) to receive lymphatic drainage from a primary tumor.
Sentinel Lymph Node Concepts - Mapping the Messengers
SLNs: first nodes draining a tumor; key for staging, minimizing lymphadenectomy.
- Tracers & Detection:
Tracer Type Detection Pros Cons Blue Dyes Visual Visual Inexpensive, simple Allergic reactions, tattooing, ↓ solo rate Radiocolloid Radioactive Gamma probe High detection, objective Radiation, cost, facility needs ICG Fluorescent NIR camera High detection, real-time visual Cost, special equipment - Radiocolloid details: Technetium-99m, particle size 200-1000 nm, dose 0.1-1.0 mCi.
- Combined Technique: Blue dye + radiocolloid preferred for ↑ accuracy. (📌 Mnemonic: "Blue Radio is AccuRate Duo")
- Injection Sites: Peritumoral, intratumoral, subdermal, intraparenchymal.
- Detection Methods: Gamma probe (radiocolloid), visual (blue dye), NIR imaging (ICG).
⭐ The combination of blue dye and radiocolloid (dual technique) offers the highest localization rates for SLNB.
Sentinel Lymph Node Concepts - When Nodes Nod Yes
- Indications:
- Breast Cancer: Clinically node-negative (cN0) invasive carcinoma (typically T1-T2 stages).
- Melanoma: Breslow depth >1mm, or >0.8mm with ulceration or high mitotic rate (key prognostic factors).
- Other Uses: Penile, vulvar, cervical, and select head & neck cancers.
- Contraindications:
- Clinically positive/palpable nodes (cN+).
- Inflammatory breast cancer.
- Prior extensive axillary surgery/radiotherapy (relative).
- Known allergy to mapping tracer (e.g., blue dye, radiocolloid).
⭐ SLNB is the standard of care for axillary staging in clinically node-negative, early-stage invasive breast cancer, reducing ALND-related morbidity.
Sentinel Lymph Node Concepts - Decoding the Dispatch
- SLN: First lymph node(s) draining a tumor; predicts regional spread.
- Interpretation:
- Positive SLN: Tumor cells present.
- Negative SLN: No tumor cells; often spares Axillary Lymph Node Dissection (ALND).
- Implications:
- Positive SLN: Traditionally ALND; see Z0011 nuances in flowchart.
- Negative SLN: Observation/adjuvant therapy.
- False Negative Rate (FNR): Risk of negative SLN despite positive non-sentinel nodes. Acceptable FNR <5-10%.
- Key Trials:
- ACOSOG Z0011: Early breast Ca (T1-T2, 1-2 +ve SLNs, BCT, WBRT).
- MSLT-I/II: Melanoma staging & management.
- ALND Complications (spared by SLNB): Lymphedema, pain, seroma.
⭐ ACOSOG Z0011: In T1-T2 breast cancer with 1-2 positive SLNs, undergoing BCT, WBRT & systemic therapy, ALND isn't superior to SLNB alone for survival.
High‑Yield Points - ⚡ Biggest Takeaways
- Sentinel Lymph Node (SLN): The first lymph node receiving tumor drainage.
- Tracers: Blue dye (Isosulfan/Methylene) and Technetium-99m sulfur colloid.
- Gamma probe used for intraoperative localization of radiolabeled SLN.
- SLNB stages breast cancer & melanoma, potentially avoiding full lymphadenectomy.
- A negative SLN strongly suggests other regional nodes are clear.
- False-negative rate (5-10%) is a key limitation; technique dependent.
- Indications: Clinically N0 breast cancer, melanoma (>1mm depth or specific features).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more